|
 New sim lab space for nursing school |
 |
 In brief |
| March 28, 2016 | ||||||||||||||||
Nursing moves to 8th and physical therapy to 5th in US News rankings
In the most recent US News & World Report graduate school rankings, published this month, the Nell Hodgson Woodruff School of Nursing ranked 8th in the nation, moving up from 10th. It is the top-ranked nursing school in Georgia and the No. 2 ranked nursing school in the Southeast. The school's family nurse practitioner program moved from 11th to 10th. The joint Emory-Georgia Tech biomedical engineering PhD program ranked 2nd in the nation for the 10th consecutive year. The medical school moved up in the primary care ranking from 42 to 29 and maintained its ranking of 23 among research-oriented schools. The school's physical therapy program moved up from 7th to 5th. Its physician assistant program was not ranked this year and remains 3rd in the nation. The Rollins School of Public Health also was not ranked this year and remains 7th. Read more about other Emory rankings. View a current list of all rankings in the Woodruff Health Sciences Center. Redefining sepsis and septic shock
Craig Coopersmith and Greg Martin were part of a task force of international experts in critical care medicine that recently redefined the terms "sepsis" and "septic shock" to facilitate earlier recognition and more timely management of these conditions.
The results were presented at last month's 45th Critical Care Congress of the Society of Critical Care Medicine (SCCM), to coincide with publication in JAMA. This is the third major effort to better define sepsis and septic shock in 30-plus years. Definitions were last revised in 2001 (Sepsis-2) and before that, in 1991 (Sepsis-1). Sepsis is a major public health concern, being the primary cause of death from infection and the third leading cause of death overall in the U.S. In 2011, it accounted for more than $20 billion of total U.S. hospital costs. The reported incidence of sepsis is increasing, likely reflecting individual susceptibility and greater recognition of the condition. "Since considerable advances have since been made in the pathophysiology, management, and epidemiology of sepsis, there was a need for re-examination of these two conditions," says Coopersmith, associate director of the Emory Critical Care Center. "Better defining sepsis and septic shock will help us treat patients in a more timely fashion, plus offer greater consistency for epidemiologic studies and clinical trials." The task force to address these redefinitions was convened by the SCCM and the European Society of Intensive Care, both of which supported this work with grant funding. Coopersmith was SCCM president when the definitions were being revised. For one year, the group reviewed large data sets pertaining to hospitalized patients with presumed infection, assessing the simplest and most accurate ways to determine which patients have sepsis. Once definitions were updated, they were circulated to international professional societies, with requests for peer review and endorsement. "In lay terms, the task force defined sepsis [now known as Sepsis-3] as a life-threatening condition that arises when the body’s response to an infection injures its own tissues and organs," says Martin. Patients with suspected infections who are likely to have a prolonged ICU stay or die in the hospital can be identified at the bedside with a new test that examines respiratory rate, mental status, and blood pressure to determine risk of mortality and need for prompt intervention. The new definition of septic shock is a subset of sepsis in which underlying circulatory and cellular/metabolic abnormalities are profound enough to substantially increase mortality. "These updated definitions and clinical criteria should clarify long-used descriptors and bring about earlier recognition of patients at risk of developing sepsis," says Coopersmith. "But the process remains a work in progress, and new diagnostic approaches and enhanced collection of data will fuel their continued re-evaluation and revision." Coopersmith adds that interest in the JAMA article, which both he and Martin co-authored, was high. As of March 25, the article had 754,792 page views, and the paper is in the 99th percentile of all research outputs scored by Altmetric. New frontiers in simulation training
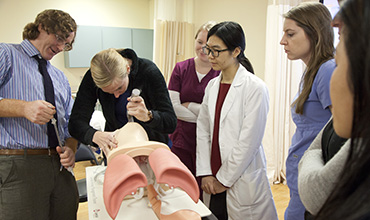
For Kate Moore, who recently orchestrated expansion of the nursing school's simulation training facilities, the idea of "space" is every bit as thrilling as it was for Captain Kirk, although decidedly more down to earth.
Until last fall, BSN and MSN students shared simulation training space in the Evans Center for Caring Skills, located on the first floor of the nursing school building. While undergraduates continue to train there, graduate students now practice skills in a new 4,000-square-foot space that formerly housed outpatient clinics on the Emory Wesley Woods campus. The space includes a procedures lab with a large classroom and video monitors; four hospital beds; low-fidelity adult, child, and infant mannequins; and a skeleton for tube placement. It also includes a health assessment lab with 12 exam rooms and a main desk equipped with four computers and audio headsets for faculty to monitor groups of students. The expansion doubled nursing's space for simulation training, and for good reason. Student numbers have grown steadily in recent years, with 322 BSN students and 194 MSN students currently enrolled. The new space "allows us to teach more small groups at each location," says Moore. Simulation training has become increasingly essential in preparing nurses to practice high-quality, team-based care. Early this semester, emergency nurse practitioner (NP) and adult-gerontology acute care NP students took to the procedures lab to practice difficult airway skills, chest tube insertion, lumbar punctures, and cricothyroidotomy techniques. "A major driver for using simulation is the challenge of obtaining enough clinical placement sites for students and providing them the opportunity to participate in 'must-have' experiences such as cardiac arrest, rapidly changing situations, and airway challenges," says Elaine Fisher, director of accreditation and curriculum for the school. "Areas to enhance learning with simulation are based on course and program objectives, professional organization and accrediting body requirements, and scope of practice for entry-level and advanced practice nurses." In the Evans Center, Fisher notes, BSN students participate in numerous scenarios requiring them to demonstrate various skills. They monitor their patient, who can develop complications at any moment. They look at lab work, vital signs, and changing medication requirements and chart information in the electronic health record. Such scenarios help prepare them for interprofessional team training with medical and other health profession students. Thanks to the new space at Wesley Woods, faculty member Imelda Reyes was able recently to bring parents and children to the health assessment lab to interact with pediatric NP students. Students worked with them to complete a history and physical and then give a report of their assessment. This type of experience is invaluable, Fisher says. "When students went to their clinical sites, their preceptors commented on how much better the students performed than in prior years." That's welcome feedback for Moore, as the nursing school’s director of simulation training. Her expertise harkens back to her U.S. Army Reserve experience in Iraq, where she served as assistant chief nurse of the 10th Combat Support Hospital in Baghdad's Green Zone. She cared for servicemen and civilians alike and commandeered leftover patient mannequins to train nurses, EMTs, and others in treating mass casualties. Two years ago, Moore supervised expansion of the Evans Center simulation lab and advocated greater integration of simulation training across the BSN curriculum. She advocates the same for MSN students at the Wesley Woods facility, and she intends to keep pushing the simulation frontier at Emory. "We could become one of the largest simulation training programs in the country," she says. "The potential is there."—Pam Auchmutey Sheep versus wolves: potential new class of targeted antibiotics
Like sheep dogs protecting the flock, the body's galectin proteins can fill in gaps in the immune response against microbes (wolves) that disguise themselves to look like the body's own cells (sheep). Sean Stowell (pathology) explains how galectins work in a four-minute video, the second in a new series highlighting basic research in the medical school. Stowell and other Emory scientists identified galectins' anti-bacterial properties and now are engineering galectins that could target bad microbes while leaving beneficial ones alone. If successful, this work could lead to an entirely new class of antibiotics. This video, which has proven highly popular on YouTube, showcases the breadth of research being done in Emory's Antibiotic Resistance Center. It was produced by Damon Meharg with writer Quinn Eastman and narrated by Peta Westmaas.—Mary Loftus |
| From the Executive VP
Diversity and inclusion—key values and priorities
Poet Maya Angelou once advised, "It is time for parents to teach young people early on that in diversity there is beauty and there is strength." She's right, of course, and that's why diversity and inclusion are key values and priorities of the Woodruff Health Sciences Center and Emory Healthcare. I share our institutional commitment to ensuring equity, inclusion, and respect for all people—both our own and those whom we serve. To better understand where we are (and where we need to be), the senior leadership group and I have undertaken a diversity and inclusion audit of all WHSC units, and I've been greatly impressed by the work that's being done and by our teams' real commitment to living these values. As I collect a full picture of the units' best practices, I will share them broadly to inform, shape, and be consistent in our diversity and inclusion efforts, and as we move forward, I'll be reaching out to each of you for your ideas and feedback as well.
Match Day 2016
On March 18, Emory medical students, along with thousands of others across the country, learned where they would begin their careers as MDs. Read more details. Watch a short video. Reducing "pajama time" for physicians
In a recent article in MD Magazine, hospitalist and Emory Healthcare CMIO Julie Holberg discussed work flow improvements to EeMR that reduced clicks for physicians and resulted in a 36% reduction in "pajama time," the time they spend in the system at night and on weekends. Read more. New president's annual report
Parkinson's specialist Mahlon DeLong is one of the health sciences faculty featured in the 2015 President's annual report, Emory Leads. New CRISPR services
The Transgenic Mouse and Gene Targeting Core is now making CRISPR/Cas9 gene editing techniques available to the research community. Read more. JScreen cited for innovation
JScreen, a national at-home genetic screening program based out of Emory's medical school, was named one of North America's top innovative Jewish organizations in the 2016 Slingshot Guide. JScreen has screened approximately 4,000 individuals and couples of reproductive age and has identified 150 at-risk couples. Read more. New clinic location
A new Emory Clinic location opened March 1 in Tucker, adjacent to Emory University Orthopaedics & Spine Hospital on Montreal Road. Notable
Allen Beck is interim chair of ophthalmology in the medical school and interim director of the Emory Eye Center.
Rasheeta Chandler (nursing) was named one of 40 Under 40 Leaders in Health Care by the National Minority Quailty Forum.
Gari Clifford is interim chair of biomedical informatics in the medical school.
Hannah Cooper (behavioral sciences and health education, public health) co-edited a special issue of the Journal of Urban Health that examined police violence as a public health issue. Read more.
Solveig Cunningham (global health) received Emory's 2016 Levy Award for Junior Faculty for contributions to the study of obesity.
Haian Fu (Winship, pharmacology) was named the Winship Partner in Research Endowed Chair. Recently announced recipients of the university's 2016 Award of Distinction include four from health sciences: Sonia Bell (infectious diseases), Katherine Egan (medical school), Sharmyn Gipson (animal resources), Adam Malm (nursing school). Events
Currently on display: Art and photography by Alzheimer's patients in the atrium of the medical school building. Read more.
Also on display: Joel A. Katz Music Is Medicine Collection. Permanent exhibit in tunnel level of Winship. Read more. April 14: Seventh Annual Academic & Industry Intersection Conference, 9 a.m. - 1:30 p.m., Emory Conference Center. Register. May 1-3: Bridging the Sciences: Zika Virus. Emory Conference Center. More info. May 18: 3rd Annual Advancing Health Care Quality at Emory. 8:30-5. SOM Auditorium 110 and lobby. Deadline for abstracts is March 30. |