Nursing advocates at the state capitol |

New EUH bridge opens next month |

New ICU at EUH Midtown |
 In brief |
|||||
| January 27, 2015 | ||||||||||||||
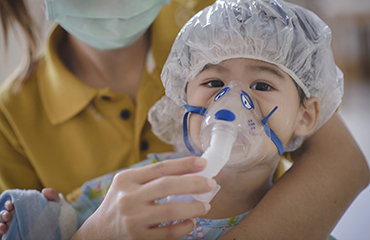
Getting closer to an RSV vaccine
Crafting a vaccine against RSV (respiratory syncytial virus) has been a minefield for 50 years, but researchers here and at Children's Healthcare believe they have found a possible solution. As they reported in the Dec. 21 issue of Nature Communications, they have engineered a version of RSV that is highly attenuated—weakened in its ability to cause disease—yet potent in its ability to induce protective antibodies. When used as a vaccine, it can protect mice and cotton rats from RSV infection.
"Our research shows that it's possible to attenuate RSV without losing any immunogenicity," says senior author Martin Moore (pediatric infectious diseases). "This is a promising live-attenuated vaccine candidate." The next steps, he says, are to produce a clinical grade lot of the vaccine and conduct a phase 1 study of safety and immunogenicity in infants. Past efforts to develop a vaccine have met with frustration. In the 1960s, an attempt to develop a vaccine by chemically inactivating RSV, as in a standard flu shot, backfired. Exposure to this vaccine actually made natural RSV infection in infants worse. More recently, a clinical trial of a protein-only RSV vaccine in older adults showed disappointing results. Several successful vaccines against other viruses, like measles, polio, and mumps, have been created by weakening the viruses in cell culture. Weakening RSV in this way hasn't worked out satisfactorily, says Moore. "It turns out that for RSV, the natural virus does not induce a lot of immunity itself." Instead, Moore and his colleagues engineered RSV to enhance production of a key protein, called F (for fusion). F is critical for RSV's ability to enter cells and is the target of several vaccines in development. By making mutations in the viral gene that encodes F, the researchers also made the virus more stable with respect to heat, which could help vaccine manufacturing and distribution. At the same time, the researchers removed or weakened several other viral genes that promote infection and suppress the immune system. One measure of this is that the modified virus, called OE4, stimulates high levels of antibody production. Emory has optioned the vaccine technology to a startup company, Meissa Vaccines, Inc, which was co-founded by Moore, who serves as chief scientific officer. Read more about how the team made the re-engineered virus less likely to mutate back to its original form and how they determined through viral structural visualization that OE4 is both highly immunogenic and highly attenuated.—Quinn Eastman Advocating for nurses and patients
On January 12, 75 nurses from Emory and other health systems gathered "under the gold dome" for a legislative kickoff day sponsored by the Georgia Nurses Association (GNA). Their mission: to deliver care packages and a personal message about 2017 legislative priorities to every Georgia lawmaker. Each nurse was assigned two to four legislators, whom they tracked down and spoke with in the hallways outside the House and Senate chambers. "It's easier to connect with legislators at the beginning of the session," the nursing school's Suzanne Staebler told the group of nurses who shadowed her that day. "The further into the session, the harder it is to connect with them. Legislators are less willing to step out of the chamber to meet you, especially if there's a vote coming." Staebler is at home in the advocacy arena, having led national nursing organizations and held major fellowships in health policy. In addition to directing Emory's Neonatal Nurse Practitioner Program, she directs advanced practice for GNA. Whatever the setting, she can take the bull by the horns. "I'm from Texas, and I can rope a calf," she told Representative Vernon Jones upon running into him at the state capitol. She then segued to tell him about this year's legislative priorities, including the licensure compact, which would speed up the licensing process for nurses from other compact states and allow them to enter Georgia's nursing workforce more quickly. Jones was familiar with the idea. "You're talking about reciprocity," he said. Similar to a driver's license, compact licensure allows nurses to receive reciprocity in accordance with state standards of practice. Currently, 25 states offer compact licensure, including North Carolina, South Carolina, and Tennessee, which all border Georgia. In times of disaster, compact licensure would allow nurses from those states to assist quickly.
By mid-afternoon, the nurses at the capitol had accomplished their mission, including Emory Healthcare's Mary Gullatte, corporate director of nursing innovation and research. Gullatte has walked the capitol hallways many times, initially in support of prescriptive authority, which became Georgia law in 2006. "The best way to make policy change is from the inside out," says Gullatte, a longtime state and national nursing organization leader. "Legislators need and want to hear about issues that are important to us to help them decide how to vote on health care legislation, whether it has to do with patients or our profession." Three years ago, Gullatte proposed formation of the Emory Nurse Legislative Council (ENLC) to coalesce EHC nurses and nursing faculty and students around health advocacy. The group meets quarterly and last fall hosted a health care advocacy forum featuring Senator Renee Unterman and Representative Sharon Cooper, two of three nurses who serve as Georgia legislators. When Gullatte proposed the ENLC, she did so with one caveat. "I didn't want to be the one to lead it," she says. "I wanted to mentor other nurses interested in changing health policy." EHC nurses Julie Swann and Barbara Hill stepped up to co-chair the council. Swann attended her first state legislative session in 2015. "It's a great way to get your foot in the door and talk with legislators about what's important to nursing," says Swann, VP of patient services and CNO for Emory Saint Joseph's Hospital. Last year, Governor Deal signed a law raising the penalty for assaulting emergency services and hospital emergency room personnel. Hill, an ER nurse, was key in revitalizing the bill that Deal signed. It's one of the laws that other EHC nurses have supported and discussed in the workplace. "Assaulting nurses and others in the ER is now a felony," says Swann. "We have to consider what we do at the bedside to make sure we're upholding the law to its full capacity. Does it apply to all patients? What if it's a patient who lashes out because they are ill or hurt and don't know any better? And what if it's a patient who intentionally tries to harm you? We have to put a context around it to educate nurses about it." Staebler is equally intent on teaching nursing students how to be strong advocates at the start of their careers. In her policy, ethics, and law course, she invites legislative staffers and lobbyists to critique her students' presentations. Students often accompany her to the state capitol to talk with legislators. Those visits "help nurses and nursing students develop tools for their tool kit later on," Staebler says. "So many things can impact their practice. We have to know how to advocate for our profession and our patients. We have to be our own voice."—Pam Auchmutey New EUH bridge opens next month, old bridge demo begins
The sleek new bridge concourse connecting the original Emory University Hospital building with buildings on the other side of Clifton Road is slated to open Monday, February 20, marking a major milestone toward opening of the new hospital tower later this year. Because the new tower itself will not be open yet next month, only the lower level of the bridge will be accessible. The bridge's lower and upper levels connect to the second and third floors, respectively, of each hospital building. The bridge's lower level connects to an area of the new tower allowing access to clinics A and B and Winship. The bridge's upper level is expected to be operational in April. When the new bridge opens next month, foot traffic will transition immediately from the old to the new bridge. The old bridge will close for demolition, with tear-down tentatively scheduled to begin the last weekend in February, starting Friday evening, February 24, after rush hour (date and time dependent on weather). Access to Clifton Road and to the new bridge will be restricted over this weekend, with restrictions expected to be lifted on Sunday evening, February 26. Watch for more details in an all-Emory email, including a traffic advisory, that will be sent closer to February 24. The bridge's lower level will be for public and staff use, and the upper level will be used for patient transportation.
Last month, Emory University Hospital Midtown opened a new 18-bed, state-of-the-art intensive care unit, complete with e-ICU technology, a team "theater" for patient observation, and spacious rooms. "The large rooms allow for families to stay with loved ones, while giving providers plenty of space to care for the patient in designated 'clinical zones,'" says Susan Kill, specialty director of critical care services. Twelve of the 18 beds in the unit are open, with the remaining six beds to open later this year. Six of the beds are negative-pressure rooms, which prevent contaminated air from leaving the room. Three of the rooms have special lifts for bariatric patients. The unit's observation theater has eight TV screens affixed to the wall, allowing interdisciplinary teams to round and discuss patient care while monitoring different patients in their rooms. The unit also includes a family welcome center, a family conference room, a staff conference room for education, and a staff retreat area, complete with aroma therapy, couches for relaxing, and a massage chair for stress relief. "We also included extra amenities for our staff to give them a place to relax during their breaks," says Cheryle Collins, unit director. "Caring for extremely sick patients in an ICU can be very stressful, so making sure staff have downtime in a positive environment is important." The new unit brings new job opportunities for the nursing profession. Additional critical care nurses and other nursing staff are being hired to work in the new ICU and throughout other parts of the hospital. Read more. |
| From the Executive VP
Always on our mind...
Here at the Woodruff Health Sciences Center, we're working 24 hours a day, seven days a week toward a healthier world. As you'll read in Eight Days a Week, the 2016 community benefits report, the more than $72.3 million in charity care that we provided to the poor, the uninsured and underinsured, children and seniors, and many others in need made a lasting and tangible difference in the lives of thousands of people in 2016. Together our research, education, and health care missions have a $7.5 billion impact on the community, in addition to the immeasurable value of providing help and hope to people in need all day, every day. Thanks for all that you do to make it possible for us to be here around the clock for all the people who depend on us. I wish you much health and happiness in the year ahead!
The inauguration of Claire E. Sterk as Emory's 20th President will take place on Wednesday, Feb. 8, 10-11:30 a.m. in Glenn Memorial Auditorium. The ceremony will include a grand procession of dignitaries and academic delegates from around the world, a keynote address from Emory neurosurgeon Sanjay Gupta, a performance by the Vega Quartet, and reading of a commissioned poem by Kevin Young, director of the Schomburg Center for Research in Black Culture. A live webcast will be available. Among several events scheduled to celebrate the inauguration is a symposium on Health Challenges and Bold Opportunities on Tues., Feb. 7, 7:30-9:00 p.m. Check ticket availability. Nursing ranks first in NIH funding
With $7.8 million in NIH funding for fiscal year 2016, the nursing school ranks first among nursing schools for NIH funding. The school has risen steadily in this ranking in the past few years—from 38th in 2009 to fourth in 2015 to its current position as the nation’s top-ranking nursing research program. Read more. NIH taps "omics" capabilities in Atlanta
A metabolomics, proteomics, and lipidomics ("omics") analytics team led by Emory with collaborators at Georgia Tech will receive $13.6 million over six years from the NIH as part of a national effort to create a map of the molecular changes that occur in the body in response to physical activity. The information they uncover could help researchers and doctors develop personalized exercise recommendations. Read more. Budd Terrace receives fifth five-star rating U.S. News & World Report named Budd Terrace a Best Nursing Home, based on its five out of five-star rating from the Centers for Medicare & Medicaid Services (CMS) for excellence in quality, safety, and adequate staffing. Out of 358 nursing homes in Georgia, only 26 received an overall rating of 4.5 stars or above for 2016-2017. Budd Terrace is beginning its fifth consecutive year as a five-star rated facility, which places it in the top 20% of skilled nursing facilities in the U.S. under CMS’s criteria. Read more. Notable
Elisabeth Binder (psychiatry) was awarded the Eva King-Killam Research Award from the American College of Neuropsychopharmacology. Read more.
Diane Cassels recently retired from her position as chief administrative officer at Winship Cancer Institute after a 24-year career at Emory, in which she served a number of leadership roles. Another long-time Emory leader, Babs Hargett, corporate director in the Office of Quality and Risk, retired this month after 42 years at Emory. Maggi McKay also retires this month after 17 years at Emory—under her leadership as VP for Health Sciences Development, the Woodruff Health Sciences Center raised more than $1.1 billion since 2008.
Carolyn Clevenger has been appointed associate dean for clinical and community partnerships, effective in June. Read more.
Andrea Crowell and Jeffrey Rakofsky (both psychiatry) received the 2017-2018 Faculty Innovation in Education Award from the American Board of Psychiatry and Neurology. Read more.
Carlos del Rio (infectious diseases and chair of global health in Rollins School of Public Health) has been appointed interim executive associate dean of clinical services for the medical school's Grady campus.
Jaffar Khan (neurology) has been appointed assistant dean for education in the medical school, a role in which he is the primary liaison between the medical school and Grady Hospital in matters concerning undergraduate and graduate medical education.
Heart surgeon Douglas Murphy, who practices at Emory Saint Joseph's Hospital, achieved a world record after completing his 2,000th robotically assisted heart surgery. He performed Georgia's first robotic heart surgery at ESJH in 2002. Read more.
Kelly Wiltse Nicely is program director of the new nurse anesthesia track in the nursing school's DNP program.
Raymond Schinazi (pediatrics) received the Scrip Lifetime Achievement Award last month. Read more.
Dong Moon Shin (hematology, Winship) was named a fellow of the American Association for the Advancement of Science. Read more.
Mylin Torres (radiation oncology, Winship) was selected to hold the Louisa and Rand Glenn Family Chair in Breast Cancer Research and was named director of the Glenn Family Breast Center at Winship. Event May 10: Eighth Annual Academic & Industry Intersection Conference. Georgia Tech Research Institute Conference Center. |