Year one

A recent graduate tells about his first year on the job
“How long have you been a nurse?” a patient will sometimes ask. I always know why the question is posed. My silver hair, face, and hands reveal my time on earth, so surely I must be a grizzled veteran of floor nursing. My answer always surprises them: I’m a new nurse. I was 58 when I graduated last May from Emory University’s nursing school.
As you read this, I’ve had RN behind my name for almost a year. I call myself a cardiac nurse because I’m learning how to be a nurse on Unit 21 at Emory University Hospital Midtown, formerly Emory Crawford Long Hospital. It’s the same unit where I was a patient more than eight years ago following my own quadruple-bypass surgery. Unit 21 is a telemetry unit, but we’re more than cardiac nurses. We also care for post-op lung and esophageal cancer patients, vascular patients, and others. It is a demanding, intense, and stressful launching pad for a new nurse.
 |
Has the experience so far been what I expected? I knew something about this floor before joining its staff. Besides having been a patient in room 2118, I spent two years as a Mended Hearts volunteer here, working with open-heart patients during the long recovery that follows this major surgery. My last semester as a nursing student was on Unit 21, working with the same veteran RN who would become my preceptor.
Gerry Wall has worked on this floor for 22 years. She was the preceptor each new nurse hopes for and deserves, consistently encouraging and supportive, always patient. When I was discouraged at what I perceived to be my own slow progress, she assured me that the technical skills would come with time and repetition. She claimed to see in me an uncommon gift for connecting with patients. “Your patients love you, your coworkers like you. You’re doing a great job,” she told me on days when I seemed to need encouragement. And Gerry set patient-care standards I try to follow each day. I never saw her compromise patient safety or take a shortcut—even on days when the workload was almost overwhelming.
No nursing school, even one bestowed with limitless resources, could fully prepare a new nurse to assume total responsibility for four or more critically ill patients. No classroom course could possibly teach the time-management skills demanded by a job like the one I’ve chosen.
On a typical day, I begin my shift with four or five patients. After charting head-to-toe assessments and vital signs (we RNs do our own vital signs every four hours), I check for new morning orders on my patients and scan those containing new or changed medications to the pharmacy. Administering medications to just four to five patients can take two hours or more—opening PO packages; drawing up IV meds, flushing, pushing and flushing again; punching and hanging bags, programming pump settings, labeling tubing. I’ve thought often of my first clinical rotation and how my clinical instructor, Erin Ferranti, watched patiently as I fumbled and fidgeted in my first attempts to draw medicines from a vial. I wish she could see me now. I have had days on the floor during which I dispensed meds to my patients almost non-stop for the entire shift, struggling between patients to complete other ordered tasks: emptying or removing chest tubes, changing or removing central lines, changing dressings, collecting lab draws or samples, transferring and walking patients. I’m constantly reprioritizing, in my head and on lists, juggling times, orders, medicines, policies and procedures, assessments, tests, labs, requests and issues—from patients, family members, doctors, and management. And of course, there’s charting—lots of charting.
One evening, as my face reflected my distress after new orders were written on each of my patients an hour before the end of my shift,
I received some simple but sage advice from a veteran Unit 21 nurse, Sue Rodgers. “Don’t look at the whole picture,” she advised me. “If you look at everything you have to do, you’ll just get paralyzed. Prioritize, decide what needs to be done first, get that done, and then do the next thing. It will all get done, and your patients will be safe. At the end of the day, that’s what is important.”
During a typical day, I also may discharge one or more of my patients, a process that requires paperwork, education, and for cardiac patients, scheduling follow-up physician appointments. I enjoy discharging patients, especially open-heart patients, because I enjoy patient education. Open-heart surgery recovery is measured not in terms of days, but in weeks and months. Alone among my nurse coworkers, I know personally the roiling of emotions, the challenge to a weakened physical body, the discouragement, and the triumph of recovery. I’ve offered my telephone number to patients who seem particularly distressed about their ability to recover, and some of these patients have called me at home weeks after discharge to seek encouragement and motivation. They also tell me what my words, care, and example meant to them during their hospitalization and recuperation. This is my strength during hard days.
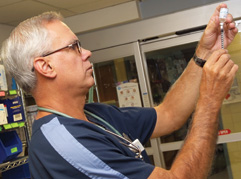 |
Nursing school provides the information we will need to be a nurse, but we learn, on the job, how to be a nurse. —Randy Evans, RN, 08N |
||
I noticed from our earliest clinical rotations that many of my young classmates were most intimidated not by procedures or medicine administration, but by the simple act of entering a patient’s room and connecting personally with the person in the bed. I do this easily. When I care for a cardiac patient, I know that person’s pain, and I have experienced the same emotions. I have been extubated. I have had chest tubes removed from my body. I have hugged a pillow to my split sternum, dreading the next cough. I have shuffled painfully 200 feet around the same nursing station and heaved in exhaustion at the end, frightened by my incapacitation. Make no mistake: knowing this makes a difference to the patient, and makes me a different kind of nurse.
Nursing school provides the information we will need to be a nurse, but we learn, on the job, how to be a nurse. I am sufficiently mature, sufficiently humbled by the responsibility of caring for sick persons to ask questions, to seek assistance or guidance in areas where I am unsure or inexperienced, and I am inexperienced in most areas, often unsure. But I am fortunate to be learning on Unit 21, where so many nurses and nurse managers, day and night shift, have so willingly helped me and taught me. And not just nurses: I have asked for and received help from secretaries, nurse technicians, housekeeping staff, physician assistants, and physicians. Nursing is more difficult and challenging than I ever imagined: always arduous and exhausting, often laborious, exasperating, frustrating, and poorly compensated. But at the end of every shift, I walk out of the hospital’s bright lights into the same dark from which I entered sometimes 14 hours before, gratified and satisfied that I have made a difference in someone’s life that day. I know of few jobs that provide that kind of fulfillment. May I never lose it.


