

|

|

|
May 20, 2014
Nursing school renovates its sim lab
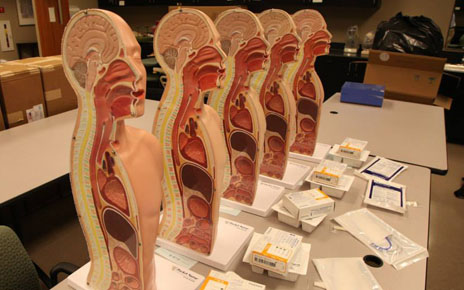 |
The nursing school has taken in 34 important new tenants. They range in age from infancy to senior and reside in quarters on the school's plaza level.
They are simulation manikins, and they are part of a multi-phase renovation to the school's "sim lab."
 |
|
| Kate Moore |
"We have outgrown our lab," says Kate Moore, director of the Evans Center for Caring Skills, as the lab is known. "Our enrollment has increased 127% since the nursing school's building opened in 2001, and we had not updated our sim lab since 2005. Simulation technology has advanced significantly since then."
The school has bought 18 low-fidelity manikins, suitable for practicing catheter insertion, CPR, and wound dressing, and 12 VitalSim manikins (four each of adults, children, and infants), which can be programed through a hand-held device and used in any classroom.
"Faculty can use the device, which is like a tiny iPad, to record phrases that the manikin will say in a scenario in a gender- and age-appropriate way," Moore says.
For blood pressure readings on the Vital Sim manikin, students can listen to Korotkoff sounds that are controlled by the instructor with the sim pad. Previously, students practiced on each other and relied on a teaching stethoscope for confirmation of sounds, says Moore.
"Students are going to come away from this simulation with a much higher level of competence and confidence," she says. "On these manikins they can feel the pulse, and the instructor can adjust the pulse to be easier or harder to gauge."
The VitalSim manikins also have heart, lung, and bowel sounds, allowing students to hear normal and abnormal sounds.
One SimMan Essential also joined the team for teaching airway, cardiac, and circulation management. "I can give him a blood clot in his leg and make his pulse disappear," Moore says. "Students can find his pulse rate by palpation rather than having to rely on a monitor screen for a digital display of the pulse rate.
"Many people who go into nursing are kinesthetic learners—they learn by doing—so simulation is being integrated into every nursing course," Moore says.
The sim lab has expanded into additional classroom space, and by 2017, Moore hopes to add birthing and premature infant manikins and to build simulated hospital rooms. The nursing school also is hiring a full-time facilitator who will help run the lab and will be available to tutor students.
"One of the things we've heard from students is that they wish they had more time to practice their skills," she says. "We want to give them as much opportunity as possible to do so. Consistent use and practice on our manikins will help ensure that they are highly competent when they care for real patients." —Kay Torrance
 |
Pablo Picasso once said that art is the lie that enables us to realize the truth. He probably would have cast an approving gaze on the artwork in the Rollins School of Public Health.
On the walls of the school's two buildings, for example, hangs a rotating poster collection that addresses some of the stickiest topics of public health—obesity, mental health, sexually transmitted diseases. The posters, colorful and thought provoking, are popular with faculty, staff, and students, says Dean Surbey, RSPH's executive associate dean for finance and administration.
After the Claudia Nance Rollins (CNR) Building opened in 2010, a staffer from the CDC asked Surbey if he would like to display a poster collection about hand washing. He didn't see the art beforehand, and "taking a huge leap of faith, we hung up nine great graphics and hosted a reception." The artwork was a hit.
"We really didn't want to take them down, so the CDC gave them to us," he says.
The posters were created by students of Mary Campbell at the Portfolio Center, an Atlanta design and illustration school. Surbey then contacted Campbell for more posters, and the two worked out a plan: he would give her a public health topic twice a year for her class (now once a year). Coming up at the end of June is a set of posters on health disparities.
"We get emails and lots of comments on the posters. They are mostly positive, but we usually manage to offend someone," Surbey says.
Someone was offended that one poster labeled a woman with a "muffin top" as obese, "but that was the point," he says. The mental health posters generated more comments than any other group of posters. The posters educate and raise awareness about public health topics that are often sensitive, and Surbey doesn't want to change that. "People want to come to Rollins to talk about public health," he says.
The mental health poster series is displayed on the CNR Building side of the bridge, and obesity posters are now located in its stairwell; hand-washing posters are in various restrooms in both buildings and on the first floor of the Grace Crum Rollins (GCR) Building.
 |
|
| Image from "The ThrowAways" |
Also in the GCR on the bottom floor is a photography exhibit, "The ThrowAways," on sex trafficking by artist Charlotte Watts 13C. Watts took photos and put them atop light boxes to simulate the lights of a highway and the neon lights of businesses. Other photography exhibits include Kenya in a GCR stairwell and Emory photographer Brian Meltz's work on Haiti on the plaza level of the GCR. —KT
 |
|
| Jane Bordeau |
Jane Bordeau can't remember the exact day she decided to leave bedside care to become a clinical research nurse. But she knew for certain that she wanted to do more to help patients with debilitating disease. She found her niche in the Emory ALS Center, one of the nation's largest clinical and research centers for patients with amyotrophic lateral sclerosis, the fatal disease that causes the deterioration of cells in the brain and spinal cord that control muscle movement.
Serving as a clinical research nurse in the Emory ALS Center enables Bordeau to broaden her skills and her impact on patients. "One day you're in the clinic with patients, the next day you are filling out a regulatory document," she says. "The subject and I are generating the data together—it's not just me entering a bunch of numbers. As a nurse in research, there still is a human aspect."
Bordeau works with neurologist Jonathan Glass and neurosurgeon Nick Boulis, who are testing the injection of human neural stem cells into the spinal cord as a possible treatment. The researchers currently are in a Phase II trial in which ALS patients are given more injections with more neural stem cells. In Phase I, patients received a maximum of 10 injections of 100,000 cells per injection during surgery. In Phase II, patients receive a maximum of 20 injections and up to 400,000 cells per injection. The study is the first U.S. clinical trial of stem cell injections into the spinal cord for ALS treatment.
"It's the best shot that we've seen so far," says Bordeau of the stem cell procedure. "It's not a cure, but we think it can slow the disease. We think the stem cells will protect the neurons that are not damaged and prevent others from further deterioration."
Bordeau monitors and assesses the study participants, testing their physical capabilities after surgery. She organizes the data in a computer database for reports and publications in journals.
"I want to see what happens," she says of the research. "This disease is rare, thankfully, but there is no treatment or cure. One medication can prolong life for a short time but does very little to improve quality of life, leaving patients exhausted. An antibiotic has not proved fruitful in clinical trials.
"If this study can help in any way in moving our knowledge forward to help these patients, that will mean a lot to me."—KT
Cost-reduction initiative: A look at the first year
 |
|
| Wright Caughman |
Participation in the first year of our cost-reduction initiative has been outstanding across all units of the Woodruff Health Sciences Center, yielding more than 700 faculty and staff ideas to date through both the WHSC and Emory Healthcare collection websites. A multidisciplinary team has reviewed the non-health care specific ideas and identified the following short list of the most frequently submitted, simple, and universally applicable cost-saving measures. As you'll see, many of these measures also dovetail with the University's commitment to sustainability, making them doubly beneficial.
Direct reductions:
• Reduce travel expenses as much as possible.
• Minimize the number of meals provided for meetings.
• Ensure that all overtime for hourly employees is pre-approved and has a legitimate business purpose.
• Minimize shipping and courier expenses.
• Review vendor contracts and renegotiate more favorable terms where possible.
• Ensure that gifts to employees adhere to the finance department's guidelines.
Behavior changes:
• Turn off lights in non-essential areas when not in use and at the end of each day.
• Provide reusable cups, rather than disposable cups, in break rooms.
• Ensure that building temperatures meet the University's maximum/minimum policy and adhere to the policy prohibiting the use of space heaters.
• Reduce paper use and printing costs by doing as much work electronically as possible.
• Print double-sided and in black and white.
• Provide recycling bins in the common areas of all facilities.
• Urge staff to refill their own reusable bottles/cups rather than providing bottled water.
• Share or repurpose excess supplies rather than disposing of them.
Although many of these may seem like small measures, spread over more than 20,000 people, they have the potential to significantly impact our ability to deliver on our research, education, and patient care missions. After all, every dollar we save is a dollar we can invest in meeting the needs of the people we serve.
Please let me know how you're implementing the measures above in your own areas, as well as any other measures you're taking to reduce costs, and thank you for your ongoing stewardship and support.
Please direct questions and comments to evphafeedback@emory.edu.
 |
NSF awards Rollins $2.5 million grant
 |
|
| Justin Remais |
The National Science Foundation awarded a five-year, $2.5 million grant to the Rollins School of Public Health to develop new computational approaches to predict infectious disease risk resulting from changing climate. "We need models capable of estimating the impact of climate change on water quality and waterborne disease so we can devise strategies to moderate potential future risks," says principal investigator Justin Remais (environmental health). His research team will develop open-source computational models of surface water quality and waterborne disease risk that account for relationships between meteorological phenomena and pathogen growth, survival, and transport, using test sites in western China and northern Ecuador. Read more.
Faculty awards at commencement
 |
|
| Carlos del Rio |
Carlos del Rio, chair of the RSPH Hubert Department of Global Health, received Emory's Thomas Jefferson Award at commencement for service to the university and the greater community. Del Rio co-directs the Emory Center for AIDS Research (CFAR) and is program director of the Emory AIDS International Training and Research Program. In October, he was elected to the Institute of Medicine, one of the highest distinctions in health and medicine.
This year's recipients of the Emory Williams Award for Distinguished Teaching include Kimberly Jacob Arriola (behavioral sciences and health education), Thomas Dodson (vascular surgery), and Tami Thomas (nursing).
Health Care Heroes 2014
Emory was well represented at the Atlanta Business Chronicle's Health Care Heroes award ceremony last week, with four winners out of seven categories and three finalists: Winners include Kirk Kanter (surgery, health care innovation), Kate Moore (nursing, military service), Will Sharp (pediatrics/Marcus, allied health professional), and Mylin Torres (Winship, rising star). Finalists include James Eckman (hematology, physician category), Raul Nogueira (neurology, physician category), and Robert Mannino (BME PhD student, rising star). Read more.
Exhibit pays homage to Emory Medical Unit in world wars
 |
The stories of Emory doctors, nurses, and enlisted men who comprised Base Hospital 43 during World War I and II are the focus of "When the Emory Unit Went to War," an exhibit at the Woodruff Health Sciences Center Library that runs through March 2015. The exhibit features diary entries, scrapbooks, photographs, uniforms, and books about the unit. "The exhibit is a way to let students and the larger community know about this unique part of Emory's history," says its curator, Clayton McGahee, an Emory archives specialist. Read more.
BPI scholar applications due June 6
The Office of Business Practice Improvement (BPI) is accepting applications, due June 6, for its next BPI Scholars class, which begins in September. BPI Scholars is a one-year professional development program designed to help early- and mid-career Emory staff members develop project management, communication, analytical, and leadership skills. Participants will apply these skills in a practice improvement opportunity identified within their home unit at Emory. More info.
Notable
Nancye Feistritzer was named VP of patient care services and chief nursing officer for Emory University Hospital, effective July 7. She previously served at Vanderbilt University Hospital. Read more.
Larry Young (Yerkes, psychiatry) was elected a member of the American Academy of Arts and Sciences.
Save the date
May 29: Position your research for commercial success: What to expect from the Office of Technology Transfer. HSRB auditorium, 4-5 p.m. More info.
Sept 27: Registration is now open for the Winship Win the Fight 5K. Event info.
