Education: Long-term care of students
A major goal of the new curriculum introduced in 2007 is to create connections between faculty and students that last throughout the entire four years of medical school, “longitudinal” relationships much like those that should exist ideally between doctors and their patients. Based on the kind of students who are attracted to Emory and on what they learn and model from their faculty mentors, these students are expected to grow not just in knowledge during their time at Emory but also in compassion, curiosity,and commitment—and to use these traits wisely; in serving their profession and community.
| In this section |
Society advisers At the heart of the curriculum is a highly popular system of faculty advisers, each faculty mentor paired with eight or nine students. These groupings are designated as “societies” named for historical medical luminaries—for example, Osler, Semmelweis, Lister, Harvey. Faculty advisers who lead these societies in each class are chosen carefully, their salaries underwritten by the medical school so they can relinquish three half-days per week from their regular clinical and/or research duties to spend time with some or all of “their” students.
With steady and intentional access to their mentors, students in each society invariably become caught up in their adviser’s work and interests: touring Atlanta’s historical sites under the wing of an adviser who is a world-class history buff, visiting a monthly neurologic disease clinic in a nearby mountain community, participating in AIDS walks and other fund-raisers, or enjoying a home-cooked meal and chance to practice physical exams on an adviser’s 2-year-old.
Road-tested first phase As the class of 2011 moves through the new curriculum, all now have completed the 18-month Foundations of Medicine phase, a whole-person approach section that combines clinical medicine and basic fundamentals of science, social sciences, humanities, and public health. This is not my father’s or mother’s medical school experience, students say.In the introduction-to-neuroscience module, for example, faculty share the classroom with a baseball player, who demonstrates and explains what a center fielder has to do to catch a fly ball or what a batter must consider before swinging at a ball leaving the pitcher’s hand at 95 mph. Students then are sent off to research the anatomic, physiologic, and neurologic functions involved in those cognitive, visual, and physical processes. Who would have dreamed that this game was so biologically complex?
In a teaching module on aging, a 50-year-old patient—in reality, one of many actors involved in medical education—describes her health and particularly the challenges of beginning menopause. The following day, she is 10 years older, in both appearance and the symptoms she describes. By the third class, she talks about being 70. At week’s end, she is 90 and knows she is dying. Students not only study the body, from cellular senescence to why the body needs to age, but they also become highly sensitized to what life is like for an aging person. “I look at the patients I see differently now,” said one student, “and I realize that my grandparents’ house is filled with risks for falling.”
Teaching the teachers Ensuring that Emory’s medical training yields compassionate clinicians cannot be left to chance and must be intentional and deliberate. This maxim was reinforced by a recent study on which the medical school took the lead to determine whether “humane” care can be “taught” and “learned.” In the study, which involved four other medical schools, facilitators implemented a curriculum emphasizing the human dimensions of care, such as the need to communicate effectively, show compassion, and build strong relations.
After faculty members in the study had undergone the special training, their trainees (both students and residents) completed a questionnaire designed to evaluate its effectiveness. Students of faculty who were trained in the humanistic model of medicine rated their professors higher in how they demonstrated this type of care, communicated with patients and each other, and inspired students, among other measures. The results were statistically significant and sufficiently robust to suggest practical importance, according to Emory internist William Branch, lead author of the study, which was published in Academic Medicine.
Creating cross-disciplinary scientists In partnership with Emory’s Rollins School of Public Health and other entities both in and outside the university, the medical school is co-directing a new PhD program, “Human Health: Molecules to Mankind” (M2M), designed to educate students in both lab and population sciences and to bridge the gap among scientific disciplines. M2M includes four tracks: predictive health, population processes and dynamics of infectious diseases, biomarkers and development of acute and chronic diseases, and genetic environmental determinants of health.
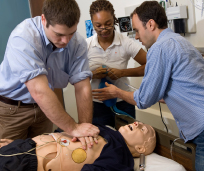 |
In addition to learning clinical care in simulation labs and in interactions with actors and real patients, Emory students have diverse research opportunities with partners like Rollins School of Public Health and Georgia Tech. Last year, two Emory students were among 40 selected nationally by CDC to participate in its applied epidemiology fellowship involving an epi project and field experience and culminating in scientific presentations. |
|||

