
 |
 |
 |
 |
| Members of the Ebola care team met with President Obama during his September 16 visit to the CDC. L to R: Charles Hill, Carolyn Hill, and Bruce Ribner |
When infectious disease physician Bruce Ribner got the call on July 30 from the US State Department requesting to transfer a patient with Ebola to Emory University Hospital's Serious Communicable Disease Unit, he and others had only 72 hours to plan for the patient's arrival. But the unit team had already been planning for this for the past 12 years, since the unit was first constructed.
"We conducted field exercises routinely, with a dedicated training day every year," says Ribner, who is medical director of the unit. "We knew what we had to do."
The first order of business was to mobilize and expand the team and "review, retrain, refresh" in standard operating procedures to ensure everyone's safety.
The team caring for the patient would include five infectious disease physicians, two pathologists, five medical technologists, and eventually 21 nurses, as the team expanded because of clinical demands. All were volunteers, with nursing staff coming from med-surg, emergency medicine, and critical care units at both EUH and EUH Midtown.
Unit and team coordinator Sonia Bell, a research specialist in infectious disease who has worked on the unit with Ribner since 2008, handled logistics, organizing training sessions, determining supply needs, and setting up nursing schedules.
Environmental Health and Safety personnel Patty Olinger and Kalpana Rengarajan provided biosafety support, including selection of personal protective equipment and training in how to don and doff Tyvek suits, how to use powered air purifying respirators (PAPRs), how to dispose of waste, and how to handle and transport samples. They also helped prepare the team psychologically, challenging them with spills and other incidents to give them practice remaining calm in the face of unexpected occurrences.
"We wanted to reassure ourselves that we could actually perform," says clinical nurse specialist Sharon Vanairsdale. "We wanted to see what it felt like starting an IV while wearing double gloves or wearing PAPRs for hours at a stretch. We wanted to make sure we could hear stethoscope sounds while wearing our head gear."
While the care team was preparing, dozens of others—in pharmacy, security, pastoral care, facilities, environmental services, and other departments throughout the hospital and university—also mobilized to support the effort.
EUH CEO Bob Bachman organized an operations team of key administrators and nursing and physician leadership that met twice a day. Reiterating the hospital's top priorities—the patients' welfare and the safety of staff and the community—was paramount. They sent daily emails to staff to share whatever information could be shared and joined with physicians on the care team to conduct regular town halls so staff could ask questions.
Robin Brown-Haithco, EUH's director of spiritual health, and the spiritual health team also provided support for hospital staff, and to the families of the Ebola patients. They made daily rounds on the unit, posted meditations and words of encouragement in the staff lounge and at the nurses station, and created a meditative slide presentation that ran throughout the day as a way to create calm and help staff and the patients' families remain centered. She also wrote an article on vocational call that was distributed to clinical areas throughout the hospital to help alleviate anxiety.
To help keep the public informed, physicians held a press conference the night before Kent Brantly was admitted to EUH on August 2 and thereafter remained available to respond as much as possible to the tsunami of interview requests from news media that ensued during and after the first two patients' stay.
"We had three basic messages to get across," says infectious disease physician Aneesh Mehta: "We have the expertise needed in serious infectious diseases. We are trained and prepared for these patients. And we will protect our patients, our staff, and our community."
It was up to the care team, the "we" to whom Mehta referred, to prove these statements true. They did so by adhering to their training and watching out for each other like hawks to make sure everyone else did too. They provided the best care possible and a lot of encouragement, companionship, and compassion to the patients, their families, and each other.
"I have never been involved with a team effort that was so family oriented," says Charles Hill, a pathologist who was struck by the historic significance of what was happening when the results of Kent Brantly's first blood test, processed through the unit's shoebox-size pathogen-detection device, came through: Ebola Zaire detected.
"As a pathologist, I interact with doctors all the time, but I don't usually get to work close to the patients and their families or with nurses. This was really special, and it changed my life. I got to see firsthand how amazing our nurses are."
His words about family were echoed by others.
"We had to function like a family," says Carolyn Hill, the unit's nursing director. "You depend on your family to keep you safe, and we depended on each other. We had family rules, and everyone on the team had an equal say in decision-making. There was no hierarchy."
"We had a family meeting for all team members every morning at 7:15," adds Vanairsdale, "and we agreed on decisions together, getting everyone's buy-in before making any changes."
While the nurses and doctors cared for the patients, remaining with them 24/7, Hill and Vanairsdale cared for the caregivers. "We were there to watch over them, to remind them of safety protocols, to take their lunch orders, debrief them during break, and diminish any 'noise' that could distract them," says Hill.
Hill is one of several team members who gave up their vacations to be on the team. "It is so inspirational and such an honor to be part of this," she says. "I would have given up all my vacations."
The hospital's first two Ebola patients were discharged the third week of August, and the third patient was admitted on Sept. 9.
Linking ICUs throughout Emory and beyond
 |
Heart rate 40, blood pressure 50, oxygen saturation 60. The post-operative patient was turning blue, and the ICU on-call physician was 15 minutes out. At a monitoring station miles away (like the one above), an eICU RN detected the deterioration and alerted the on-service eICU physician. He guided the critical care nurse practitioner at the patient's bedside through advanced resuscitation techniques via high-definition audiovisual tools as he watched vital signs, ordered medications, and reviewed lab data. The patient's condition stabilized.
 |
|
| Cheryl Hiddleston |
This is the mechanism of the recently initiated Emory Electronic ICU in action. Located in the Doctor's Center Building on the campus of Emory Saint Joseph's Hospital (ESJH), the Emory eICU is linked to ICUs at ESJH, Emory University Hospital (EUH), EUH Midtown, and East Georgia Regional Medical Center (and soon, at Emory Johns Creek Hospital).
Funded by a Health Care Innovations Award (HCIA) from the Centers for Medicare and Medicaid Services, Emory's eICU was initiated by Tim Buchman, Emory Critical Care Center (ECCC) director, as a way to expand access to critical care services, lower costs, and address the looming national shortage of critical care physicians.
Telemedicine provider Phillips Healthcare installed cameras, video monitors, microphones, and speakers in all of the participant ICUs as well as vital sign, patient monitoring, flowsheet, and lab interfaces and servers to handle data streams and storage. All hardware- and software-derived patient data from the participant ICUs routes to the eICU at ESJH and its 24-7 monitoring personnel. The eICU teams work closely with providers in the member ICUs in treating patients.
"This means all of our ICU nurses have a second pair of eyes watching their patients. When other physicians have gone home for the day, we have an ICU physician available at the push of a button," says critical care nurse Cheryl Hiddleson, operations director of the eICU.
The HCIA grant also provides support for two residencies in the ECCC. A one-year critical care residency is recruiting, training, and deploying NPs and PAs throughout the Emory system. A six-month HCIA residency provides critical care training for providers in other fields from hospitals in Georgia's underserved communities. When certified, the PAs and NPs return to their hospitals, which will improve access to community ICU health care across the state and eventually serve thousands of Medicare and Medicaid beneficiaries.
"The partnership's next phase will be adding the emergency departments at EUH and Midtown," Buchman says. "Patients requiring critical care will then be tracked as soon as they enter the Emory system, further widening the range and scope of the data needed to make informed decisions."—Sean Moore
DeLong receives Lasker Award for work in deep brain stimulation for Parkinson's
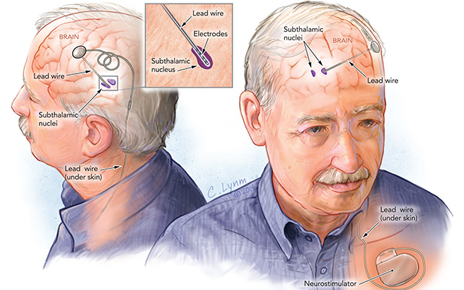 |
| In deep brain stimulation, electrodes implanted into a target site are connected to a neurostimulator implanted near the collarbone. Courtesy of Lasker Foundation. © Cassio Lynm. |
Mahlon DeLong, William Timmie Professor of Neurology, received the 2014 Lasker-DeBakey Clinical Medical Research Award along with Alim Louis Benabid of Université Joseph Fourier, Grenoble, France.
 |
|
| Mahlon Delong |
The two scientists are honored for their roles in developing deep brain stimulation of the subthalamic nucleus, a surgical technique that reduces tremor and restores motor function in patients with advanced Parkinson's disease. Their work has resulted in an effective treatment for more than 100,000 people worldwide.
Through more than 40 years of research, DeLong has played a leading role in discoveries about the functional organization of the basal ganglia, a group of connected brain structures deep in the cerebral hemispheres and their role in movement and movement disorders that have led to major breakthroughs in patient care for Parkinson's and other diseases.
When DeLong began his research, in the late 1960s, scientists knew that Parkinson's disease resulted from a loss of the neurotransmitter dopamine in the basal ganglia and that replacement therapy with levodopa, the precursor of dopamine, could eliminate the symptoms. No one, however, understood how this loss caused the symptoms associated with Parkinson's or the side effects of levodopa therapy.
Studying animal models of Parkinson's disease, DeLong and colleagues identified the neuronal circuitry and abnormal cellular activity in the basal ganglia that malfunction in Parkinson's disease. They found that specific regions in the basal ganglia involved in the control of movement, including the subthalamic nucleus, exhibited abnormal and excessive cellular activity. A key finding was that inactivation of the subthalamic nucleus abolished the slowness, tremor, and rigidity of Parkinson's in the animal models.
These findings provided a clearer understanding of the abnormalities in Parkinson's and a strong rationale for surgical therapy, thereby contributing to the revival and development of surgical treatments for this disorder. Most important, they provided a highly effective surgical target, the subthalamic nucleus, laying the groundwork for treatment of the disease by high-frequency deep brain stimulation, which was discovered by Lasker co-recipient Benabid. High-frequency deep brain stimulation acts to control abnormal firing of cells through delivery of electrical impulses, much like a cardiac pacemaker. Read more. Watch a video of DeLong discussing his research.
It's what we do
 |
|
| Wright Caughman |
I hope you have had a chance to see the ongoing national media coverage of Emory's leadership role in the global fight against the Ebola virus. By caring for three Ebola patients so far, we have helped to develop knowledge and protocols that are now being used to combat the virus in West Africa and other regions.
As the Ebola epidemic continues unabated and international health authorities urgently call for more fiscal and human resources in the hardest hit nations, it is rewarding to know that we at Emory have helped to save lives from the disease and to provide hope at a time when it is sorely needed. When the time came to do the right thing, our faculty and staff were amply prepared and selflessly driven to do so.
In a press conference upon his release from Emory University Hospital, Dr. Kent Brantly spoke eloquently about his miraculous recovery from the Ebola virus and about the extraordinary Emory team who helped to make that recovery possible. This inspirational outcome resulted from the efforts not only of the outstanding physician and nursing team you saw on camera, but also from all the talented and dedicated staff and faculty, from international leaders in infectious diseases to hospital support personnel, who provided the knowledge and expertise to educate and design the best treatment, and who worked behind the scenes over the course of several weeks to care for Dr. Brantly and his fellow patients.
Caring for such seriously ill patients requires an impeccably trained, well synchronized, and deeply compassionate team of professionals. Fortunately for our Ebola patients, our Emory team is just that. Let us not forget that, even when there is no spotlight, we care for patients every day whose illnesses are less newsworthy but every bit as serious to those patients and their families. Every day, the most critically ill patients in the region turn to us for help, and every day we give them the world-class care they need to regain their health. It's what we do. It's who we are.
Thanks to everyone who has cared for and continues to care for our patients with the Ebola virus and to everyone who provides the same stellar level of care to all of our patients every day.
Please direct questions and comments to evphafeedback@emory.edu.
 |
In case you missed it on Facebook...
 |
Neurosurgeon Nick Boulis and neurologist Jonathan Glass took the ice bucket challenge on Aug. 20 to raise money to fight ALS.
Houry named director of CDC center
 |
Debra Houry has been named director of the CDC's National Center for Injury Prevention and Control, effective Oct. 6. She currently holds joint appointments in the schools of medicine (emergency medicine) and public health (behavioral sciences and health education). She will lead a staff of more than 250 in national efforts to prevent prescription drug overdose, motor vehicle-related injuries, traumatic brain injuries, and violence against children and youth. Read more.
HRSA training grant for NPs and midwives
 |
|
| Carolyn Clevenger directs the grant program. |
The nursing school received a $700,000 award from the Health Resources and Services Administration to train nursing students to become primary care nurse practitioners and/or nurse midwives. The school will award 35 students with $10,000 scholarships over the next two years. Read more.
ESJH expands med-surg and oncology units
 |
Emory Saint Joseph's Hospital hosted an open house last month for two expanded units: The newly refurbished 7 East unit houses all of the hospital's oncology patients, and 7 West is the new home of ESJH's medical-surgical unit. Each unit has the ability to care for 18 patients. Read more.
Emory offers free, secure cloud storage
Emory is providing faculty, staff and students a secure version of Box. Emory Box is available at http://emory.box.com. (Log into the service and use your Emory ID and password to create an account.) According to Rich Mendola, enterprise CIO and senior vice provost for library services and digital scholarship, Emory Box meets all the requirements for storing protected health information to allow clinicians and other investigators to easily and securely share information. Read more.
Notable
 |
| Griendling and Alexander |
Kathy Griendling was recently appointed to the R. Wayne Alexander Professorship in Cardiology. Read about her research.
 |
Jasmine Hoffman (nursing communications) recently received the Shining Star Award from the Georgia Chapter of the Public Relations Society of America.
Leonard Howell (neuroscience research) has been appointed associate director for scientific programs at Yerkes. Read more.
 |
Marilyn Margolis is interim CEO at Emory Johns Creek Hospital, where she is currently also CNO and VP of operations.
Craig McCoy has been named CEO of Emory Saint Joseph's Hospital after serving as interim CEO since May.
Ken Newell (Emory Transplant Center) is president of the American Society of Transplantation. Read more.
 |
Raymond Schinazi (pediatrics) received the 2014 Research & Hope Award for excellence in research from the Pharmaceutical Research and Manufacturers of America.
 |
Susan Shapiro has been appointed associate dean in nursing for community and clinical partnerships, a role in which she will oversee development of strategic collaborations with other institutions and develop continuing education and non-degree certificate programs to strengthen's the nursing school's offerings to working professionals.
 |
Suzanne Staebler was recently named a fellow of the American Association of Nurse Practitioners.
Events
Sept 27: Winship Win the Fight 5K. More info.
Oct. 2-3: HIV & Aging: From Mitochondria to the Metropolis. Decatur Marriott, Atlanta. More info.
 |
Oct 17: Winship researcher Adam Marcus will be a presenter at TEDx Peachtree. More info.
Oct 23: State-of-the-Nursing-School. Address by Dean LInda McCauley, 4:30 p.m., SON auditorium, RSVP.
Oct. 29: Emory Medicine 2015. Address by Dean Christian Larsen, 4:30, WHSCAB Auditorium. Reception to follow.
Oct 31: 2014 EHC Quality Conference. 8-noon, Cox Hall. Deadline for poster submission has been extended to Sept 26. More info.
