WHSC finance 101: Case study in connectivity
Part of a series explaining how funds flow throughout health sciences
A birds-eye view of how units are funded in the health sciences ecosystem makes one thing readily apparent—the extent to which financial health in one unit or mission is interwoven with that of others. Fluctuations in revenue and expenses in one area have ripple effects downstream that in turn can exert their own eventual effects back up-river.
| |
 |
| |
Ronnie Jowers |
Keeping all three missions (research, patient care, teaching) in these units healthy and growing strategically requires a "delicate financial balancing act," says WHSC CFO Ronnie Jowers.
Take the research mission, for example. Over the past three decades, Emory has invested heavily in research, adding space and talent and raising its national rank in NIH awards from essentially off the radar to 16 in the medical school and 18 university-wide, with the vast majority of the latter coming to WHSC, and not just to medicine but also to nursing, public health, and Yerkes.
"This investment catapulted research but also benefited our standing in teaching and patient care at the same time," says Jowers.
During this same period though, patient care facilities have continued to age, some more gracefully than others. "We need to reduce the average age of our plant facilities, which is an issue that the new proposed 210-bed hospital tower will help address," says Jowers.
Keeping clinical facilities up to date and staying healthy in patient care are important not only for their own sake but for that of research and teaching too.
Another, more specific example of the interwoven nature of missions and funding is the medical school's Academic Enrichment Fund (AEF).
The AEF, which comes directly from net patient service revenue in Emory Healthcare, currently accounts for about 17% of the medical school's university budget. It has been around since the 1950s, when, thanks to Robert Woodruff, The Emory Clinic was created for the specific purpose of shoring up medical school finances. At that time, the school had virtually no income other than tuition, was trying to hire more paid faculty (as opposed to relying exclusively on volunteers for teaching), and was drowning each year in red ink.
"Every academic health center in the country has some version of the AEF," says Jowers. "That's how academic medicine gets funded in part."
When AEF dollars come to the medical school, the medical dean in turn uses them to help support the school's 28 departments—their operational and recruitment needs, including recruitment of clinical and basic science chairs. By far the largest and most numerous of the school's departments (20) are clinical.
"AEF dollars may go to the school, but they are used to attract and keep the very people who help create and sustain our reputation and capabilities in patient care," says Jowers. "Without the AEF, the school's teaching and research would suffer, but so in turn would the whole clinical mission."
New Yerkes research building
 |
| The building was designed by Lord, Aeck, and Sargent. |
| |
 |
| |
Stuart Zola |
Yerkes National Primate Research Center is making way for a new $15 million research building.
The nearly 20,000-square-foot building will house researchers focusing on immune system function and transplant medicine, says Stuart Zola, the center's director.
Construction on the three-story facility is expected to begin this summer and will take about 18 months. The facility is being built with NIH stimulus funds, and the expansion is expected to create up to 20 new jobs, including researchers and animal care technicians.
Training for danger in a safe place
 |
| Sean Kaufman leads a BSL 4 training course. |
One in a series of profiles of people in the Woodruff Health Sciences Center
When Sean Kaufman joined the faculty in Rollins School of Public Health in 2004, he came from the CDC, where he had helped respond to outbreaks of anthrax, SARS, and West Nile virus. But he experienced a pang of fear when Ruth Berkelman, director of RSPH’s Center for Public Health Preparedness and Research, told him the center had received an NIH grant to create a training program for biosafety level (BSL) 3 and 4 labs. She wanted Kaufman to design and implement the curriculum.
| |
 |
| |
Sean Kaufman |
But Kaufman specialized in health and human behavior, and despite his extensive CDC experience he had never even been inside a BSL lab.
Such labs are numbered according to risk: BSL 3 labs focus on lethal inhalable infectious agents for which treatments exist. Workers in BSL 4 labs must wear positive-pressure suits with oxygen hoses connected to them to protect against organisms, such as Ebola and other viruses causing hemorrhagic fever, for which there is no effective treatment.
In the seven years since its inception, the Emory program Kaufman designed in collaboration with CDC and NIH has trained more than 2,000 people from across the world, including scientists and lab technicians, police, firefighters, and other emergency responders. Numerous BSL training programs have sprung up based on the Emory model, which started the trend and remains the gold standard.
Biostats
• Current: Director of Programs, Center for Public Health Preparedness and Research, RSPH
• Faculty, Univ of Phoenix, Atlanta
• Health education and communication specialist, CDC Office of Terrorism Preparedness and Emergency Response
• Health education specialist, San Diego State Univ
• BS and MPH (health promotion and education), SDSU
|
|
BSL training has much in common with flight simulation that exposes pilots on the ground to dangers they will face in the sky. BSL training takes place either in the mock lab on the Emory campus or in real labs worldwide before they "go hot" (become active). Trainees experience problems like spills with all the adrenaline rush and urgency of real-life situations—but without the risk of serious illness or death. The weeklong training also is designed to "provoke" errors.
"You can learn about BSL emergencies from textbooks the same way you theoretically can learn to swim from a PowerPoint presentation, but the only real way to learn how to respond to BSL emergencies is by responding," says Kaufman. "Our program bridges the gap between knowing something in your head and being able to respond quickly, appropriately, and with minimal risk."
In a typical day, Kaufman trains participants, polishes the curriculum, or gives talks about BSL training. The hardest part of his job is being away from home and his two sons for sometimes up to a month. During the past six months, he has provided training in soon-to-be-active BSL labs in Jordan, Switzerland, India, Mexico, and Honduras, as well as at the University of Florida, George Mason University, and UCLA.
The best part of his job, says Kaufman, is "seeing the light bulb go on when participants learn to do something they previously thought impossible."
New sim unit at EUHM
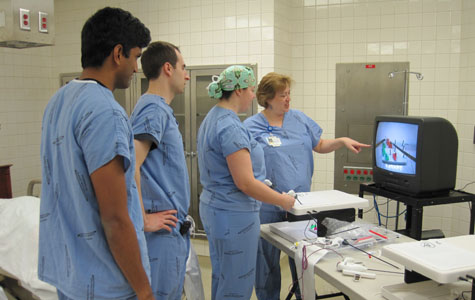 |
| Jessica Arluck teaches laparoscopic surgery techniques to resident Catherine Hudson and medical students Christopher Corso and Sri Balusu in the simulation lab. |
A new pilot simulation lab at Emory University Hospital Midtown (EUHM) is providing medical and nursing students, residents, and staff with hands-on training to perfect and maintain their skills. Located in former ob-gyn operating rooms, the lab focuses on team building, clinical competencies, and research.
The first sim lab of its kind at EUHM, it is a joint venture between the medical school and Emory Healthcare (EHC).
One side of the lab is set up to train gyn-ob residents and students in deliveries and laparoscopic surgeries, cardiac arrests, mock codes, and high-risk procedures.
| |
 |
| |
Sharlene Toney |
| |
|
| |
 |
| |
Douglas Ander |
The other side is used for training nurses in central-line and intravenous insertion and medication dispensing. It also is used for competency validation for new nursing employees and annual skills assessment of current nursing staff, according to Sharlene Toney, executive director of professional nursing practice in EHC.
Jessica Arluck, assistant professor in gyn-ob, uses the lab to teach residents the basics of laparoscopic surgery on a training module and monitor. She also teaches students with the help of an adult-size mannequin named Noelle that simulates giving birth and going into cardiac arrest.
The lab is a "proof of concept" center, with the small setup being only the first step in the process, says Douglas Ander, director of the Emory Center for Experiential Learning and an associate professor of emergency medicine. In the future, plans include adding cardiac catheterization simulator capabilities, as well as space for a simulated emergency department and nursing station.
Bittersweet journey
 |
Team Blissfully Unaware: Paige Martin, Lisa Tillman, and Nancy Sestak, all in health sciences development and alumni relations |
First person, by Paige Martin: In December, after a glass of wine or two at an event, I registered for a 200-mile bike ride to benefit AIDS vaccine research. I thought this would be a good way to get into shape by my 40th birthday, and the money raised would go to a great cause. The AV200 has raised $1 million for AIDS vaccine research at the Emory Vaccine Center (EVC).
So from January to May, I spent almost every Saturday and Sunday on training rides with my teammates, two other development colleagues I knew peripherally when we started out. We learned a lot about each other on our 75-mile rides. I now consider them dear friends. Without a team, I would never have been so faithful in my training.
We chose the team name "Blissfully Unaware" because we didn't know what we were doing. When I started training, I rode a sub-par bike and couldn't identify a spoke or a front or rear derailleur. I upgraded to a bike that is worth more than my car but still can't identify a spoke or a front or rear derailleur.
I also was blissfully unaware when I started this adventure that we would hit Zaxby's after every training ride, thwarting my plans to become a waif by my birthday. And I was unaware of how a life event would make this bike ride so very special to me.
| |
 |
| |
Ron Martin |
My father had a stroke on April 14 and passed away two days later. In his memory, my teammates dedicated our ride on May 14-15 to him. My teammates had been entertained by (subjected to?) countless Ron Martin stories over the course of our training, and the dedication was a fitting tribute, as Dad bought me my first bike in 1978, shortly after my family moved to Cullman, Ala. I had lamented that without a bike, I would not make any new friends ("I will never make it in this town!"). Dad gave me a bike that was quite fashionable for 1978, light green with swirling yellow flowers, and I happily rode it around the neighborhood for years. In Alabama, everything closed on Sundays, and Dad would ride with me and my siblings. With a grown-up, we got to go faster and farther, into a nearby shopping center where the parking lot was vacant and inviting. There is a sense of joy and youth and strength that I will always associate with biking. And with my dad.
When May 14 arrived, rain was forecast, and I was more than a little nervous about braking on slick, wet roads. In our five months of training, remarkably we never had to ride in the rain, but the day went well, and we biked through the scenic Georgia countryside to arrive at Camp Rock Eagle in the Oconee National Forest, where we would spend the night before heading back the next day.
Due to injuries and fatigue, the rest of Team Bliss opted for the shorter 88-mile route on Sunday, so I was alone on my 106-mile journey (they don't tell you until you start that the ride is actually 106 miles out and 106 miles back).
My biggest fear was that I would be "swept up" by the rescue vans. Knowing that I needed to bike the full day, I hurried through breakfast and was the first to leave camp. I was on my own for the first 30 or so miles, and then these "youngsters" (ages 24, 25, and 30) adopted me into their group, and I was able to keep pace with them.
I finished the race, biking 200+ miles in all, and
I didn't get swept up!
I know I would not have finished the full ride had I not been part of a team. I would have missed out on all of the riders biking from Decatur Square to Emory with police escort. I would have missed out on the celebration and learning from Dr. Rafi Ahmed, director of the EVC, and Dr. Mark Mulligan, director of the Hope Clinic, about what is made possible at the EVC and clinic by AV200 dollars. I am grateful for my training team and my riding team—and what they made possible for me. |
|
 |
|
From the Executive VP
 |
| Wright Caughman |
|
Facilities Update
A few weeks ago, we had the privilege of announcing an exciting opportunity—the plan to build a new bed tower on Clifton Road and to make capital improvements to our existing health care facilities. I'm thrilled to know that many of our medical professionals and the patients they serve will soon have the state-of-the-art facilities they deserve.
If you or someone you love has ever been a patient in the oldest sections of Emory University Hospital (EUH)—those that date back to 1922—or has ever visited our Emergency Department on a Friday night, then you know why our trustees recently approved the construction of a new bed tower on Clifton Road as well as updates to the existing EUH. While our old building has served us well for nearly 90 years and will continue to serve us for several more, increased patient volumes and the challenges of modern medicine necessitate a new facility. And of course in the meantime, we also will address needed improvements to our current facility in order to most effectively serve our patients and our community.
I've been an Emory physician for more than 20 years, and I've never ceased to be amazed by the transformative care our medical teams provide in spite of aging facilities. Imagine then what this group of medical professionals will be empowered to accomplish in state-of-the-art new and upgraded facilities. Imagine the increased comfort and ease of access for our patients.
Of course, we recognize that our current plan won't overcome all of the facilities challenges we face across our campuses, but it represents a positive first step toward a better environment for our faculty and staff and, most important, a better experience for our patients and their families.
That's not to say the process will be easy. Change never is. Construction is bound to cause inconveniences now and again, and we'll probably experience some growing pains along the way. But as we do, I'll ask you to remember what we're getting in return … to think about the people in need and their families who will be the ultimate beneficiaries. I know we will all find the trade-off well worth it.
We're still in the very earliest stages of beginning to plan, but I'm committed to keeping you up-to-date as decisions are made and work begins. Thanks to all who have written and called to express your enthusiasm for this exciting opportunity for Emory and for our community. Expect to hear from me regularly with updates on our planning and progress, and I hope to hear from you too. (evphafeedback@emory.edu)
In brief
Emory's doctors are among the best in Atlanta, but you already knew that.
Special congrats to all the doctors who made the 2011 Atlanta magazine Top Doctors list. More than 100 of the 318 physicians who were recognized this year practice at one of Emory's facilities. (See the list.) Special thanks also to Emory patients and their families for putting their trust in us every day.
Long-awaited FDA approval for Emory-developed drug
Surgeon-scientists Chris Larsen and Tom Pearson learned last month that the drug Nulojix (belatacept) had received FDA approval for prevention of graft rejection after kidney transplants.
They played a leading role in driving its development, in collaboration with other researchers at Emory, including at Yerkes, and at Bristol-Myers Squibb.
Belatacept could be a less toxic alternative to calcineurin inhibitors, the drugs most transplant patients now rely on to inhibit their immune systems but which can damage the kidneys and lead to high blood pressure and diabetes.
This is the first time a new class of drugs has been developed for transplant since the 1990s. Belatacept has the potential to improve and simplify the medication regimens of kidney transplant recipients and is also now being tested in experimental clinical trials for liver transplant and pancreatic islet transplant. Read more.
New guidelines for volunteer activities
The Office of Quality and Risk, which oversees Emory's professional and general liability insurance, recently implemented new guidelines for Emory employees and students who volunteer their time to outside nonprofit organizations. If you wish to participate in such volunteer activities as a representative of Emory and be covered by Emory's professional and general liability insurance, the guidelines require that this be approved beforehand. For more information, please access university policies or Emory Healthcare policies.
Questions? Please call the Office of Quality and Risk at 404.778.7932.
Notable
 |
|
| Christine Dunham |
|
Christine Dunham (biochemistry, medical school) has been selected as one of 22 Pew Scholars in the United States. The Pew biomedical sciences program awards financial grants to encourage early career scientists to advance promising research. Read more.
 |
|
| Nancy Collop |
|
Nancy Collop, director of the Emory Sleep Center, has been named president of the American Academy of Sleep Medicine.
 |
|
| Jenny Foster |
|
Jenny Foster (nursing school) was elected as a fellow of the American College of Nurse-Midwives. Foster recently led an NIH-funded study to reduce maternal health disparities in the Dominican Republic.
 |
|
| Marcia Holstad |
|
| |
|
 |
|
| William Puentes |
|
Marcia Holstad and William Puentes (nursing school) will be inducted as fellows into the American Academy of Nursing (AAN) at its annual meeting in October. With their induction, Emory will have 12 nurses who are AAN fellows.
 |
|
| Debra Houry |
|
Debra Houry (emergency medicine) was inducted as president of the 6,500-member Society for Academic Emergency Medicine at SAEM's annual meeting in June. At that same meeting, Kate Heilpern, chair of emergency medicine, was honored with the SAEM's award for Advancement of Women in Academic Emergency Medicine. Read more.
 |
|
| Spero Karas |
|
Sports medicine specialist Spero Karas has been named head team physician for the NFL's Atlanta Falcons. He will be the team's orthopaedic surgeon and oversee medical care for the Falcons' athletes and coaches. Karas is also orthopaedic surgeon for Georgia Tech baseball and consulting team physician for Georgia Tech, Emory, Oglethorpe, and Perimeter athletics.
 |
|
| Tom Lawley and Ursula Kelly |
|
Congrats to Thomas Lawley (medical dean) and Ursula Kelly (nursing faculty), who each received a Healthcare Hero Award from the Atlanta Business Chronicle. Lawley won the physician category for his role in guiding Emory to a top research ranking among U.S. medical schools. Kelly won in the Allied Health Category for her work at the Atlanta VA Medical Center with female veterans suffering from post-traumatic stress disorder and sexual trauma. Other Emory faculty, including Linda Cendales, Kate Heilpern, and Curtis Lewis, also were honored.
 |
|
| Mark Rapaport |
|
Mark Rapaport will join Emory in September as chair of the Department of Psychiatry and Behavioral Sciences. He currently is vice chair and professor of psychiatry at UCLA. Read more.
 |
|
| Jeremy Sarnat |
|
Jeremy Sarnat (environmental health, public health) has been awarded the 2011 Joan M. Daisey Outstanding Young Scientist Award by the International Society of Exposure Science (ISES). The award, one of four the ISES gives each year, recognizes outstanding contributions to human exposure analysis by a young scientist.
Events
Oct. 15: Winship 5K Win the Fight Walk/Run to support cancer research and care. McDonough Field, Emory campus. Register online.
Oct. 15, 16: Juvenile Diabetes Research Foundation Walk to Cure Diabetes. Two local events, one at Centennial Olympic Park (Oct. 15) and one at State Farm Park in Johns Creek (Oct. 16). Contact Tara Davis, tdavis2@emory.edu, or register online. |