Beyond borders
Emory doctors bring their expertise to their Ethiopian colleagues
By Martha Nolan McKenzie
Photos courtesy of Patricia Hudgins and Ali Tahvildari
The gaunt teenage boy lay on the cot, his dark eyes registering only mild interest when the medical team parted the red and white candy-striped curtain that separated him from the other patients and approached.
Patricia Hudgins, an Emory radiologist, Dominique Cosco, an Emory general practitioner, and three Emory residents greeted the boy and his father, who stood next to the bed clutching a soiled bag containing his son’s medications and a much-folded, stained X-ray.
When the clinicians held the rumpled film up to a window, they saw a massively enlarged heart. This, along with the boy’s shortness of breath and distinctive heart murmur, confirmed the diagnosis of rheumatic heart disease and symptomatic heart failure. Back at Emory, the teen would have been scheduled for a heart valve replacement. But they were not at Emory. They were in the sparse emergency room of Black Lion Hospital in Addis Ababa, Ethiopia. Here, the best they could do was recommend that his symptoms be managed medically in the hospital, realizing that he would likely have to remain on his ER cot for several days before a hospital bed became available.
Welcome to medicine in Ethiopia, where there is one qualified doctor for every 35,000 people and where the advanced life-saving equipment and technology that are the stock and trade of U.S. health care are either very rare or nonexistent.
“The practice of medicine here is marked by lack—lack of human resources, lack of physical resources,” says Hudgins. “Yet the health care practitioners here are amazing in how much they are able to do with so little.”

A growing contingent
Hudgins and Cosco are part of Emory medical school’s rapidly growing involvement in Ethiopia, aimed at helping address that dearth. The lion’s share of Emory’s Ethiopian efforts center on a medical education exchange program funded by a U.S. government grant to the country’s largest medical school, Addis Ababa University (AAU). Emory also has received funds from the Bill & Melinda Gates Foundation for a project involving maternal and child health. And the dean of the School of Medicine has pledged more support through the Emory Global Health Residency Scholars Program.
“There are more Ethiopian doctors practicing in the United States than in Ethiopia,” says Henry Blumberg, an Emory infectious disease specialist and epidemiologist. “Physician shortage is a huge problem there, along with challenges in medical education and training, all problems that Emory is helping to address. We don’t want to be involved in medical tourism. Our goal is to make a difference.”
The medical school’s ramped-up efforts in Ethiopia began about two years ago. In January 2010, Emory was awarded an open-ended grant through the Bill & Melinda Gates Foundation to “…do something related to maternal and child health,” says Blumberg. “So we went to Ethiopia with money but no project. Our colleagues at AAU decided they wanted to put the funds toward making magnesium sulfate available to pregnant women for the treatment of pre-eclampsia and eclampsia.”
Pre-eclampsia is routinely treated in the United States and throughout the world with magnesium sulfate, “a pretty old and very cheap drug,” says Blumberg. For reasons that are not clear but likely related to profitability, there are no manufacturers or importers of the drug in Ethiopia. As a result, pre-eclampsia and eclampsia are the number two causes of maternal mortality in Ethiopia, behind hemorrhage.
Upon learning of AAU’s desired focus, Blumberg, an infectious disease specialist, recruited the aid of Jennifer Goedken, an Emory gynecologist. Goedken, Blumberg, and their team developed a standardized protocol for the drug’s use and created teaching materials in the form of posters and pocket cards. The original plan called for introducing magnesium sulfate use in Addis Ababa University’s three teaching hospitals (Black Lion, St. Paul’s, and Gandhi), but the AAU-Emory team also arranged partnerships with the Ethiopian Ministry of Health, the Ethiopian Society of Obstetricians & Gynecologists, and UNICEF. The influence of that partnership resulted in magnesium sulfate use being implemented in 107 public hospitals throughout the country.
This accomplishment, while laudable, pales when you consider that nearly 90% of the births in Ethiopia occur in the home. “The next step is to find a way to take magnesium sulfate beyond the hospital and into the community,” says Goedken. “We’ve put together a proposal for a pilot project to train community health workers to diagnose pre-eclampsia so they can refer patients to health centers. Emory already has a Gates grant through the nursing school to create a community-oriented strategy to improve maternal and newborn health in rural Ethiopia. We would like to add education about diagnosis and treatment of pre-eclampsia to what they are already doing.”
Separately in 2010, the National Institutes of Health unveiled a new initiative to strengthen medical education in sub-Saharan Africa. AAU garnered one of the five-year $10 million grants and chose to partner with Emory, along with three other U.S. universities. AAU is looking to Emory to help it meet two recent government mandates, increase the number of medical students and doctors trained each year and increase the number of subspecialties in which graduates can train. AAU’s medical classes jumped from 100 to 300, though its faculty count remained the same, and no faculty are trained in many of the subspecialties that are being planned.
Emory is approaching the task on a department-by-department basis. The Gyn/OB department, for example, met with their counterparts at AAU and discovered that while there is a residency program, there are no fellowships, particularly in the much-needed specialty area of gynecologic oncology. So in addition to Emory Gyn/OB faculty and residents giving lectures and doing teaching rounds, they are developing a curriculum for a gyn-oncology fellowship at AAU.
“Cervical cancer is a very big issue here because they don’t have Pap smears to detect precancerous stages, and they don’t have the resources to treat advanced stages of the disease,” says Goedken. “But beyond that obvious need, postgraduate training in a subspecialty such as gynecologic oncology can be a powerful tool in retaining faculty at Ethiopian medical schools. It gives them a path for advancement that they might not have had before.”
Many other Emory medical departments are in various stages along the same path. These include the departments of medicine (including infectious disease, pulmonary medicine, general medicine, and cardiology), radiology, surgery, pathology and laboratory medicine, and pediatrics (specifically, pediatric infectious diseases).

Back to the basics in radiology
Some departments have an easier time translating their skills and services than others. “If you are an infectious disease doctor who vaccinates kids against pertussis or gives TB medicine, there is a lot of opportunity for you to do global outreach,” says Hudgins. “You carry your stethoscope and medicine in your backpack. But if you’re a radiologist who uses $3 million MRIs, $1 million CT scanners, and $35,000 ultrasound machines, your outreach opportunities are a little more limited.”
When Hudgins and an Emory radiology resident arrived at Black Lion Hospital in March, they found one only CT scanner, which worked intermittently, a handful of ultrasound machines, and some film X-ray machines. No MRI. So even though the residents and faculty they encountered were extremely well-read, their hands-on experience was limited.
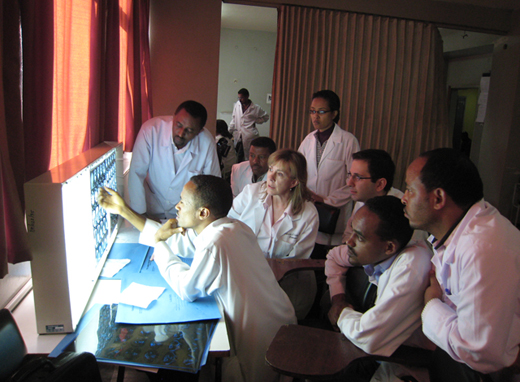
Yet the exchange of knowledge was equally valuable both ways. “None of my residents had ever touched a film X-ray before—it’s all digital these days,” says Hudgins. “And there is no file room in these hospitals. The patients are given their X-ray films, and they take them home with them and bring them back to future appointments. So the patient just hands you his film, and you’re reading it with him right next to you. That’s highly unusual in the United States where radiologists are usually off in our own corners. But it is exciting and helps remind us of what we’ve lost with all the subspecialization in medicine in the United States.”
Hudgins will be returning to AAU to help set up fellowship training in neuroradiology. “I’m putting together my suggestions for a one-year training program in neuroradiology,” she says. “Another Emory radiologist, Aarti Sekar, will lecture on body imaging—abdomen, chest, and pelvis. So we are slowly bringing more expertise in more areas.”
Training general surgeons
Surgery is another specialty that doesn’t translate as readily as others, but that has not stopped several members of Emory’s surgical team from making the trek, including Jonathan Pollock, a general surgeon. Pollock moved to Ethiopia in July through the Pan-African Academy of Christian Surgeons, which trains African doctors for five years to become general surgeons.
Like Hudgins, Pollock sees outreach opportunities that extend beyond the obvious. “There is a focus on infectious disease as a driving force of public health,” he says. “But there has increasingly been recognition that surgery is an important component of this.”
Pollock is not spending his time training surgeons to perform open heart surgery; rather he is working to develop proficiency in Cesarean sections, treatment of ulcers and fractures, and laparoscopy. One common problem for surgeons in Ethiopia is a typhoid perforation of the bowel.
“Not every surgical technique needs to be done by a fully trained [by Western standards] surgeon,” says Pollock. “While there is increasing specialization in Western medicine, with different clamps and forceps for every conceivable situation, in Africa, you have to be a true general surgeon and operate with only a few different instruments.”
So far Pollock’s program has trained four surgeons, two of whom have remained in the country. One is a general surgeon in rural Ethiopia—the only surgeon at the local hospital—and another is practicing in western Ethiopia in his hometown of 100,000 people where he is the town’s very first surgeon.
Emory medical school’s already significant presence in Ethiopia is set to expand, thanks to School of Medicine Dean Thomas Lawley’s recent commitment to fund the Emory Global Health Residency Scholars Program. These funds will support Emory residents and fellows to travel to Ethiopia, provided they have a link with an Emory faculty member. “This will really expand the number of people who will be able to go,” says Blumberg. “When it’s up and running, it will involve a series of monthly seminars in Atlanta and a one-month rotation in Ethiopia.”
Whether participating residents and fellows decide to pursue a career in global health or not, their time in Ethiopia will surely change them as physicians. “It’s so valuable to learn how medicine is practiced in other parts of the world, and we can bring that knowledge back to the United States,” says Cosco. “Physicians need to be creative about how to best deal with resource-limited patients. Here in Atlanta, at Grady Hospital, we have lots of patients who don’t have the funds to buy needed medicines or who have low health literacy. Global health can happen right across the street.” EM