 |
| |
|
|
| |
 |
Emory
medical faculty last year were responsible for more than 3.3 million patient
visits in clinical facilities either owned by or affiliated with Emory
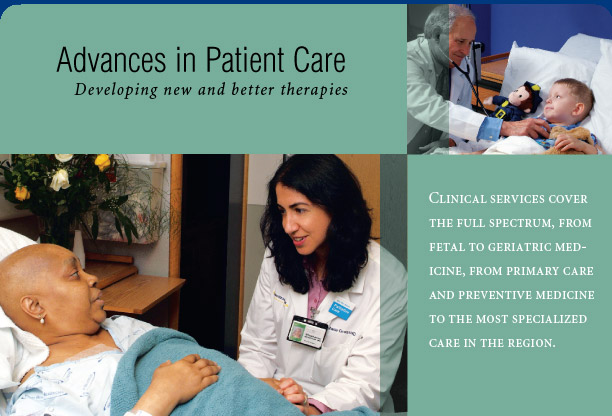
(see Hospitals and Clinics). These clinical
services comprise a substantial proportion of all health care provided in
Atlanta and cover the full spectrum from fetal to geriatric medicine, from
primary care and preventive medicine to the most highly specialized care
in the region. Many of these services are unavailable elsewhere in the city,
state, or region.
For example, Emory physicians practicing at
Grady Memorial Hospital, a public hospital funded by DeKalb and Fulton counties,
lead the state's only poison control center, one of the nation's largest
burn centers, and the area's only level 1 trauma center, as well as the
state's largest programs in sickle cell anemia, diabetes, lupus, and infectious
disease.
Emory also serves as the referral center for
Georgia's newborn screening program and is responsible for follow-up of
nearly 5,000 abnormal screening tests performed in six area hospitals each
year. Emory has specialty clinics for patients with Down syndrome, fragile
X syndrome, and other genetic disorders. Emory's Cystic Fibrosis Adult Program
is the only program in the city providing care specific to the needs of
the increasing number of adult patients with this disorder. In addition,
the Emory Transplant Center is one of only a few such centers in the country
providing islet cell transplantation for type 1 diabetes.
The unique services offered, together with
the breadth and diversity of the populations seen in facilities served by
Emory, not only support the needs of Atlanta and the region but also make
Emory's training programs some of the most sought after in the country.
Despite increasing pressures placed on clinicians
in today's challenging health care environment (especially for academic
physicians with responsibilities for teaching and research and for treating
the sickest of the sick in addition to a high relative proportion of indigent
and uninsured patients), Emory clinicians continue to push the envelope,
always seeking ways to improve care. Following are some examples. |
 |
| |
|
|
 |
| |
|
|
 |
Heart
care |
|
 |
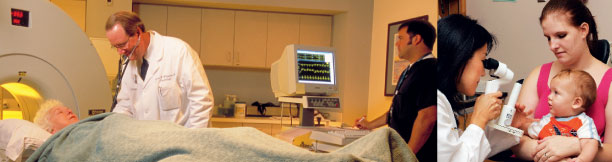
Emory
University Hospital was the first hospital in Georgia to implant a ventricular-assist
device without surgery. Unlike traditional ventricular-assist devices, which
require surgery to access the heart, the new TandemHeart device is designed
for insertion through the femoral artery. The device restores blood circulation
in as little as 30 minutes. The resulting increase in blood flow helps save
vital organs and gives damaged hearts a chance to heal, helping patients
survive severe heart attacks or making those who need a heart transplant
healthy enough to be placed on a transplant waiting list.
This past year, faculty surgeons at Emory
University Hospital also performed the state's first implant of a ventricular-assist
device as a form of destination therapy (permanent therapy in place of a
heart transplant). More commonly, such devices are used as a bridge to transplant.
Physicians at Emory Crawford Long Hospital
also were the first in the country to use a new advanced imaging system
to detect heart and other diseases in their earliest forms. The system combines
PET technology with the fastest 64-slice CT scanning available, allowing
physicians to obtain highly detailed information in a single, noninvasive
procedure. |
 |
| |
|
|
 |
Regenerative
medicine |
 |
 |
About
70% of people who have a heart attack suffer permanent damage to the heart
muscle, and no treatments are available to restore function to this damaged
tissue. Medical faculty conducting a new clinical study at Emory Crawford
Long Hospital are trying to change that, using stem cells generated within
patients' own bone marrow to grow new blood vessels to improve circulation
around the heart. They are enrolling patients who have had acute heart attack
within the past four to five days and who have already received the standard
of care for their condition. This is one of some 600 clinical trials being
conducted by Emory medical faculty. |
|
| |
|
|
 |
Brain
tumors |
|
 |
Radiation
oncologists in the medical school recently performed Georgia's first
frameless radiosurgery brain tumor treatment, eliminating the rigid head
frame used typically in radiosurgery, which can cause discomfort, swelling,
and bruising. Frameless radiosurgery requires only a custom-made mask, secured
to the table on which the patient lies, and a fitted dental bite plate with
embedded reflective markers. Matching a CT scan performed immediately before
the treatment with a previous scan used to plan therapy corrects discrepancies
in position, while an advanced optical radio-camera system uses the bite
plate reflective markers to continuously track the patient's position.
|
 |
| |
|
|
 |
| |
|
|
 |
Neurointensive
care |
|
 |
Medical
faculty will soon realize their dream of having a new state-of-the-art
neurointensive care unit in Emory University Hospital. The new facility
brings all neurologic services together on one floor, eliminating the
need for patients to be moved long distances for necessary services, such
as CT scans. The patient- and family-friendly unit also provides greater
physical space for family members, who often spend extensive time with
patients in the unit. |
 |
| |
|
|
 |
Traumatic
brain injury |
|
 |
No
new medical therapies for traumatic brain injury (TBI) have been developed
in more than 30 years, until now. Early results from a clinical trial designed
and conducted by Emory emergency medicine physicians show that giving progesterone
to trauma victims shortly after brain injury may reduce the risk of death
and degree of disability. The study was conducted at Grady Memorial Hospital,
where the level 1 trauma center is headed by Emory physicians. This study
was the first clinical trial of its kind in the world, and the research
team is now planning a multi-institutional phase III clinical trial of 1,000
patients with TBI. Other studies will determine progesterone's effectiveness
in pediatric TBI, blast-related brain injury (a major cause of death among
combat personnel), and acute stroke. |
 |
| |
|
|
 |
Palliative
care |
|
 |
Unlike
hospice care, used for patients at the end of their lives, palliative care
focuses on the many ways serious illness or chronic conditions affect patients
and their families in any stage of illness. A new palliative care program
was launched this year by medical school faculty at Emory University Hospital
and Emory Crawford Long Hospital, with the goal of helping patients by relieving
both physical and nonphysical suffering that accompanies serious, chronic,
or terminal conditions. |
 |
| |
|
|
 |
For a list of the facilities
in which Emory medical faculty practice, please see (see
Hospitals and Clinics). |
|
| |
|
|
 |
Top |
|
 |
Copyright
© Emory University, 2006. All rights reserved |
|
| |
|
|


