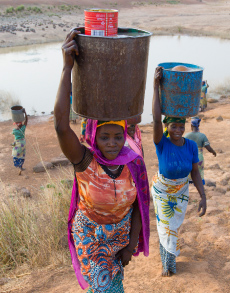A president's promise
by Rhonda Mullen
President Carter made a vow to wipe an ancient and terrible disease from the face of the earth, and two decades later, he’s on the verge of making it happen.
Jimmy Carter has told the story many times, but it is worth retelling. He and former First Lady Rosalynn Carter had made the long trip from Georgia to a remote village about 50 miles from the capital of Ghana. They had come to Denchira to see first-hand an ancient and unsavory disease called Guinea worm that was wreaking havoc in Africa.
As they arrived, all the villagers who were able gathered under a patch of shade trees to hear what this former President of the United States had to say. Carter began to talk about the causes of Guinea worm, a tropical disease that here in Denchira on this day affected more than 200 of the 500 villagers listening to him.
Among them was a woman, cradling a baby in her arms. Carter approached her to ask the baby’s name and to talk with her, but when he got closer, he realized there was no baby. Instead the woman was holding her right breast, swollen to an arm’s length, with a Guinea worm painfully emerging from the nipple. Later that same year, the woman would have 11 other Guinea worms break the skin and begin their painful exit from her body.
Then and there Carter made a promise to himself that this horrific disease had to be stopped. He thought, there is no reason that people should go through such suffering from a disease that is so easy to prevent.
Referred to as the “fiery serpent” in the Bible, Guinea worm has been with us always. People contract Guinea worm, or dracunculiasis, when they drink contaminated water containing tiny water fleas (copepods) that harbor Guinea worm larvae. The worms mature in a person’s body, growing up to 3 feet in length, and after a one-year incubation, they emerge through burning blisters in the skin. The worms must be removed manually from the body as they emerge—they are wound around a stick a little each day over the course of one to two months. Often infected people go into water holes for relief from the pain, releasing larvae into the water and starting the cycle all over again.
|
|
The Carter Center—founded in 1982 in partnership with Emory University—seeks to improve the quality of life for people worldwide, advance human rights, and alleviate unnecessary suffering. Its health programs look to fill vacuums in global health, areas where no other group is working effectively, and that is where Guinea worm comes in. When the Carters started to identify those vacuums, the biggest gap they discovered in the past 30 years was in the prevention and treatment of neglected tropical diseases. “We adopted them because no one else wanted to fool with them,” says Carter.
The Carters have marshaled a worldwide network of global health organizations, tropical disease experts, and volunteers to tackle not only Guinea worm but also a raft of neglected tropical diseases. The CDC has been integrally involved, as have the WHO and the Peace Corps. UNICEF has drilled deep wells, bringing safe water to some villages affected by Guinea worm. Emory’s Rollins School of Public Health has trained key leaders in the Guinea worm program. Most important, villagers in Asia and Africa have served on the front lines of the Guinea worm showdown. Today, all the leaders of the national eradication programs come from in-country, as do many of the staff on the support teams.
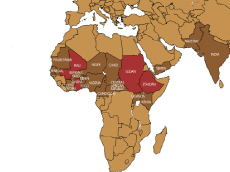
When the center undertook the first worldwide eradication campaign of Guinea worm in 1986, there were an estimated 3.5 million cases in 20 countries in more than 23,000 villages in Asia and Africa. With the doors that the President opened and the interest and energy he generated, cases of Guinea worm began dropping precipitously. One after another, the Guinea worm count fell to zero in Pakistan (1993), Kenya (1994), India and Chad (1996), and on to Yemen, Senegal, and Cameroon. Today Guinea worm cases have been reduced by more than 99.9%, and the worm remains in only four countries in Africa: Sudan, Ghana, Mali, and Ethiopia. In fact, Ghana may have already seen its last case, but because of the one-year incubation period, that can’t yet be confirmed.
What is known: there are now fewer than 600 uncontained cases of Guinea worm in the world, with the largest chunk of those in Southern Sudan. The challenges there include reaching isolated villages in war-torn areas that are spread over vast distances. The Carter Center has more than 12,000 volunteers in Sudan alone, but safety remains an issue. “In a troubled zone, it is triply difficult to get those last cases,” Carter says.
Still he is not discouraged. Despite setbacks and occasional faltering in the program over the past 20-plus years, its steady progress has kept Carter inspired and going. Guinea worm eradication is now within reach, and when—not if—that happens, it will become only the second disease ever to be eradicated and the first to be eradicated without vaccines or medicine.
One village at a time
Jimmy Carter—former President, Nobel Peace Prize laureate, Emory University Distinguished Professor—is at his core a farmer. With two family farms in Georgia, one dating from 1904, the other from 1833, Carter has roots that are deeply embedded in the soil around Plains, population 635.
When he started visiting the farming communities in Africa that were brought to a standstill by Guinea worm, he felt right at home. Carter knew what it means to a community when its farmers are unable to work, when the children are too sick to go to school, when the mothers are too weak to cook the evening meal. The son of a nurse, he knew that health is vital to peace and potential.
And it’s not just the people infected with Guinea worm who have Carter’s empathy. The threat of river blindness (onchocerciasis) in Africa has caused farmers to move further and further away from the rich fertile bottomland near the river to get away from the black flies that breed in rapidly flowing waters and cause the eye-damaging, even blinding disease. In coffee-producing countries such as Guatemala, contracting river blindness may be considered an occupational hazard. Fast-flowing streams providing irrigation to nearby coffee farms can be breeding grounds for the black flies that spread the disease.
|
|
In endemic areas, people are bitten thousands of times each year, and a small child may be bitten more than 50 times in a single day. The result is that almost everyone in an endemic community can harbor onchocerciasis, which prevents them from working, harvesting crops, receiving an education, or taking care of children.
Following the model developed for the Guinea worm program, the Carter Center has taken on other tropical diseases that are little known in the developed world: river blindness, trachoma, lymphatic filariasis (elephantiasis), snail fever (schistosomiasis), and malaria.
The center’s approach is what Donald Hopkins, vice president of the health programs at the Carter Center and former deputy and acting director of the CDC, calls “old-fashioned public health.” The Carter Center’s expertise, he says, is in providing supplies, mustering experts and volunteers, and managing data, as opposed to laboratory research or digging wells. Carter Center workers stick to what they know. While the intervention tools may vary in the specific disease programs, all involve a village-based, low-cost approach.
Take, for example, the pipe filters that protect people from Guinea worm when they have to drink from unsafe water sources. Over the two decades of the eradication program, Carter Center staff have learned that nylon filters work faster and last longer than cotton, and a finely woven metal mesh screen lasts even longer. When war prevented Carter Center workers from reaching the people of Sudan with their education interventions for Guinea worm, they still were able to send ahead more than 9 million pipe filters to the inaccessible regions. The filters were assembled by refugees living in Kenya (many of them women) and donated by private, government, and church partners in Norway. By the time workers were able to safely navigate the countryside, the filtering technique had already dramatically reduced the number of cases there.
“When we enter a new country or village, we start with respect,” says Hopkins. “We don’t go into a village with the attitude that we have all the answers. We have to remember it’s not our country. We serve at their pleasure.”
Some in the global health community have criticized the center’s decision to focus on individual diseases rather than broad primary health care initiatives. After all, while horrific, Guinea worm is not fatal. Hopkins—and Carter too—take issue with that. “There’s a lot of verbiage on how countries need to develop and strengthen their primary health care,” Hopkins says. “When a child needs an immunization, breaks a leg, or gets bitten by a snake, those are all basic health care needs. But there’s an awful lot of talk and precious little action. We don’t do good waiting for perfect.”
As for Hopkins, he says he’d “rather get something than nothing.” Working on single diseases, he argues, can lead to so much more—through health education, improvement in general hygiene, and advocacy for safe water programs. Where appropriate, the Carter Center also combines interventions, such as mass drug administration against several diseases.
The Carter Center’s river blindness program, for example, distributes the medicine Mectizan (donated by Merck) to kill the parasite’s larvae, preventing blindness and transmission, and as a fringe benefit, de-worming children. Other benefits include mobilizing villages to create better health systems and improved nutritional status.
In general, Hopkins believes that the developed world has fallen well short of its potential in answering health challenges in developing nations. “We can and should be doing more,” he says.
The realm of possibility
With the help of Hopkins and a cast of tens of thousands, Carter has been after Guinea worm for more than two decades. He’s been assisted by kings, presidents, and prime ministers as well as those who have inspired him but remain nameless. On a return trip to Denchira, he was unable to locate the woman who first motivated him to take on Guinea worm. She was no longer living in the village. But he was gratified to see that, thanks to efforts by the Carter Center and the donation of a banker who paid to have a well drilled in the village, the number of cases of Guinea worm in Denchira one year later was zero.
Those many years ago, Carter never thought it would take this long to bring the cases to zero elsewhere, but he is determined to finish the job. “We are tenacious,” he says with a smile.
Failure is not a possibility for more reasons than one. He has made promises to people who’ve done their part. If he doesn’t succeed with Guinea worm now after all this effort, how can he ever hope to succeed with a more complicated disease like malaria?
Carter also knows that just one uncontained case of Guinea worm can unleash the scourge all over again. “If you have one case left in one village in a country, that one person with a Guinea worm emerging from her leg can walk into a waterhole and the Guinea worm lays hundreds of thousands of eggs, and you’ll have all the village next to you contaminated,” he says.
As Hopkins told the Chicago Tribune, “I’m not going to be satisfied until that last worm is gone. And it’s partly out of fear. Because I know that if this program were to fall apart, Guinea worm could come back.”
At 86, Carter is 17 years Hopkins’ senior. Yet he keeps a more ferocious pace, says Hopkins. “He is inspiring and demanding. He is someone who pays attention to details but who has great empathy with people.”
So with the energy of a much younger man, the tenacity of a world leader, and the patience of a farmer, Carter is fighting to keep his promises to rid the world of the fiery serpent. “My prayer is that I’ll be able to see the last person that has Guinea worm,” he says. “I don’t have a doubt, God willing, that I’ll be able to see that achievement.” EH
When The Carter Center started its Guinea worm eradication effort in 1986, the disease affected 3.5 million people in more than 20 countries and 23,000 communities in Africa and Asia. More than two decades later, with help from worldwide partners, the disease remains in only four countries, with the majority of cases (under 20,000) in war-torn southern Sudan. |
|||