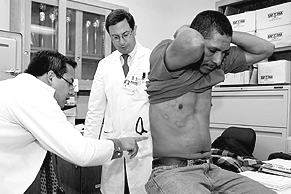
La mano de obra: The hand of the worker
Juan Perez doesn't look so bad for someone with leprosy. He's fit—lean and muscular for his 47 years, and he has a kind smile. His skin is leathered from a life spent working in the fields under the relentless Mexican sun of his hometown, Pińotepa, Oaxaca. Perez joined his father and brothers there when he was 10, harvesting or planting corn, tomatoes—whatever was in season—cleaning fields in the off season. Most of his life, he worked from dawn to dusk for about 15 pesos a day—the equivalent of $1.50, on a diet consisting of salted tortillas and frijoles. Somewhere along the way he was exposed to the bacterium that causes leprosy, and with an immune system ravaged by malnutrition, Perez was fertile ground.
Carlos Franco Paredes, chief resident at Grady, took a special interest in Perez. He views his leprosy—one of just 200 cases in the United States—as the result of a complex chain of events and situations. He doesn't hold a bacterium solely responsible. He blames a life of harsh, grinding poverty. "Many of the patients I see have HIV/AIDS or tuberculosis," says Franco, an MPH student and fellow in the AIDS International Research and Training Program at RSPH. "Treating patients with TB or HIV involves more than just making sure they take their medication. There's an entire world behind these patients, and for most it's a world of poverty and social inequalities. Social factors predispose people to these diseases. You see TB among poor people. You see it at Grady. You don't see it at Emory Hospital. It's like so many public health problems: You are much more likely to suffer disease if you're poor, malnourished, or living in overcrowded, unsanitary conditions." Rough estimates place the number of Mexicans working in the United States at about 2.7 million—54% of all illegal immigrants. Like Juan Perez, they are unlikely to receive medical care—either treatment or prevention—until they are desperately ill or worse. The Browning of America Extreme poverty in Mexico and other Central American countries drives a continual stream of immigrants across the border into the United States. During the past five to 10 years, the immigrant stream has turned toward Georgia, the Carolinas, and other southeastern states. Hispanic immigrants, both legal and illegal, flocked to Atlanta during the construction boom before the 1996 Olympics. They keep the carpet factories running in Dalton, Georgia. They harvest Vidalia onions in south Georgia, and they eviscerate chickens in Gainesville plants. They take jobs Americans have no use for during economic boom times. They fill an economic void, and they're changing the face of Atlanta, the state of Georgia, and the entire Southeast. The public health scenario is changing along with it. Jennifer Hirsch of International Health at RSPH has studied the burgeoning Hispanic community of Atlanta for six years and is disturbed by much of what she has learned. "La mano de obra (the hand of the worker) is a well-known Mexican phrase," she says. "A Mexican consul once said: 'America wants the mano, but they don't want the whole body.' That statement stuck with me... "People think it's fine that they're here as long as they're plucking our chickens, building our houses, and washing our clothes, but we're not helping them lead healthy lives. They can't get driver's licenses. They can't get emergency Medicaid for prenatal care. They can't get any routine medical care at all if they're undocumented. But it's illegal immigration that allows us to buy a head of lettuce for $1.19. People should know that there's blood on that lettuce. Our incredibly high standard of living is predicated upon the availability of migrant labor, illegal and cheap. Once they're citizens, it's much more difficult to exploit them in the same way." The US Census Bureau reports that in 2000 about 435,000 Hispanics lived in Georgia, about four times the number counted in 1990. Demographers, however, estimate the 2000 figure to be as high as 750,000 when undocumented residents are included. Either way, the Hispanic population is booming. Hispanic births jumped from 7.1% to 10.5% of all births in Georgia from 1995 to 1998. Although many Hispanics have settled here legally and permanently, most still suffer the daily uncertainty of life without a green card. The public health issues associated with this group are severe: No Medicaid or health insurance. No one who speaks Spanish at the hospital or clinic. No job training. No Workers' Compensation for on-the-job injuries. A host of social factors predisposes them to disease, death, and disability. The consequences are devastating and far-reaching.
In Our Own Backyard Jorge Simmonds Diaz, MD, 93MPH, was passing a Saturday afternoon quietly at home last winter when he received an urgent phone call from a neighbor. "A Latino roofer had fallen off a house just down the street from my house and was impaled by part of the scaffolding," he says. "A post went right through his face and into his brain. I ran down the street to help, but by the time I arrived, his co-workers had pulled out the post, and the man was bleeding profusely. He was still conscious, but he couldn't speak. I had him lie down, and I raised his legs to improve the circulation and cleared his airway. I performed emergency measures until the ambulance arrived, but he died four days later in the hospital. He was only 18."
Simmonds, a veteran of one of the busiest emergency rooms in Miami, tears up and shakes his head sorrowfully when telling the story. Director of Occupational Health and Safety for the DeKalb County Board of Health, he knows such injuries can be prevented. "Falling is the number 1 cause of occupational injury for Hispanics in DeKalb County and nationwide," he says. "Most of the migrant Hispanics in Atlanta work in construction. Usually contractors hire subcontractors for the work because they're cheaper. And subcontractors are cheaper because they hire undocumented workers. And because illegal immigrants won't usually apply for Workers' Compensation, contractors can evade responsibility for workplace injuries." The roofer who fell to his death in Simmonds' neighborhood is not an isolated case. From 1996 to 1998, a 40% increase in Hispanic fatalities in the construction industry accompanied a 20% increase in Hispanics in the construction workforce, according to a recent National Safety Council report. Accidents other than vehicle accidents are the most common cause of death for Hispanic men in the United States between the ages of 25 to 44, according to the National Vital Statistics Report for July 2000. For his MPH thesis at RSPH, Simmonds studied 101 Hispanic workers who gathered on street corners each morning on Buford Highway, waiting for someone to come by and offer them work for the day. His study was dubbed the "69-cent study" for the price of the coffee he often offered workers in return for completing his survey. His results are revealing and similar to national findings about the health status of Hispanic migrants. "They come here with one goal: to earn money," says Simmonds. "For reasons of desperation, language barriers, or lack of education, they don't pay attention to matters of safety. Because they are undocumented, they're not going to expect much from their employers either. One day they do landscaping, the next construction or carpentry, the next cleaning, and so on. They have no continuity to their work—no time to gain skills and learn safety measures."
"These men are lonely and homesick," says Simmonds. "They're very far away from their families, and they live in very unstable conditions from one day to the next." Far from Home
"So far, of the 200 men in our survey, about half engaged in sex while here," says Hirsch. "We are looking at health within a political and economic framework—not only at the individual behaviors that place them at risk for HIV. Sure, they get HIV because they have sex, but if they were at home, they could have sex with their wives. What actually puts them at risk for HIV is that they're here building our lovely houses and planting our seasonal flowers." When a married man contracts HIV during his time in the United States, he invariably brings it back to his wife in rural Mexico.
Susan Martorell, who has worked as a volunteer translator at Grady and other hospitals, agrees. "It is not unusual for children or taxi drivers to be used as interpreters in local hospitals," she says. "I recently heard a radio advertisement for a taxi company offering to drive people to the hospital and interpret for them once they got there. A hospital would never take anyone off the street to be a nurse. A patient is not going to tell their doctor about their sexual partners through a taxi driver who might be driving their neighbor or relative next week. Taxi drivers have no background in medicine, no training, no obligation of confidentiality. Yet this situation is so common." Federal law requires that every patient seeking care at a federally funded hospital or clinic be treated equally. "They cannot fail to serve someone just because they don't speak English," says Martorell. "Title VI of the 1963 Civil Rights Act guarantees that people of limited English proficiency receive interpretation and translation services." Martorell teaches medical Spanish to Emory medical students and is president of the Medical Interpreter Network of Georgia. The group is advocating for the state to adopt a formal policy requiring interpretation/translation services at Department of Health and Human Services facilities. Lawsuits in California, Oregon, and other states resulted in creation of such policies there. And before leaving office, former President Bill Clinton issued an executive order stating that the Office of Civil rights has a clear right to enforce translation standards.
Hirsch is the great-grandchild of immigrants who fled the pogroms in Russia and settled in the United States. "I was born with a lot of opportunities. We live in a global community now, but we don't all get an equal shot. Working in public health is a means to address that." A growing network of people with RSPH connections are working hard to study the health needs of Hispanic immigrants in Georgia and make sure they are met. Hirsch routinely places her students in internships and research studies associated with the Atlanta Hispanic Health Coalition, a group of health and social service workers that work with the local Hispanic community. A joint law/public health student is now working with the Office of Civil Rights to improve translation services in local hospitals. Another student is studying the HIV-risk behavior of gay Latino men in a collaborative project with AID Atlanta. "We have a lot of students who speak Spanish, and the needs in the service community are huge," says Hirsch. "Many workers in the community don't have the skills or the time to do research. This is a great opportunity for students to practice what they learn and contribute to an urgent public health need at the same time." The Mexican immigrants Hirsch works with sometimes ask her why she cares about them so much. "Every time I've been to Mexico, people have been incredibly hospitable and gone out of their way to make sure that whatever I'm doing works out," she says. "People welcome me and are just lovely. At the very least, I owe them a fair shake when they come to the United States. Here, we're all children of immigrants. Some immigrants have just had a more difficult time than others."
A Matter of Justice Juan Perez is quiet, soft-spoken, his eyes often downcast. He appears accustomed to blending in, to fading into the woodwork. But things have been looking up for him since he arrived in the United States. For the first time in his life, he eats three square meals a day and makes a living wage—$1,300 a month as a dishwasher. He lives in a one-room apartment in Roswell with eight other men and sends most of his income back to his wife in Mexico. He's very pleased that his 17-year-old son, his only child, recently joined him. He literally beams when his doctor, Carlos del Rio, enters the room, shakes his hand, and asks how he's feeling in Spanish. Franco and Del Rio examine his lesions, discuss his white count, and watch him swallow his monthly antibiotic. Perez is in good hands. When the exam is complete, Franco reminds him to take his daily medications and keep his bedclothes clean. He slips him a twenty and phones a Latino taxi company to take him home. "I really want to help these people," says Franco as he watches him leave. "They're so nice, so helpful, and so hard-working. And they have so little. They deserve better." Photos of Mexican scenes courtesy of Jennifer Hirsch
Eric Ottesen Interview | Age-Old Questions | Alumni News | WHSC | RSPH Copyright © Emory University, 1999. All Rights Reserved. Send comments to hsnews@emory.edu. |