














|
 |
| |

 |
|
 |
 hat
is leadership? According to Webster’s dictionary, there’s
no one answer. The root word “lead” can mean “to
guide someone or something along the way,” “to direct
the operations, activity, or performance of,” or “to
be first.” hat
is leadership? According to Webster’s dictionary, there’s
no one answer. The root word “lead” can mean “to
guide someone or something along the way,” “to direct
the operations, activity, or performance of,” or “to
be first.”
Across the country and around the
world, Emory nursing alumni are defining leadership in various ways.
From Georgia, Texas, Virginia, Eastern Europe, and beyond, several
have put their institutions on the nursing education road map as
deans and directors of schools of nursing. In each locale, they
are shaping future nurses and piloting their schools in ways that
enhance nursing education, research, and practice at home and abroad. |
 |
| |
|
|
 |
A
Texas-size legacy

|
 |
 |
 ouston
is a Texas-size metropolis, where it’s easy to get lost in
the sprawl of the world’s largest medical center. That hasn’t
happened to Dr. Patricia Starck, 60N, 63MN, who has made a definite
mark in her adopted state during her 20-year tenure as dean of the
University of Texas School of Nursing. ouston
is a Texas-size metropolis, where it’s easy to get lost in
the sprawl of the world’s largest medical center. That hasn’t
happened to Dr. Patricia Starck, 60N, 63MN, who has made a definite
mark in her adopted state during her 20-year tenure as dean of the
University of Texas School of Nursing.
Creating nurse-clinic partnerships
involving nursing faculty and local businesses has moved the school
into the forefront of community health. The University of Texas
Health Services is a nurse practitioner-run clinic offering primary
care and occupational health services outreach to employees at 41
businesses and industries, including major oil companies and the
Houston branch of The Coca-Cola Company.
|
 |
| |
 |
|
 |
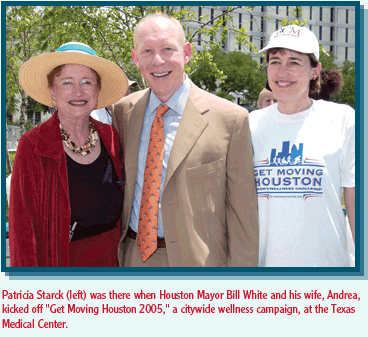 |
 |
| |
 |
|
| |
In
2004, U.S. News & World Report rated UT School of Nursing among
the top 10% of graduate nursing schools in the nation. For Starck,
the national accolade ranks right up there with the clinic, which
is her pride and joy. “The school is just 33 years old. We
are a very young school to have achieved what we have, and I’m
very proud of that,” says Starck, who also serves as John
P. McGovern Distinguished Professor.

One aspect of the clinic program includes
teaching nurse practitioners the business side of running a practice.
That has paid off. “Unlike many health care practices, clinics
run by nurse practitioners come out in the black,” she adds.
The school’s recognition is
hard won and reflects strategic planning that added a doctoral nursing
program 10 years ago and focused on building a strong research program.
Maintaining the school’s momentum is tough work. “One
of our biggest challenges is to keep everyone motivated and passionate
about our mission [in the face of] more federal regulations and
more compliance issues as well as shrinking resources and increasing
needs,” says Starck.
Last year, the nursing faculty moved
into a new $58 million building. UT’s School of Nursing and
Student Community Center has received several architectural green
awards for its environmentally friendly design and its educationally
advanced technology. The building and the UT clinic are just part
of Starck’s legacy as dean and a career spanning more than
35 years of social and technological change.
She credits her Emory experience as
pivotal in her decision to pursue an education track in nursing.
After enrolling in the late 1950s, she sought guidance from Ruth
Brice, then-faculty adviser for rehabilitation nursing.
“I loved all nursing and couldn’t
decide what specialty I wanted,” says Starck. “My intent
was to choose a nurse administrator track, since I loved hospital
nursing. But she wisely said that I could still be a nurse administrator
if I chose the nurse education track, but I couldn’t teach
with an administrator track.” Starck chose the latter and
never looked back.
Reared in Americus, Georgia, in the
segregated South, Starck was part of Emory’s first integrated
nursing class in 1963. Despite upheaval in the state over integration,
the students in her graduate class “immediately bonded,”
recalls Starck, who served as nursing program director at Albany
State College (now Albany State University), a historically black
college. She took the job in 1971, after teaching for several years
at Georgia Baptist College of Nursing in Atlanta (where Dr. Susan
Gunby, 77MN, is now dean) and at Georgia Southwestern (which she
attended prior to Emory) in Americus.
In contrast to the student population
during her first years as a nursing educator, students today are
no longer fresh out of high school, and their aspirations are more
defined.
“Many of them have degrees in
other fields and are coming into nursing, and they are going to
solve a lot of the health care system problems that we were unable
to solve,” Starck says. “They’re bright, motivated,
and energetic. I’m optimistic about the future of nursing
being in their hands.” |
|
| |
 |
|
 |
Growing
a mission

|
 |
 |
 r.
Nancy Langston, 72MN, thought she had plotted her definitive career
path when she arrived at Virginia Commonwealth University (VCU)
in 1991. r.
Nancy Langston, 72MN, thought she had plotted her definitive career
path when she arrived at Virginia Commonwealth University (VCU)
in 1991.
With terms as professor and dean of
nursing at the University of North Carolina–Charlotte and
as associate dean at the University of Nebraska Medical Center College
of Nursing, Langston believed she should not overstay her welcome
at VCU.
She likes to tell colleagues, “I
came here for 10 years—14 years ago,” she says. “I
thought I would need to make at least one more career move. I believe
a dean truly can stay too long.” Nonetheless, after 14 years
at VCU, she remains energized by the students and faculty and what
they have achieved.

|
 |
 |
 |
 |
| |
 |
|
| |
Soon
after arriving in Richmond, Langston began setting the faculty’s
sights on bolstering the school’s research funding from the
National Institutes of Health. She was appreciative of their can-do,
collaborative spirit. “We set our focus on becoming a research-intensive
school of nursing,” Langston says.
That focus was unveiled in a strategic
plan in 1997, with the goal of becoming one of the nation’s
top 25 nursing schools in NIH research funding in 10 years.
“At that time, the school ranked
81st in the nation in NIH grant funding with a single $300,000 NIH
grant,” she says. But reaching the top 25 seemed an approachable
target and in line with the school’s mission.
“We have a strong, clinical-oriented
faculty, and they developed programs with clinical research consistent
with the NIH’s national agenda,” Langston adds. “Our
faculty embraced this and created a climate to support our researchers
and research.”
In 2005, the school rose to 14th in
the nation (up from 25th in 2004, when it reached its goal three
years early), with more than $2.7 million in NIH funding achieved
through the work and initiative of five nurse/faculty researchers.
Not content to rest on their laurels, the faculty’s research-building
continues. Many of their projects focus on healing, risk and resilience,
immunocompetence, and biobehavioral clinical research.
“Our research is really patient-focused,”
Langston says. Examples range from nursing interventions such as
providing immediate oral care to decrease ventilator-associated
pneumonia in patients with traumatic injury who require intubation—a
study highly relevant to caring for soldiers injured on the battlefield—to
complementary medicine methods using tai chi and meditation to reduce
stress and boost immunity in HIV/AIDS patients.
Improving patient care through the
education of nurses has long been Langston’s passion and focus.
As with their research, the faculty have developed innovative educational
programs that provide multiple points of entry for undergraduate
and graduate education. They have developed a BS to MS program for
college graduates in other fields, an RN to MS program for those
with associate degrees, and, most recently, a fast-track BS to PhD
program. Educating nurses is the motivation behind Langston’s
involvement with the National League for Nursing, for which she
served as president from 1999 to 2000. (Emory nursing professor
Joyce Murray is the current president). She is now a board member
and chairs the organization’s Foundation for Nursing Education,
which she helped initiate.
Like many a nursing student,
Langston originally planned to be a staff nurse. Just over a year
after finishing the BSN program at the University of Arkansas, she
accepted her first faculty position and has been hooked on teaching
ever since. Her only regret: the failure of nursing education to
work collaboratively with nursing services to establish practice
differentiation in the workplace.
“A graduate of a two-year program
has a different knowledge base than a graduate of a four-year program,
yet we have not made progress in understanding that what those nurses
do should be different,” she explains.
The rewards of her career outweigh
the challenges. Langston teaches freshmen nursing students and advises
the VCU student nursing association chapter. Her students’
attitude toward the profession heartens her. “They really
have that important value of caring. It is our responsibility to
nurture that caring while helping them gain the knowledge and skills
that enable them to be competent nurses who express that competence
in and through caring.”
Langston plans to “overstay
her welcome” as dean a while longer. In June, the nursing
school broke ground for a new building. It is slated to open in
2007.
 |
|
| |
|
|
 |
Dispelling
stereotypes

|
 |
 |
 hat
do nurses know about pain management and suffering? When Dr. Susan
Gunby, 77MN, dean of Georgia Baptist College of Nursing of Mercer
University in Atlanta, began researching the topic 33 years ago,
she found one book on the subject and little else. hat
do nurses know about pain management and suffering? When Dr. Susan
Gunby, 77MN, dean of Georgia Baptist College of Nursing of Mercer
University in Atlanta, began researching the topic 33 years ago,
she found one book on the subject and little else.
The lack of research energized Gunby
to begin a career-long study of nurses’ understanding of pain
and suffering. It also became a regular part of the curriculum she
taught beginning students during their first year at Georgia Baptist.

|
 |
| |
|
|
| |
“Some
of my colleagues said beginning students do not understand pain
and do not have the life experience to understand what patients
are going through,” she says. “So every time I taught
the course, I would do research with my students on the topic.”
Her research helped focus her lectures.
Over the years, she learned that many of her students did know about
pain and suffering through shared family experiences but were often
uncertain about how to translate those experiences into patient
care. That realization led Gunby to study ethical dilemmas confronting
nurses as they cared for patients.
“One theme that came out of
my research with nursing students and RNs is what I call ‘standing
inside and standing outside.’ They wanted to stand inside
and be with the person who was suffering, yet they needed to distance
themselves and stand outside to preserve their own emotional health.”
Ironically, in October 2001, Gunby
learned firsthand about pain and suffering when she was involved
in a serious accident on her motorcycle. She suffered multiple fractures
in her right leg and hand, a fractured pelvis, and severe chest
and cardiac contusions. She spent more than five months in a wheelchair.
In December 2004, Gunby underwent knee reconstruction—her
fifth surgery.
Although the accident slowed her down,
it did not diminish her life’s passions. Her husband, Tom,
had a Harley-Davidson modified so she could continue riding. While
recuperating, and with the help of her faculty, Gunby oversaw the
relocation of Georgia Baptist College of Nursing near downtown Atlanta
to a new building a few miles north on the Mercer University campus
in 2002. (The schools merged in 2001.) She also taught first-year students about nursing concepts, processes, and
skills and graduate students about qualitative research, another
favorite subject.
taught first-year students about nursing concepts, processes, and
skills and graduate students about qualitative research, another
favorite subject.
Gunby has been part of her Georgia
Baptist alma mater for most of her 37-year nursing career. An avid
student of history, she has served on the editorial review board
of the International Association for Human Caring and the publications
committee of the American Association for the History of Nursing
(AAHN). Just recently, she worked with retired Emory nursing professor
Dr. Rose Cannon to plan the AAHN’s 22nd annual conference,
hosted by the Nell Hodgson Woodruff School of Nursing in September
2005.
As Gunby notes, Emory has an affinity
for educating nursing leaders. Her master’s class at Emory
graduated three future nursing school deans (herself, Dr. Linda
Hodges of the University of Arkansas for Medical Sciences College
of Nursing, and Dr. Pam Chally of the University of North Florida
in Jacksonville), who went on to receive their doctorates at other
schools.
“We were passionate about advancing
our education,” Gunby recalls. “It was a very competitive
environment, but we were very supportive of each other.”
She strives to instill the same value
of education in her students. “I tell my students that they
must begin planning for their career in nursing, and I encourage
them to work toward their master’s degrees and their doctorates,”
she says.
In her classes on Images of Nursing, Gunby works hard to help students
dispel stereotypes. She playfully breaks any preconceptions of what
a nurse—or a nursing school dean—should be like.

“There are stereotypes of nurses
on TV and stereotypes of what a first-grade teacher is like. But
what is a stereotype of someone who rides a Harley-Davidson motorcycle?
Well, the students come up with examples like Hell’s Angels,
tattoos, and wearing leather. And then I turn on my PowerPoint and
show a picture of me in my leather riding my Harley. It blows their
minds.”
There is another point to her lesson.
“If we stereotype our patients,” Gunby tells her students,
“that is going to get in the way of our knowing them.”
|
|
| |
 |
|
| |
Architect
for health
 |
|
| |
 f
it involves improving the health of the poor or underserved in the
state of Georgia or the nation of Georgia, chances are that Dr.
Judith Lupo Wold, 81MN, is part of the solution. f
it involves improving the health of the poor or underserved in the
state of Georgia or the nation of Georgia, chances are that Dr.
Judith Lupo Wold, 81MN, is part of the solution.
The former Georgia State University
(GSU) nursing school director and present academic fellow at Emory’s
Lillian Carter Center for International Nursing (LCCIN), Wold is
a key architect of Emory’s Farm Worker Family Health Program.
Each summer, nursing and other health professions students travel
to south Georgia to assess and treat those in the migrant farming
industry. Wold also helped implement the state’s Childcare
Advantage Network, funded by the Health Resources and Services Administration,
to train public health nurses to consult with child care directors
and staff about the health and safety of their young charges.
|
|
| |
|
|
| |
For
the past 12 years, Wold has been a primary player in improving the
health of Georgians more than half a world away through the Atlanta-Tbilisi
Healthcare Partnership. Begun in 1992 under the leadership of Emory
School of Medicine professor Dr. Kenneth Walker, the program operates
under the American International Health Association (AIHA), part
of the U.S. Agency for International Development.
After the Soviet Union fell in 1991,
health care institutions in the Eastern European nation of Georgia
crumbled. Health facilities lacked modern technology and sometimes
electricity. To compound matters, Georgia had no tradition of university
education for nurses; most entered the profession after completing
a two- or three-year nursing training program, depending on how
long they remained in high school. Through the Tbilisi project,
Wold has been at the forefront of developing a nursing education
curriculum for the former Soviet country.

“The idea has been to bring
professionalism to the nursing field,” says Wold, who continues
to serve on the GSU faculty. “We began by assessing the nursing
education system and the state of clinical nursing practice. A lively
exchange of nursing professionals began with nurses coming to Atlanta
to train, and our nurses going to Tbilisi to gather information,
assess, and teach, and, of course, learn from their culture.”
Through annual visits to the
country, Wold has watched the tenuous growth of the profession.
“The level of practice among the nurses who have been privy
to continuing education is better,” she says. The challenge
lies in navigating a culture where doctors, community members, and
even nurses do not perceive nurses as equal partners in the health
care system.
In 2004, Wold spent two weeks in Tbilisi
working with Emory graduate students Amanda Nickerson and Masayo
Nishiyama. Both are enrolled in the MSN/MPH program in international
nursing, administered by the LCCIN (Wold was interim director of
the program its first year in 2001.) Funded by grants from the AIHA
Partners for International Development, the Emory team assessed
nursing administration and staff outcomes at the new National Medical
Center and Central Children’s Hospital, which recently opened
a modern emergency room. The team also helped conduct a health fair
at a cement factory in the small rural town of Kaspi, where they
found many workers at high risk for heart disease. The physician
who runs the health clinic at the factory continues to monitor those
with problems.
“People there smoke more and
probably have a worse diet because they are poor,” says Wold,
who specializes in health promotion and prevention of cardiovascular
disease in rural areas. “They live rather hard lives, but
there hasn’t been enough research to determine what is going
on with them.”
Other nursing initiatives in Tbilisi
have ebbed and flowed over the years. A curriculum for nursing continuing
education has evolved, and a national chief nursing office was created
in the Ministry of Health. But a bloodless coup that took place
in 2003—the Rose Revolution—stalled progress, and a
new chief nursing officer has yet to be named.
Still, prospects remain bright. During
spring semester, four physicians from Tbilisi who have worked as
nurses or in nursing education attended classes and participated
in a teaching institute at the School of Nursing, led by Dr. Helen
O’Shea (see related story in One
School Gives Rise to Another). Their mission: to learn
Western curriculum development and teaching methodology, which they
are now adapting to nursing education back in Georgia. Armed with
educational resources and a new university curriculum, the physicians
are translating 27 course syllabi from English to Georgian in order
to open a university-level nursing school in 2006. Their efforts
paid off when Georgia’s minister of education gave the green
light to establish the BSN program at Tbilisi State University.
This summer, Wold and Nishiyama returned
to Tbilisi to assist the physicians with their efforts and to conduct
a workshop for nurses on the care of adults and children experiencing
respiratory problems. They also collected data on nurse administrators
and helped open Nursing Learning Laboratories at the National Medical
Center and Central Children’s Hospital.
Last year, Tbilisi partners from Emory,
GSU, Georgia Tech, Morehouse School of Medicine, and Grady Memorial
Hospital received a big boost of encouragement from Mikhail Saakashvili,
Georgia’s president, whom they met for the first time when
he came to Atlanta. “It went very well,” recalls Wold.
“He’s very young—in his late 30s—and optimistic.
He is very happy about the work we are doing in his country.”
Rebecca
Rakoczy is an Atlanta freelance writer and former editor of Pulse,
a monthly nursing supplement published by The Atlanta Journal-Constitution.
Carol Pinto, editorial associate for Emory Nursing, also contributed
to this article. |
|
| |
|
|
 |
| |
 |
|
 |
Others
Leading the Way in Nursing Education |
 |
| |
|
|
 |
Dr.
Sara Barger, 73MN, serves as dean of the Capstone
College of Nursing at the University of Alabama-Tuscaloosa,
a leadership role she has held for 10 years. She currently
is negotiating a collaborative arrangement between a community
health system in west Alabama and the nurse-operated clinic
she helped establish in rural Alabama. In 2001, she received
an Emory Medal, the university’s highest honor for alumni. |
 |
| |
|
|
 |
In
2004, Dr. Anne Bavier, 73MN,
left her administrative post in the Nell Hodgson Woodruff
School of Nursing to become dean of St. Xavier University
School of Nursing in Chicago. This year, Bavier was elected
a fellow of the Institute of Medicine and was appointed to
the board of trustees at La Rabida Children’s Hospital
in Chicago. |
 |
| |
|
|
 |
Dr.
Anne Boykin, 72MN,
has been dean of the Christine E. Lynn College of Nursing
at Florida Atlantic University in Boca Raton since 1984. Boykin
has spearheaded ongoing research on the study of caring and
how it affects nurses and improves nursing care and is in
the midst of a two-year project to implement a care plan in
a local hospital emergency department. |
 |
| |
|
|
 |
Dr.
Pam Chally, 77MN,
is a classmate of Dr. Linda Hodges (see box on page 19) and
Dr. Susan Gunby (see “Dispelling Stereotypes”
above). Chally has been professor and dean of the College
of Health at the University of North Florida in Jacksonville
since 1998. She oversees two departments, a research center,
and approximately 50 faculty members, and 1,000 students.
Chally continues to study and write on nursing ethics and
adolescent and maternal health. |
 |
| |
|
|
 |
Dr.
Kay Chitty, 65N, 68MN,
directed the School of Nursing at the University of Tennessee-Chattanooga
from 1989 to 1995. As director, she helped establish the school’s
first endowed professorship, begin a master’s program,
and improve graduates’ state board scores. “A
dean is like a sparkplug,” she says. ”There are
all these cylinders that you have to keep lit and firing in
order to keep the people with skills and abilities in a particular
area able to maximize them.” |
 |
| |
 |
|
 |
Dr.
Sarah Hall Gueldner, 65MN,
was appointed dean of the Decker School of Nursing at Binghamton
University in New York in 2003, having served as professor
and director of the School of Nursing at Pennsylvania State
University. As dean, Gueldner is working to build Decker’s
scholarship base—which includes a fairly new doctoral
program in rural health nursing—and attain increased
national visibility for the school. |
 |
| |
 |
|
 |
Dr.
Sue Hegyvary, 66MN,
dean emeritus and professor at the University of Washington
School of Nursing, is the editor of the Journal of Nursing
Scholarship, published by Sigma Theta Tau International. Currently,
Hegyvary and two other colleagues are studying the determinants
of health in more than 160 countries, focusing on life expectancy
and child mortality. This spring, she presented their early
findings at Emory as the 2005 Hugh P. Davis Lecturer and received
an honorary degree from Emory. |
 |
| |
 |
|
 |
Dr.
Linda Hodges, 77MN,
has served as dean of the University of Arkansas for Medical
Sciences College of Nursing in Little Rock since 1989. Hodges
is past president of the Southern Regional Educational Board
Council on Collegiate Education for Nursing.
Most recently, she helped secure major federal funding to
develop a regional family psych/mental health nurse practice
specialty and a research center for individualized nursing
intervention at her school. |
 |
| |
 |
|
 |
Quinn
McClean, 92MN/MPH,
can look back proudly at what she accomplished as director
of the School of Health Sciences and the nursing program at
Koc University in Istanbul from 1999 to 2002. Among her accomplishments:
supervising construction of a building to house the school
of nursing and a conference center and establishing an education
and research center to provide continuing education for nurses
and allied health professionals. McClean now resides with
her family in Washington, D.C. |
 |
| |
 |
|
| |
As
dean of Governers State University near Chicago,
Dr. Linda Samson, 72N, 73MN,
oversees programs in nursing, occupational therapy, physical
therapy, speech pathology, social work, health administration,
and addiction studies. She also leads a Project EXPORT Center
of Excellence in Health Disparities, funded by the NIH, to
reduce health disparities among women and children. Prior
to joining Governors State in 2002, she served 10 years as
dean of the School of Health Sciences at Clayton College and
State University, located south of Atlanta. |
|
| |
 |
|
|
 |
| |
 |
|
|
|
|











