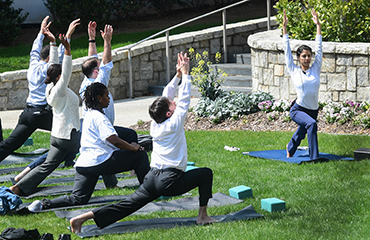If this message displays incorrectly, please view the web page

| APRIL 2017 | ||||||||
Notable
Doctors honored at Grady Gala The White Coat Grady Gala, celebrating Grady’s 125th anniversary while honoring health care heroes and the patients whose lives they saved, was March 18. A group of seven physicians who have each been actively practicing medicine at Grady for more than 40 years were presented with Lifetime Achievement Awards: Alfred Brann (pediatrics), Joel Felner (cardiology), Michael Lubin (general medicine), Sidney Stein (hematology & medical oncology), William Torres (radiology), Kenneth Walker (medicine/neurology), Nanette Wenger (cardiology). A record $1.8 million was raised at the gala, which was attended by more than 800 corporate, community, and philanthropic leaders. US News Rankings According to the most recent U.S. News & World Report rankings, the SOM ranks 23rd among research-oriented medical schools and 34th among primary care schools. Emory and Georgia Tech's joint Biomedical Engineering program ranks third. The physician assistant program remains third in the nation, and physical therapy remains fifth. For more, go here.
M. Hicham Drissi ((orthopaedics) has been named vice chair for orthopaedic research and professor of orthopaedics and cell biology. For more go here.
Robert Guyton (cardiology), Charles Ross Hatcher, Jr., Professor of Surgery and the director of the Thoracic Surgery Residency Program, was awarded the 2017 Presidential Citation by the American College of Cardiology. He received the honor at the ACC’s 66th Annual Scientific Session in Washington, D.C.
Tracey Henry (medicine) was selected as a 2017 Presidential Leadership Scholar. Over the course of several months, scholars will travel to participating presidential centers to learn from former presidents, key administration officials, and leading academics. For more go here.
The American College of Cardiology’s Fellows in Training (FIT) Section newsletter, ACC On-Call, recognized Emory cardiology fellow Salim Hayek as the “star FIT” for the month of March. Read his interview here.
Matthew Klopman (anesthesiology) was Doctor of the Day at the Georgia State Capitol on March 20. Medical Association of Georgia DOD volunteers work in the Medical Aid Station at the capitol building during the legislative session each year, providing free minor medical care to legislators and their staff. To find out more, go here.
Jeff Sands (medicine), Juha P. Kokko Professor of Medicine and Physiology, is president-elect of the American Physiological Society. Read more. Events April 6: How to Provide Feedback at the Bedside, noon-1 p.m., SOM 153A. RSVP here. April 13: Financing Your Retirement, 2 p.m., White Hall 207. RSVP here. April 22: Heel to Heal Superhero 5K, Lullwater Park Preserve. Hosted by the Emory Physician Assistant program Class of 2018 to raise funds for the medically underserved. More here. April 24: Charles R. Hatcher Jr., MD, Award for Excellence in Public Health presentation, 4 p.m., Klamon Room in the Claudia Nance Rollins Building. Recipient is William Eley, EAD for medical education and student affairs and professor of hematology and oncology. RSVP to Nancy Sterk, nsterk@emory.edu. April 25: State of the WHSC Address by EVPHA Jon Lewin, 4:30 p.m., WHSCAB auditorium. Reception to follow. May 10: Academic & Industry Intersection Conference, 9 a.m. to 1:30 p.m. Georgia Tech Research Institute Conference Center, "From Sensors to Big Data: Personalized & Population Health in the Digital Age." Keynote speaker, Neil Gomes, VP for Technology and Consumer Experience, Thomas Jefferson University and Jefferson Health System. More here. May 16: Dean’s Distinguished Lecture, May 16, 5:30 p.m. SOM 110, Nancy Newman (ophthalmology) will present "Mitochondrial Blindness: An Emory Story." Followed by award reception. |
|
Match Day Madness
Emotions swirled around the annual opening of the Match Day envelopes on March 17—screams, shouts, hugs, and tears. "But these are happy tears!" said Emma Goodstein (family medicine), who couple-matched at the University of Arizona, Tucson, with Bailey Lynn (emergency medicine). Emory SOM's Class of 2017 included 131 students participating in the National Residency Match Program (NRMP). Forty-four students will spend all or part of their residencies in Georgia, and 40 of those will remain at Emory. In addition, SOM students will receive residency training at other prominent institutions such as Duke, Brown, Johns Hopkins, Harvard, University of Massachusetts, NYU, and University of Washington. You can watch the excitement here. "The Match Day ceremony is a long-awaited culmination of hard work and perseverance that always proves to be one of the most thrilling times in the lives of our medical students," said William Eley, executive associate dean for medical education and student affairs. "Today our students learned they are headed to some of the top programs both here at Emory and throughout the nation to begin their careers as physicians." Some of the most popular specialties chosen by this year’s graduates were internal medicine (34), pediatrics (16), general surgery (13), emergency medicine (10), and family medicine (8). Prior to the NRMP match, three graduates matched into the military residency program, four matched in ophthalmology, and one matched in urology.
GME Leadership
The Graduate Medical Education program, under the leadership of Associate Dean Maria Aaron (ophthalmology) and Assistant Dean Philip Shayne (emergency medicine), oversees 104 programs with 1,266 residents, making it the seventh-largest GME system in the country.
Aaron leads many of the GME initiatives, such as core curriculum, residency tracks (including safety/quality, global health, and ethics), and mock accreditation reviews. Shayne oversees training programs and accreditation issues and leads wellness initiatives for residents and fellows. "Philip and I work very well together, as our strengths and interests complement each other nicely," says Aaron. "We have tried to transform the work of the Emory GME office from merely managing our 104 programs and maintaining accreditation to being innovative and forward-thinking, providing creative educational opportunities and creating graduates who become leaders in health care." Graduate medical education has changed in the past 20 years, says Shayne, with the adoption of duty hours, core competencies, milestones, and the Next Accreditation System. "It went from a system where programs were reviewed every five years to every year, in an attempt to figure out which programs were struggling," he says. With the beginning of the Clinical Learning Environment Reviews, the ACGME has placed increasing emphasis on embedding the GME leadership into the health care system. "We are no longer a stand-alone operation," Aaron says. "Gone are the days of simply interacting with residents/fellows, program directors, and chairs. Now, the GME leadership is much more visible and required to have facile interactions with hospital and health system administrators." In turn, the program directors' jobs became more demanding. "It used to be something you could do on the weekends," says Shayne. "Now, we manage a lot more complexity." The GME staff is responsible for licensing all 1,266 residents as well as keeping up with 14 participating affiliated institutions, including Grady, the Atlanta VAMC, Children's Healthcare, the Shepherd Center, and more remote clinics. "Our goal in working with program directors and coordinators is to provide guidance and shared resources for a confederation of strong residencies," Shayne says. "We want the program directors to feel that these are their residents." Most residents are funded through the federal Centers for Medicare and Medicaid, a process that is also managed by the GME office. Shayne served on the ACGME task force that recently refined the clinical learning environment, including new work hour requirements that maintain the weekly duty hour caps (including accounting for work from home) and give residents more flexibility within those hours. Programs are also charged with giving residents time for self-care. "People confuse long duty hours with hazing, but it’s really just preparation for what the real world in medicine is like," Shayne says. "The day you leave residency, you will independently begin taking care of patients. Residents need to be prepared for that." In addition, says Aaron, the changes improve patient safety by reducing the number of handoffs, providing more continuity of care, and enhancing educational opportunities. Cultivating Wellness
Hectic schedules and stressful events seem a bit more manageable after warrior poses on the grass and playing with furry therapy dogs. Centered on the theme of wellness and well-being, the fourth Annual Medical Education Day event was held on March 20 and was the highest attended so far, with more than 140 participants. In alignment with the SOM's strategic plan to address the issues of burnout and wellness in the workplace, the event was kicked off by keynote speaker Tait Shanafelt, MD, a cancer specialist and director of the Mayo Clinic Program on Physician Well-being, with a talk on “Cultivating Meaning, Balance, and Satisfaction in the Practice of Medicine.” A strong business case can be made for investing in efforts to reduce physician stress and foster engagement, said Shanafelt, who conducted a national survey that found more than half of US physicians report at least one symptom of burnout. Some antidotes: a sense of community, recreational opportunities, flexibility, and paying attention to/getting help for physicians who, at any stage in their careers, are experiencing distress. The event hosted 20 sessions with colleagues from the schools of nursing and public health and Emory Healthcare covering lively topics like maintaining the joy of practice, community resiliency and the iChill app, and a four-minute workout. There were presentations by SOM leadership, animal-assisted therapy, yoga on the lawn, cognitively based compassionate training, and "no strain, no pain" ergonomics. Posters, presentations, and booths highlighted campus resources such as Healthy Emory, FSAP, and Blomeyer Fitness Center. In additional wellness-related news, surgeon Carla Haack will be recognized as a Henry B. Tippie Clinician Scholar. This $2 million endowment will go toward Wellness Initiatives at the SOM and Emory Healthcare—Jay Patel (Strategic Initiatives)
|