$15.5 million NIH grant to fund study of vaccine effectiveness
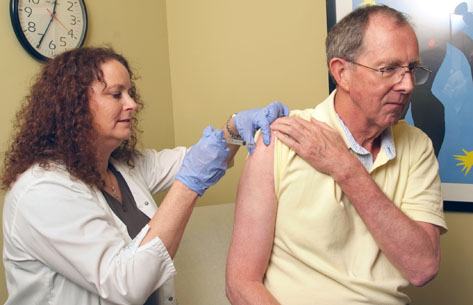 |
| Emory researchers will determine whether a "systems" approach involving immunology, genomics, and bioinformatics can be used to test and improve vaccine effectiveness in individuals. Currently, vaccines for flu, pneumonia, and shingles are ineffective in a substantial proportion of the elderly. |
The NIH has awarded a five-year, $15.5 million grant to researchers at Emory Vaccine Center at Yerkes to study human immune responses to vaccination to guide design of vaccines against HIV, malaria, and other global pandemics.
| |
 |
| |
Bali Pulendran |
| |
|
| |
 |
| |
Rafi Ahmed |
| |
|
The research will address a major challenge in vaccine development—that effectiveness of vaccination can be ascertained only after those vaccinated have been exposed to infection. To study vaccine-induced immunity in humans, they will use a multidisciplinary approach developed by pathologist Bali Pulendran, who is principal investigator. Rafi Ahmed, director of the Emory Vaccine Center, is co-PI.
Pulendran’s approach involves immunology, genomics, and bioinformatics to predict vaccine-induced immunity. This "systems" approach allows researchers to observe a global picture of the nearly 30,000 genes, proteins, and cells participating in immune responses to vaccination. Using this approach, the investigators have been able to identify signatures of gene expression in the blood a few days after vaccination that could predict with up to 90% accuracy the strength of the immune response to the yellow fever vaccine, one of the most successful vaccines ever developed.
The researchers will determine whether this approach can be used to predict the effectiveness of other vaccines, including common vaccines against flu, pneumonia, and shingles, which currently fail to launch protective immunity in a substantial proportion of the elderly. Read more.
Top
Start your engines! Emory Healthcare 500 will race on Labor Day weekend

Emory Healthcare has been named the title sponsor for Atlanta Motor Speedway’s Sept. 5 NASCAR Sprint Cup race—the Emory Healthcare 500. Labor Day weekend marks the return of night racing to the Atlanta track. Besides the cooler night air, read nine more reasons to spend the holiday weekend at Atlanta Motor Speedway.
| |
 |
| |
Terry "Mr. 500" Green will serve as grand marshall of the event. He is Emory's 500th heart transplant patient. Read more. |
| |
|
As part of a multi-year contract, Emory Healthcare also will serve as the official health care provider of Atlanta Motor Speedway, providing health care screenings and educational programs during the event for fans and visitors.
“Partnering so closely with NASCAR and the Atlanta Motor Speedway is a chance to support and thank the many valued patients and physicians in the Henry County and Southern Crescent region who allow Emory to serve them for cutting-edge medical care,” says John Fox, Emory Healthcare president and CEO. "We look forward to making this an incredible and memorable weekend as well as a lasting partnership with the local communities we have had the honor and privilege to serve for so long."
Read more.
To purchase tickets, call 877-9-AMS-TIX or visit the AMS website.
Top
Emory's drug discovery center selected to target glioblastoma
| |
 |
| |
Haian Fu is the grant's principal investigator. |
| |
|
Emory's Chemical Biology Discovery Center has been selected by the National Cancer Institute for a $1.5 million task order to study genomic alterations in glioblastomas, the most deadly of adult brain tumors. Emory is one of only two centers funded for this task.
To discover a target for a new cancer drug, scientists must find the proteins that are made by altered genes and study the interactions between those proteins within their network in a tumor. Drugs can disrupt those networks and inhibit or promote the activity of a particular target protein.
To search for effective drug therapies against glioblastoma, Emory scientists will use high-throughput technologies—robotics equipment that automatically handles thousands of liquids and chemical assays in minute quantities and then computes and analyzes the resulting massive amounts of information to screen compounds against protein targets.
Emory is part of the NCI's Chemical Biology Consortium, which is focusing on a new national effort to convert genomic information into new therapies. Despite the fact that first draft of the human genome was completed 10 years ago, this information's impact on diagnosing and treating disease has yet to be realized, and the NCI is working to glean more practical benefit from genomics data. Read more.
Top
Buildings to be improved to reduce energy, water consumption
| |
 |
| |
Whitehead Biomedical Research Building |
| |
|
Emory University has hired Siemens Industry to retrofit campus buildings to improve their energy efficiency and decrease water consumption. The health sciences buildings included in the first phase of the project include Rollins School of Public Health, 1525 Clifton Road building, and the Whitehead Biomedical Research building.
Improvements include replacing inefficient lights and plumbing fixtures
and repairing windows and doors to reduce air leakage.
Read more.
Emory also has started composting its lab animal bedding.
Read more.
Top
Helping patients navigate the payment process
One in a series of profiles of people in the Woodruff Health Sciences Center
| |
 |
| |
Adam Gobin |
| |
|
Adam Gobin works with the part of health care that many people find most confusing: helping patients navigate the payment process and sorting out who pays for which clinical services.
As part of his job as an Emory Clinic operations/business manager, Gobin oversees 28 clinic financial counselors who meet with patients to discuss outstanding bills as well as ways they can obtain assistance with payments.
He and his team also help patients anticipate what their obligations will be before they see the doctor. When Gobin began working at Emory two years ago, his supervisor, Taylor Williams, had just initiated something called patient portion pricer (PPP) to help keep patients from being blindsided by bills. PPP counselors call insured patients a couple of weeks before an appointment or procedure to advise them exactly how much their insurer will pay for the upcoming service and how much they will need to pay. Many patients have only a vague idea what their insurance contract promises, so they appreciate the explanation and heads-up, says Gobin, who helped Williams roll out PPP to the entire clinic.
PPP has resulted in earlier payments, but more important, Gobin says, is the dramatic reduction in complaints from patients who are puzzled as to why Emory sent them a bill in the first place.
Life also became smoother for patients and previously overwhelmed financial counselors when Gobin implemented a financial counseling call center to handle insurance verification and other administrative details that can be addressed by phone. This freed counselors to spend more time face to face with patients with more complex issues.
Biostats:
• Program Manager, Emory Clinic
• Operations and Planning Coordinator, Emory Clinic
• Intern, Emory Clinic
• Intern, Athens Regional Medical Center
• BA and MPH (administration), UGA
|
|
| |
|
But the most "revolutionary" initiative, says Gobin, has been getting input and advice from actual patients and family members who know firsthand what it's like to interact with clinic financial counseling. Getting such feedback is part of Emory Healthcare's care transformation program, designed to ensure that patients' voices are heard in every facet of care, including the payment process.
Another part of Gobin's job is figuring out who should pay for clinical services provided as part of a clinical trial and then billing appropriately. Appropriate billing is a crucial part of compliance with research regulations, says Gobin, with stiff sanctions imposed for even inadvertent clerical errors. Attention to such details is also an important part of patient safety because it provides additional opportunity to track patients involved in research studies.
Gobin believes his staff and colleagues are "the best possible" and finds creative ways to express enthusiasm. He created a blog so his co-workers could see his videos of them "having fun and enjoying coming to work." And his personal blog contains an account of his participation in a clinical trial in Emory's predictive health program.
Top
Brain boot camp in med school simulation lab
| |
 |
| |
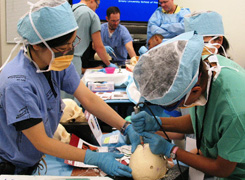
FIrst-year neurosurgery residents practiced drilling and craniotomy. |
Neurosurgery hosted a two-day boot camp for first-year neurosurgery residents in July as part of a new national course launched by the Society of Neurological Surgeons in six cities throughout the country.
The course focused on fundamental skills, patient safety, professionalism, and communications. Day 1 consisted of traditional lectures; in day 2 participants practiced in simulated operating room environments and performed re-created bedside neurosurgical procedures.
Equipment for the training, including synthetic skulls, was loaned and donated by six corporate sponsors. Residents practiced skills relevant to all first-year residents, such as line placement and suturing, as well as neurosurgical skills like drilling and craniotomy.
According to neurosurgeon Costas Hadjipanayis, one of the Emory organizers and course directors, the 37 interns from universities across the region who participated in the Atlanta training was the largest number nationwide. View story on CNN.
Top
|
|
 |
|
From the
Interim EVPHA
 |
| Wright Caughman |
|
A transformative experience
It wouldn't be an exaggeration to say that the Woodruff Health Sciences Center (WHSC) has transformed my life. Since I joined the dermatology faculty in 1990, I've had the good fortune to experience WHSC from many different perspectives—physician, educator, researcher, and administrator—and to work alongside some of the most talented and dedicated people I've ever known. The amount I've learned from my colleagues, students, and patients over the past 20 years is humbling, and I'm still learning every day. I'm a different—and I hope better—person as a result.
It's not surprising that WHSC has transformed me because that's really the nature of what we do. I think all the people whose lives intersect with WHSC find themselves transformed in some way. Our students find their futures transformed as a result of the comprehensive, cutting-edge health education they receive here. Our patients and their families find their lives not only changed, but often saved, by the compassionate, high-quality medical care they receive here. And our faculty and staff are transformed, as I have been, by working in a collegial environment with opportunities for learning and growth and the knowledge that they're making a lasting and tangible difference through the work they do.
And now WHSC itself is being transformed as we adapt to the rapidly changing external environment. The economy, health care reform, and other external developments require us to rethink the way we do business, and that's not necessarily a bad thing. I prefer to view the changing environment as a context for positive energy—an opportunity to re-examine old ways of thinking and doing things and to embrace new ideas that will propel the health sciences to new levels of success. After all, we'd rather lead change than have it happen to us. If we're going to continue transforming lives, we'll have to start by transforming ourselves, and I look forward to working alongside you in my new role as we explore the possibilities that lie before us.
As I begin to serve in my new role today, I thank Dr. Fred Sanfilippo for his leadership and vision over the past three years. Fred is a leader who understands the need for change and never shrinks from it, and WHSC is stronger for having had him as its CEO.
I look forward to continuing our collective transformation because I know WHSC will always change for the better. Together, we have the chance to become both wiser and more impactful. It's a journey I look forward to taking with you. Please let me know your thoughts and suggestions at evphafeedback@emory.edu.
Editor's note: Read a bio of Wright Caughman in the Aug. 30 issue of Emory Report.
In brief
Increase in applications to nurse practitioner programs
 |
| Nurse practitioner Michelle Mott is a nursing faculty member and associate CNO at The Emory Clinic. |
| |
The number of applicants to the nursing school's nurse practitioner programs has risen dramatically in the past year:
• Adult NP 16%
• Family Nurse Midwife 35%
• Family NP 20%
• Pediatric Acute Care NP 71%
• Pediatric Primary Care NP 112%
• Women's Health NP 20%
Nursing faculty attribute the growth to health care reform and the increased need for primary care.
Tobacco use surcharge for 2011
To promote health and wellness for employees, Emory Healthcare is instituting a surcharge to its medical insurance premiums for EHC employees or spouses/SSDPs who use tobacco products. The $50 monthly surcharge will take effect Jan. 1. To address tobacco use, EHC conducted focus groups with employees in 2009. Overall, the employees, even the smokers, agreed with the surcharge, given the ample tobacco cessation resources available at Emory. There will not be a tobacco use surcharge for university employees in 2011.
Emory in talks with St. Joseph's
A recent communication from Emory Healthcare President and CEO John Fox to EHC staff and physicians alerted recipients to an Aug. 13 article in Atlanta Business Chronicle about a potential collaboration between St. Joseph's Hospital and EHC to explore formation of a joint operating company. Such a venture would allow the two organizations to integrate services and share operational costs while maintaining separate boards of directors. Fox specified that while a non-binding letter of intent had been executed, conversations had just begun and were anticipated to continue for at least 30 days. No decisions on financial commitments or structure of the relationship had been made, and any affiliation would have to be approved by all levels of Emory governance.
Ethics center plans expansion
As described in an Aug. 20 article in the Atlanta Business Chronicle, the Emory Center for Ethics has plans to raise up to $20 million to transform itself into a global think tank on ethical issues. Center director Paul Wolpe, who was recruited to Emory two years ago from University of Pennsylvania, spoke in July at the first meeting of the Presidential Commission for the Study of Bioethical Issues in Washington, D.C. Emory President James Wagner is vice chair of this commission, which will hold its Nov. 16-17 meeting at Emory (topic: synthetic biology).
Notables
Cardiovascular nurse researcher Sandra Dunbar is associate dean for academic advancement in the nursing school, effective Sept. 1. She will be responsible for recruiting faculty, overseeing faculty promotions and assisting them in creating professional development plans, and establishing mentorship programs for junior faculty. Read more.
Jeffrey Lennox is associate dean for clinical research in the medical school, effective Sept. 1. In this new role, he will enhance clinical trial performance. He serves as infectious diseases section chief at Grady Hospital and co-director of the clinical research core at the Emory Center for AIDS Research.
Grady trauma surgeon Jeffrey Salomone has been appointed to the National Emergency Services Advisory Council of the U.S. Department of Transportation. Read more.
Nursing faclty member Ora Strickland is the 2010 Distinguished Faculty Lecturer at Emory and the inaugural recipient of the Mary Elizabeth Carnegie Award. Carnegie was a pioneer in breaking down racial barriers in nursing in the early 1900s.
Upcoming events
Sept. 5: Emory Healthcare 500, 7:30 p.m. Atlanta Motor Speedway. Read more.
Oct. 12: Medicine State-of-the-School address, 5:00 p.m. WHSCAB auditorium. Reception to follow in med school lobby.
Oct. 30: American Heart Association's annual Heart Walk. For more information, contact Adam Tribbett, 404-778-2926, adam.tribett@emoryhealthcare.org.
|

