Growing up and older with cystic fibrosis
by Quinn Eastman
When Michael Schechter was a resident in training in the 1970s, he had only one cystic fibrosis patient who made it to 20.
"At the time, that was considered remarkable," says Schechter, who today directs Emory's Cystic Fibrosis Center.
Now the average life span of people with cystic fibrosis (CF) is edging toward 40. Emory's center, for example, is treating patients like David Adkins, 53, who started jogging as a form of respiratory therapy and eventually completed four marathons.
"Eventually children have to take responsibility for their own schedules and their own medications," says Lindy Wolfenden, director of the Adult CF program. "This sometimes is an adjustment for both parents and children. It's not that long ago that parents were told not to expect their child to live past the age of 18."
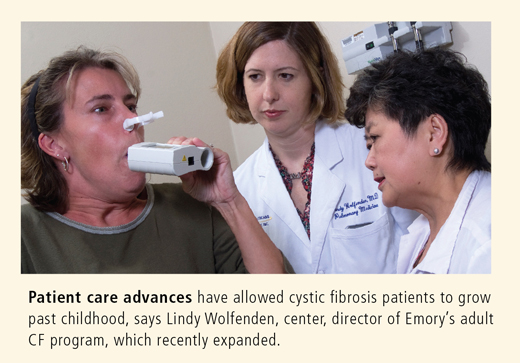
Gradual advances in patient care have transformed CF from a condition that cut short the lives of children to one in which adults are planning for their futures. Recently Emory's adult program has expanded so dramatically that it has moved to a new location in the Emory Clinic.
|
|
Because of mutations in a gene that disable the cells' ability to transport salt, people with CF produce unusually thick, sticky mucus. The mucus clogs their airways and often leads to life-threatening lung infections. It also obstructs the pancreas, preventing digestive enzymes from breaking down and absorbing food.
CF causes a gradual loss of lung function, exacerbated by infections and bronchial obstruction, says Wolfenden. Advances in treatment over the past few decades include refinements in airway clearance techniques and infection control as well as improved inhalable antibiotics and medications that thin mucus.
The Emory CF center also is bolstering research to support clinical care in areas such as CF-related diabetes and vitamin D deficiency. Pulmonologist Arlene Stecenko is looking at how diabetes develops in CF patients and the mechanism by which diabetes aggravates lung disease. In another area, membrane physiologist Nael McCarty is bolstering basic research on proteins that mutate in CF. Schechter is looking at the impact of patient and parental anxiety and depression on the course of disease. And the center's clinical researchers are gearing up to participate in large-scale, multicenter studies of medications that may enhance the functioning of mutant proteins.
At Emory, CF patients typically visit their doctors at least every three months for a checkup and test of lung function. They use a variety of methods to clear mucus from their lungs, such as vibrating vests, inhalation of several nebulized medications, and regimens of breathing exercises and coughing. They often have diets whose caloric intake rivals that of Olympic swimmer Michael Phelps, and they take enzyme supplements with each meal to aid digestion.
Adults with CF have concerns ranging from having families to managing CF-related diabetes, which becomes more common as patients age. One-third of adults with CF between 20 and 29 and close to half of those over 30 develop diabetes.
Emory's CF center is one of the five largest in the country and cares for approximately 600 people through its adult program and an affiliated program at Children's Healthcare of Atlanta, Schechter says. To tailor care to the growing adult population of close to 200, Emory has brought in several specialists, including an endocrinologist, a social worker, a dietician, nurses, and nurse practitioners.
One of the adult patients, Craig Pubanz, 35, is happy to share advice with young people with CF: "If you take care of yourself, you can go to college, have a family, and live life to its fullest."



