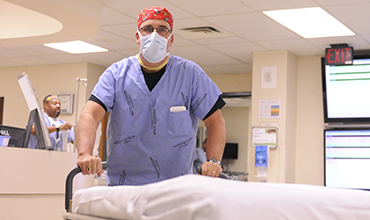
Radiation response: CEPAR drill |

Synergy awards |

MotherToBaby Georgia |
 In brief |
|||||
| September 30, 2016 | |||||||||||||||||
Third Emory hospital receives Magnet status
When Emory University Orthopaedic & Spine Hospital (EUOSH) received notification this month from the American Nurses Credentialing Center that it had achieved Magnet recognition, it became one of only 444 health care organizations in the world to be so designated.
Magnet recognition is the most prestigious distinction a hospital can receive for nursing excellence, and it takes years of preparation and hard work to achieve. No one is more aware of the challenges involved in this process than June Connor, who led the Magnet charge for EUOSH as hospital CNO and COO. "This is a highly choreographed effort throughout the entire hospital, and I am so, so proud of our entire team," says Connor, who is also interim chief nursing executive of Emory Healthcare. Organizations seeking Magnet status must undergo a rigorous and lengthy process that demands widespread participation from leadership and staff. This includes an electronic application, written patient care documentation, an on-site visit, and a review by the Commission on Magnet Recognition. "The on-site visit gave us the opportunity to showcase our teamwork in action," says Connor. "The appraisers were impressed with the participation and cooperation of the staff, physicians, and nurses they encountered. Our Magnet designation validates that our teams are on the right path to continued success." As a fellow alumna of Emory's nursing school, Linda McCauley, the school's dean, extends special congratulations to Connor and the EUOSH team: "The high-quality care provided in Magnet organizations depends on having a well-educated nursing workforce," she says. "Recent studies indicate that Magnet hospitals' performance in terms of lower mortality rates, fewer medication errors, and better overall outcomes can be directly attributed to the investments made in highly qualified nurses prepared at the undergraduate and master's level. June Connor and her team instill these values across the organization." EUOSH's new designation makes Emory Healthcare the only system in Georgia with three Magnet hospitals (including Emory University Hospital and Emory Saint Joseph's Hospital). Only four other hospitals in Georgia, in addition to Emory's three, are recognized as Magnet. Read more about the EUOSH designation. View a list of Magnet hospitals in Georgia. Drill simulates response to mass casualties from radiation exposure
On Saturday morning, September 17, Emory nursing and public health students walked onto the airfield at Dobbins Air Reserve Base and into the cavernous body of a C-130 Hercules aircraft, where they cheerfully allowed themselves to be strapped onto stretchers piled five-high. Moments later, they heard the call: "The exercise has begun." Personnel from the Georgia State Defense Force and Cobb Medical Reserve Corps entered the plane, secured the stretchers, and carried the volunteers, who were simulating patients with radiation injuries, into a bustling triage area in a hangar nearby. Emory and Atlanta VA Medical Center physicians and nurses performed simulated medical evaluations, and local EMTs placed the most severely injured "patients" into two mobile ambulance buses. Cobb/Douglas Public Health personnel assisted the VA with command and control functions. This mock scenario was part of a drill named "Operation Gateway," which included more than 250 people representing more than 15 health care and government agencies simulating the local response to a mock radiation incident with mass casualties.
Sam Shartar, senior administrator of Emory's Office of Critical Event Preparedness and Response (CEPAR), directed the drill. "This exercise is important because we are able to test the processes required to receive large numbers of casualties. Improvised nuclear detonations are low-probability, high-consequence events. But these same processes will also be used for response to higher-probability events like hurricanes, floods, or earthquakes," he says. The drill was conducted by the Emory Radiation Injury Treatment Network (RITN), which is part of the national response plan for a mass casualty radiation incident resulting in bone marrow-toxic injuries. Emory University Hospital is a RITN center. If a nuclear device were detonated somewhere in the United States, the National Disaster Medical System would be activated. Military aircraft would transport persons injured by radiation to Dobbins. The patients would then be transported to Emory and Northside hospitals for treatment. Read more about the drill and the players involved. WHSC names 2016 Synergy Award recipients
Last spring, WHSC researchers were invited to apply for internal grant funding through the first-ever cycle of WHSC Synergy Awards, created to support new collaborative research projects, from basic to clinical, among all disciplines in WHSC schools, centers, and faculty, from all levels of academic rank. Proposals had to include faculty with primary appointments in at least two schools as co-PIs and had to pertain to new research projects not yet funded or published. The awards would offer as much as $100,000 for one year, with potential carryover to a second year. According to David Stephens, WHSC VP for research, the response was impressive. "Both the quantity and quality of the proposals we received were remarkable and emphasize the interest in opportunities for more collaboration in research." The six winning proposals for 2016 have been announced, as follows: - Relationship of the gut microbiome to neurodegeneration in Alzheimer's disease: James Lah (neurology), Elizabeth Corwin (nursing), Viola Vaccarino (epidemiology) - Evaluation of an intervention to increase post-abortion LARC Uptake: A randomized controlled trial of educational and financial counseling prior to clinical presentation: Kristin Wall (epidemiology), Lisa Haddad (gyn-ob), Victoria Phillips (health policy & management) - Measuring fertility in reproductive-aged women diagnosed with systemic lupus erythematosus: Sam Lim (medicine), Penelope Howards (epidemiology) - Does norovirus infection cause nutritional damage? A longitudinal analysis: Anne Williams (pediatrics), Ben Lopman (epidemiology), Parmi Suchdev (pediatrics)
- Advancing cancer screening and early detection among people living with HIV/AIDS: Theresa Gillespie (surgery), Jessica Wells (nursing) - Optimizing screening mammography accuracy and adoption through improved recall rates: A multi-disciplinary investigation of the effects of human capital depreciation and fatigue on radiologist performance: Richard Duszak (radiology), Jason Hockenberry (health policy & management), Elizabeth Krupinski (radiology), Mary Newell (radiology), Margaret Fleming (radiology) Addressing concerns re exposures during pregnancy and breastfeeding
Pregnant and nursing women have a lot of questions, and Bethany Kotlar has a lot of answers. |
| From the Executive VP
Well done, EUOSH!
Earlier this month, Emory University Orthopaedics and Spine Hospital (EUOSH) achieved Magnet recognition from the American Nurses Credentialing Center (ANCC), joining Emory University Hospital and Emory Saint Joseph’s Hospital, and making Emory the only health system in Georgia with three Magnet-designated hospitals. Magnet accreditation is the undisputed gold standard for nursing excellence, and I’m proud of Interim Chief Nurse Executive June Connor and the entire team at EUOSH, whose hard work, dedication, and excellence have enabled them to join this elite community—a goal they accomplished in impressive fashion. The ANCC Commission on Magnet identified 11 exemplars (outstanding best practices) from the EUOSH application and site visit, and the commission chair was enthusiastic that this number of exemplars would set a high benchmark for others to model.
New CNE for Emory Healthcare
Sharon Pappas will begin her role as chief nurse executive for Emory Healthcare on Nov. 14. She comes form Centura Health in Denver, where she is CNE and CNO for Porter Adventist Hospital. Her daughter, Ruthie, is a nursing student at Emory. Read more. $5 million from Rollins to Seavey Clinic
The O. Wayne Rollins Foundation has made a second $5 million gift to the Seavey Clinic, which is directed by David Roberts (internal medicine). The gift is intended to sustain the individualized care, teaching, and research modeled by the late Paul Seavey. Read more. Winship expands network The Winship Cancer Network has expanded to include Peyton Anderson Cancer Center at Navicent Health in Macon. Read more. Search engine for HIV PrEP access
RSPH researchers led by Aaron Siegler introduced a new website this month at the 20th Annual Conference on AIDS, which allows users to locate providers that can prescribe pre-exposure prophylaxis (PrEP) to prevent HIV infection. Read more. Task Force receives $2 million Practices earn medical home recognition Nine primary care practices in the Emory Healthcare Network recently earned Patient-Centered Medical Home Level 3 (the highest) recognition from the National Committee for Quality Assurance. Read more. Notable
Bassel El-Rayes was selected to hold the John Kauffman Family Professorship for Pancreatic Cancer Research. Read more.
Veda Johnson (pediatrics) was appointed to a Marcus Society in Pediatrics Professorship.
Felipe Lobelo (global health, RSPH) was appointed to the Action for Healthy Kids Board of Directors. Read more.
Tammie Quest (director, Emory Palliative Care Center) was appointed by Governor Nathan Deal to the Georgia Palliative Care and Quality of Life Advisory Council.
Raymond Schinazi (pediatrics) received the 2016 Lifetime Achievement Award for Public Service from the Institute of Human Virology. Read more.
Nate Spell, previous chief quality officer (CQO) for Emory University Hospital, is now associate dean for education and professional development in the medical school. Frank Brown (psychiatry) is the new CQO for EUH.
Kenneth Walker (associate chief of internal medicine at Grady) was named the 2016 Lifetime Heroic Achievement winner by the Georgia Hospital Association.
Steven Wolf (rehabilitation medicine) received the 2016 Excellence in Rehabilitation of Aging Persons Award. Read more.
Manuel Yepes (Yerkes) was named the inaugural Rollins Chair in Stroke and Imaging Research. Read more. Events Oct. 1: Sixth Annual Winship Win the Fight 5K Walk/Run. 8:30 a.m., McDonough Field. Atlanta Braves Vice Chairman John Schuerholz will serve as grand marshal. Volunteers needed to help this Friday, Sept 30. Register. Oct. 10-11: NETEC Emerging Infectious Disease Preparedness Training, Room 101, Nell Hodgson Woodruff School of Nursing. Oct. 14-15: Fifth Annual Symposium on Regenerative Rehabilitation, Emory Conference Center Hotel. More info.
Oct. 20: Journey from Health Disparity to Health Equity. Virginia DeHaan Lecture by former Surgeon General David Satcher. 4:15, WHSCAB auditorium. Oct. 26: Medical dean's 2016 Emory Medicine Annual Address. 4:30 p.m., WHSCAB Auditorium, with reception following in lobby. Nov. 3: The State of Child Health in Georgia. Lecture by Brenda Fitzgerald, Georgia Dept of Public Health. 4:00, HSRB auditorium. Details. |