Moving Forward
The company line
One giant laboratory
No more chicken scratch
Hard evidence
Physician, evaluate yourself?
What price security
EHCA realigns
Milestones


Hair today
grown tomorrow?
It's easy to spot your friends, neighbors and co-workers who've exhausted their follicular cell allotment in life. Some despair over a thinning pate; others make the best of nature with the trendy totally bald look.
Hair has a natural growth cycle of dormancy and renewal. Each time a hair falls out, a new hair follicle forms. People are born with a fixed number of follicular stem cells within each follicle that are responsible for this hair recycling process.
Soon there may be an alternative to baldness when your supply of follicular cells is depleted. Tissue engineering for hair replacement is a hot strategy being pursued by Aderans Research Institute, one of six biotechnology companies at Emtech Bio on Emory's Briarcliff campus. Scientists at Emtech are seeking answers and cures to some of the most challenging conditions and deadly diseases of our times -- from hair loss to lung disease to AIDS.

The company line
By Holly Korschun
Inside the seven modest yellow modular units tucked behind the Candler Mansion on the edge of Emory's 42-acre Briarcliff campus, scientists are quietly brewing innovative technologies designed to understand, prevent, diagnose, and cure some of the most widespread and challenging diseases and conditions of our time. From AIDS vaccines to nanobeads to replacement hair follicles to gene-based drugs, the six companies of Emtech Biotechnology Development (Emtech Bio) hope to nurturetheir fledgling business ventures, then give them the wings necessary for commercialization and distribution within the wider world of big pharma and larger biotech companies.
Three years ago, when Emory purchased the Georgia Mental Health Institute property on Briarcliff Road from the state, a biotechnology incubator was to be a cornerstone of the new campus. The start-up biobusiness development center would be operated by Georgia Tech and Emory, with support from the Georgia Research Alliance (GRA) and the state-sponsored Advanced Technology Development Center (ATDC), headquartered at Georgia Tech. The new incubator was designed to create bridges between the universities and local industry.
Although slow to get off the ground, Emtech Bio has emerged as a solid life-sciences incubator. Emory and Tech are still joint partners, the modular units are owned by Tech through GRA, and Emtech leases the land from Emory. GRA has funded some shared equipment, and the start-up companies sublease the facilities. Emtech holds a small equity position in some of the start-ups in exchange for a reduction in rent. Overflow companies from the Emtech campus also can occupy space at the ATDC, which this summer moves to Georgia Tech's new Technology Square campus in midtown.
Emtech's new CEO, Lee Herron, is an Atlanta entrepreneur with a 17-year track record as founder or team member of five start-up life-science companies. He manages Emtech through a contract with ATDC, where he is associate director for biosciences. Connie Snipes, facility manager since Emtech's inception, serves as full-time on-site administrator. The primary goal of Emtech is not for Emory and Tech to make money, but to develop the intellectual property of the universities and boost the commercialization of promising research for the benefit of patients and the state's economy.
Aderans Research Institute is a new branch of Tokyo- based Aderans -- the largest manufacturer of wigs, hairpieces, and toupees in the world. Aderans recently purchased Bosley Medical - a large US surgical hair restoration company - and tissue engineering start-up BioAmide, an early Emtech company originally based on bone replacement technology developed by Tech faculty member Robert Guldberg.
based Aderans -- the largest manufacturer of wigs, hairpieces, and toupees in the world. Aderans recently purchased Bosley Medical - a large US surgical hair restoration company - and tissue engineering start-up BioAmide, an early Emtech company originally based on bone replacement technology developed by Tech faculty member Robert Guldberg.
Now Aderans is pursuing tissue engineering hair replacement strategies at Emtech and University of Pennsylvania. During hair's natural growth cycle of dormancy and renewal, a new hair follicle is formed each time an old hair falls out. Each hair follicle contains stem cells that induce formation of new hair follicles. By microdissecting biopsied follicles from the back of the head that are resistant to the balding process, expanding the follicular stem cells in culture, then implanting them in the front of the head, Aderans hopes to create new hair follicles that will grow new hair.
At GeoVax, one of the most exciting developments at Emtech![]() is unfolding as some of the top researchers in the world take important steps closer to an AIDS vaccine. The company was founded by the Emory Vaccine Center, Yerkes microbiologist Harriet Robinson, and GeoVax CEO Don Hildebrand. GeoVax has exclusively licensed technology for an AIDS vaccine developed by Robinson and colleagues at the NIH and CDC. More than 11 years of laboratory research supports development of a two-part vaccine that began a Phase I clinical trial in January at three US sites, sponsored by the NIH Vaccine Trials Network.
is unfolding as some of the top researchers in the world take important steps closer to an AIDS vaccine. The company was founded by the Emory Vaccine Center, Yerkes microbiologist Harriet Robinson, and GeoVax CEO Don Hildebrand. GeoVax has exclusively licensed technology for an AIDS vaccine developed by Robinson and colleagues at the NIH and CDC. More than 11 years of laboratory research supports development of a two-part vaccine that began a Phase I clinical trial in January at three US sites, sponsored by the NIH Vaccine Trials Network.
During preclinical trials in rhesus macaque monkeys at Yerkes Primate Center, the vaccine has successfully controlled infection and prevented clinical AIDS in 23 of 24 primates for nearly three years. The two-part regimen consists of a multiprotein HIV DNA priming vaccination followed by an HIV recombinant pox virus booster vaccination. This first, one-year clinical trial in 30 patients will assess the safety of the DNA vaccine among HIV-negative volunteers. Another clinical trial will focus on the safety of the booster vaccine, and additional trials will test the combined regimen for both safety and effectiveness.
GeoVax plans to develop and test HIV vaccines targeting the viral strains prevalent in the United States and other countries. GeoVax has received more than $2 million in investor funding and is currently seeking first-round financing to support continued development of vaccines and clinical trials.
GeneRx+ came to Emory last year along with pulmonologist  Kenneth Brigham, who moved here from Vanderbilt University. Brigham also brought his expertise in developing new therapies for chronic and acute lung diseases. Founded in 1998, geneRx+ is developing seven gene- and protein-based drugs to prevent and treat respiratory diseases, including emphysema, pulmonary hypertension, cystic fibrosis, chronic bronchitis, and acute respiratory distress syndrome. GeneRx+ refers to its drugs as "gene-based therapeutics" rather than "gene therapy," because they do not permanently alter patients' genes. Instead, they introduce therapeutic proteins into cells or direct the patients' own cells to produce therapeutic proteins.
Kenneth Brigham, who moved here from Vanderbilt University. Brigham also brought his expertise in developing new therapies for chronic and acute lung diseases. Founded in 1998, geneRx+ is developing seven gene- and protein-based drugs to prevent and treat respiratory diseases, including emphysema, pulmonary hypertension, cystic fibrosis, chronic bronchitis, and acute respiratory distress syndrome. GeneRx+ refers to its drugs as "gene-based therapeutics" rather than "gene therapy," because they do not permanently alter patients' genes. Instead, they introduce therapeutic proteins into cells or direct the patients' own cells to produce therapeutic proteins.
Two of the drugs have proven effective in preclinical and early clinical trials and will soon enter Phase I trials. After early development, geneRx+ plans to license its drugs to larger pharmaceutical companies to pursue regulatory approval. Last fall geneRx+ formed a collaboration with Aradigm Corporation to study the feasibility of aerosol delivery of its gene-based drugs.
GeneRx+ research is carried out at Emtech Bio and at Emory's Whitehead Biomedical Research Building with Emory as academic partner and subcontractor in the company's SBTTR (Small Business Technology Transfer Research) and SBIR (Small Business Innovative Research) grants. Vanderbilt helped geneRx+ obtain $3.5 million in small business grants and holds all the currently licensed patents, but any new proprietary technology would be licensed to Emory. Emtech holds a small equity stake in the company in exchange for a portion of rent and other expenses.
Crystalplex Corporation (formerly Bioplex) has licensed  technology
invented by Emory and Georgia Tech biomedical engineer Shuming Nie, formerly
at Indiana University. Nie is developing nanoparticle quantum dots as
biosensor probes to trace specific proteins in cells for early cancer
diagnosis and to monitor the effectiveness of drug therapy. The biosensors
might profile genes and proteins simultaneously, allowing physicians to
individualize cancer treatments based on molecular variations. Crystalplex
has received seed funding from LaunchCyte, a biotechnology incubator located
in Pittsburgh.
technology
invented by Emory and Georgia Tech biomedical engineer Shuming Nie, formerly
at Indiana University. Nie is developing nanoparticle quantum dots as
biosensor probes to trace specific proteins in cells for early cancer
diagnosis and to monitor the effectiveness of drug therapy. The biosensors
might profile genes and proteins simultaneously, allowing physicians to
individualize cancer treatments based on molecular variations. Crystalplex
has received seed funding from LaunchCyte, a biotechnology incubator located
in Pittsburgh.
Design Science Research, a contract research lab  headquartered in Indiana, specializes in manipulating the solid-state structure of drugs, including the way they form crystals, to change their physical properties, such as changing the rate at which a drug dissolves. The company provides its research results and services to pharmaceutical companies. Former Emory chemistry graduate student Scott Childs, who now works for DSR, uses Emory's X-ray Crystallography Center to analyze crystals he grows in his Emtech lab. While readily available products from DSR are years from the pharmacy shelf, first-year results show great promise.
headquartered in Indiana, specializes in manipulating the solid-state structure of drugs, including the way they form crystals, to change their physical properties, such as changing the rate at which a drug dissolves. The company provides its research results and services to pharmaceutical companies. Former Emory chemistry graduate student Scott Childs, who now works for DSR, uses Emory's X-ray Crystallography Center to analyze crystals he grows in his Emtech lab. While readily available products from DSR are years from the pharmacy shelf, first-year results show great promise.
FOB Synthesis is both a drug discovery company and a  custom synthesis company. Woo-Baeg Choi, FOB founder and co-inventor of the AIDS drugs 3TC and FTC, along with Emory's Dennis Liotta and Raymond Schinazi, is working with seven colleagues to discover stronger antibiotics that can fight drug-resistant infections, including hospital-acquired superbugs. FOB partners with two Korean companies and also contracts with small biotech companies, large phamaceuticals (such as Johnson and Johnson), and Emory scientists to synthesize promising drugs.
custom synthesis company. Woo-Baeg Choi, FOB founder and co-inventor of the AIDS drugs 3TC and FTC, along with Emory's Dennis Liotta and Raymond Schinazi, is working with seven colleagues to discover stronger antibiotics that can fight drug-resistant infections, including hospital-acquired superbugs. FOB partners with two Korean companies and also contracts with small biotech companies, large phamaceuticals (such as Johnson and Johnson), and Emory scientists to synthesize promising drugs.
Emtech also awards seed grants to encourage Emory and Tech ![]() research with commercial potential. In January, awards went to Mark Feinberg, medical director of the Hope Clinic, to enhance the immunogenicity of HIV vaccines; to Brigham to develop an aerosol delivery system for gene-based drugs to treat lung disease; to pharmacologists Raymond Dingledine and Stephen Traynelis for drugs to block receptors responsible for brain damage during stroke and traumatic injury; to Tech's Athanassios Sambanis and Emory endocrinologist Peter Thule for research involving gene insertion into rat liver cells to allow them to produce appropriate levels of insulin to treat diabetes; and to biochemist Paul Doetsch to prevent and reverse degenerative processes induced by DNA damage.
research with commercial potential. In January, awards went to Mark Feinberg, medical director of the Hope Clinic, to enhance the immunogenicity of HIV vaccines; to Brigham to develop an aerosol delivery system for gene-based drugs to treat lung disease; to pharmacologists Raymond Dingledine and Stephen Traynelis for drugs to block receptors responsible for brain damage during stroke and traumatic injury; to Tech's Athanassios Sambanis and Emory endocrinologist Peter Thule for research involving gene insertion into rat liver cells to allow them to produce appropriate levels of insulin to treat diabetes; and to biochemist Paul Doetsch to prevent and reverse degenerative processes induced by DNA damage.
To learn more about Emtech Bio companies, see these web sites: www.crystalplex.com, www.generxplus.com, www.fobsynthesis.com, and www.aderans.co.jp/e/index.html.
More Moving Forward


Illustration by Joyce Hesselberth
One giant laboratory
Imagine research not bound by walls, campus boundaries, or state lines. A giant laboratory where investigators, regardless of geography, can enter each other's lab or clinic to share an idea, problem, unpublished manuscript, or clinical trial protocol.
Thanks to the largest, federally funded, three-year award for prostate cancer research in history, investigators at 13 universities in eight states will soon work together as if they were all located in one place. Using web-based technology, they will share data to find new ways to treat advanced prostate cancer.
With a $10 million grant from the Department of Defense Prostate Research Program, the Winship Cancer Institute (WCI) will develop the consortium over the next three years. Jonathan Simons, WCI director, and Leland Chung, director of molecular urology, are the primary investigators.
Participants will use web-based videoconferencing and online, real-time videostreaming data-sharing technologies, developed under a 2001 competitive planning grant award in which WCI researchers created a Virtual Corridor of Adjacent Programs (V-CAPs) to connect consortium team members. "To our knowledge, this infrastructure for real-time interaction across space is a first in prostate cancer research," Simons says.
Investigators are from Emory's WCI, Wayne State in Detroit, Johns Hopkins Oncology Center in Baltimore, Harvard Medical School in Boston, University of Texas Southwestern Medical Center in Dallas, Fred Hutchinson Cancer Research Center in Seattle, University of California at Davis, Memorial Sloan-Kettering Cancer Center in New York, UCLA Jonsson Cancer Center in Los Angeles, University of Washington School of Medicine in Seattle, University of Virginia, and Harvard/Brigham and Women's Hospital in Boston. Investigators include PhD-level basic scientists in tumor biology, bone physiology, molecular genetics, pharmacology, and biostatistics as well as urologists, pathologists, radiation oncologists, and medical oncologists.

NO MORE chicken scratch
Based on reports that about half of all medication errors begin with prescribing, Emory Hospitals launched its Medication Error Prevention Initiative (MEPI) in 2000 and standardized prescription writing to increase patient safety.
In the first year of the project, the total number of reported prescribing medication errors declined by 13%. And the percentage of prescribing errors detected prior to patient administration rose to 95.2% by November 2002, says William Bornstein, chief quality and medical officer at Emory Hospitals and medical director of Emory Healthcare Information Systems.
Now the MEPI team is working on "problem prone" abbreviations, says Tish Kuban, Emory Hospitals' pharmacy assistant director for sterile products and performance improvement. Although there is a list of approved abbreviations to use when writing a prescription, the list constantly changes and is hard to manage.
To cut down on potential errors, the MEPI team not only identified a group of abbreviations as high risk, but went one step further by getting professional service committees at the hospitals to agree not to use them. The MEPI team continues to work on identifying risky activities that could lead to potential errors and plans to implement additional patient safety projects in the future.
The Georgia Hospital Association recently recognized Emory Hospitals and Wesley Woods for the initiative and awarded Emory the 2002 Partnership for Health and Accountability Award for Quality and Patient Safety for Hospital Health Systems.


Hard evidence
Emory medical school faculty, residents, staff, and students are trying out and evaluating clinical guidelines that offer best practices in medical care for more than 100 medical conditions. They're using evidence-based medicine via a pilot project called EBM Solutions (formerly WebEBM).
The guidelines, many authored by Emory physicians, are on a private, password-protected website. Each topic includes a parallel guideline written specifically for patients to help them understand the recommendations and the underlying evidence.
Organizations licensing EBM Solutions' guidelines make them available to physicians and other health care providers, who can, in turn, make consumer-friendly versions of the guidelines available to their patients. Patients can also report on their understanding of and compliance with the guideline. There are also links to the evidence underlying the guideline so the user can find further information.
In 1999 Emory Healthcare joined four other academic health centers (Duke, Oregon, Vanderbilt, Washington University, and later Mt. Sinai NYU Health) to create the evidence-based guidelines. Many have been authored by Emory clinicians, working under the direction of Emory medical advisors: formerly William Bornstein, chief quality and medical officer at Emory Hospitals, and medical director of Emory Healthcare Information Systems, and currently Kimberly Rask, associate professor of medicine and health policy and management. Emory physicians continue to author new guidelines, update existing guidelines, and review guidelines written at other institutions.
Depending on feedback and use during the pilot phase, the license for the EBM content may be expanded to other Woodruff Health Sciences Center and Emory Healthcare users.
Authorized Emory users can obtain a password to the site by going to www.emory.edu/WHSCL/EBM.
For more information, contact Rask at krask@emory.edu or 404-727-1483 or Jon Saxton, special assistant for health policy and communications, at jsaxton@emory.edu or 404-778-4798. Or see the EBM Solutions website at www.ebmsolutions.com.

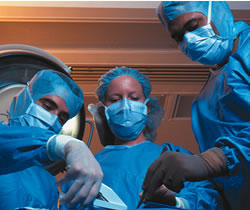
Physician, evaluate thyself?
That doesn't quite have the same ring to it as the old saying, "physician, heal thyself." Maybe there's a reason. When hospitals review patient outcomes, they usually use data collected by doctors who at best are too busy to devote their full attention to the matter and at worst are not disinterested observers.
That's part of the idea behind the National Surgical Quality Improvement Program (NSQIP). Developed to evaluate outcomes at VA medical centers nationwide, NSQIP was recently put to the test at Emory University Hospital (EUH), one of just three private medical facilities in the nation so chosen.
Unlike other mandatory report cards now being generated on hospitals and surgeons, NSQIP data is risk-adjusted for death and complications rates, says Aaron Fink, chief of surgical services at the Atlanta VAMC. "In most other outcomes studies, numbers or percentages don't reflect severity of illness or any complication of surgery. So quality institutions that treat the sickest patients might appear below par. Or surgeons who hesitate to take on complex, high-risk cases give the false impression that they are rendering good care."
NSQIP evaluations are based on detailed, impartial data. Surgical nurses not involved in patient care look at 40 preoperative and intraoperative clinical factorsfrom laboratory tests indicative of malnutrition or chronic illness to anesthesia risks to whether the case is a high-risk emergency. Researchers sort outcomes into 21 well-defined categories, such as wounds or respiratory problems.
"For example, we define exactly what is superficial and what is deep wound infection," says Fink. "Nurses don't have to make a judgment call about how to report a slight stain on a bandage." Patient outcomes are tracked for 30 days after a procedure.
NSQIP can predict the number of expected deaths or complications for patients with defined risks. Hospitals that score below the published accepted values reflect high quality of care; scores above signal concern and merit a call for change.
In the decade since the VA first implemented NSQIP, 30-day post-op deaths at the VA have dropped 27%. While part of the credit for the decline can be attributed to advancements in medical care, Fink believes that NSQIP's detailed analysis is also a factor. And he's confident that Emory and 15 other hospitals trying NSQIP can show a similar improvement over time. EUH did well in preliminary data, and the alpha trial proved that NSQIP analysis could be transferred to a more typical hospital setting.
To learn more, see www.NSQIP.org.

What price security?
New laws intended to boost homeland security may have major implications on Emory research -- in ways that go beyond restricting possession and transfer of "select agents" and toxins that could pose serious threats to public health and safety. They may affect how the university builds future labs and provides security as well as how researchers share information. The laws may also have a profound effect on Emory's growing contingent of postdoctoral students from other countries and on researchers from the Middle East.
The laws - specifically the Patriot Act, the Public Health Security and Bioterrorism Preparedness and Response Act, and the Agricultural Bioterrorism Act, as well as regulations proposed by the Centers for Disease Control and Prevention and the US Department of Agriculture (USDA) - went into effect in February. The Patriot Act criminalizes possession of select agents except for medical or clinical purposes or for "bona fide research" but does not define the latter.
Emory has identified 16 researchers studying three highly infectious diseases who will be affected by the act.
"To meet the requirements of the act, the culture at Emory will probably change on the health sciences campus," says Kris West, director of research compliance. Wherever certain biological or chemical agents (60 select agents) are used and studied, labs will have to be locked at all times with only approved users provided keys or card keys. It's possible that buildings themselves will be locked even during the day and that staff, faculty, and students will have to have card key access. Guards will be stationed outside designated labs and will be charged with searching all packages going in and out of those labs.
Anyone working in those labs, including some administrators, will be subject to security risk assessments by the US Department of Justice and must be approved by the Department of Health and Human Services or USDA every five years.
The new security and human guard requirements will be costly. In fact, the Association of American Universities says the cost of compliance in just one 1,000-square-foot lab at one university was estimated at $400,000.
Among the considerations are whether it is cost-efficient to maintain separate labs and separate security systems for the various select agents on campus or whether all such work should be combined in one controlled location.
"Does this mean we'll have to provide locks on cubicles in the future?" asks West. "We don't know yet whether we'll have to designate a building or a floor for those agents and researchers who are affected by the act."
Facing such troubling questions, a university-wide task force is studying the campus-wide implications for research and education. It is charged with determining how Emory will proceed to meet the requirements of the act and continue its building program, which in the past has emphasized collaboration in open labs.
While these new laws currently affect only a small number of researchers at Emory, as the university's vaccine work and other research continue to gear up, more people and their working environments probably will be affected.
The task force, headed by the Environmental Health and Safety Office and the Office of Research Compliance, is expected to come up with options and recommendations by this summer. For more information about the Patriot Act, see www.cdc.gov/od/sap.


Illustration © Tracy Walker/www.i2iart.com
EHCA realigns
EHCA, the joint venture between Emory Healthcare and HCA-The Healthcare Company, continues to evolve and shift its focus (See "Emory and Columbia/HCA open new doors," Spring, 1999 at www.emory.edu/WHSC/MOMENTUM).
Last year, Emory Cartersville Medical Center and Emory Northlake Regional Medical Center left the EHCA fold, returning to HCA. Emory Dunwoody Medical Center and Emory Eastside Medical Center, the two other hospitals currently operated by EHCA, remain in the joint venture.
The goal of the realignment, say EHCA chair Michael Johns, and HCA's Tom Gilbert, is to better direct resources and concentrate efforts on specific programs and services for the communities served by HCA, Emory, and EHCA. Both HCA and Emory Healthcare remain committed to the EHCA joint venture and say the changes will benefit the communities they serve.
The recent relocation of Emory's Family Practice Residency Program to the Emory Dunwoody campus exemplifies this mutual commitment. Capital improvements will include renovations and expansions of Emory Eastside.
EHCA plans to develop Emory Johns Creek Hospital, which will replace Emory Dunwoody Medical Center and the now-closed West Paces Medical Center. Restructuring will not result in the closure of any other hospital or the loss of any jobs. The management team of each facility will also remain in place.
The joint venture EHCA was originally formed in 1999 for several reasons, including the desire to work with managed care companies in contract negotiation and to compete with other networks that were being formed in the metropolitan area. Since then, there have been significant changes in the health care industry as well as in the competitive hospital landscape in Atlanta -- managed care contracting has become less exclusive and the strength of networks such as Promina has lessened considerably.
"During this time, EHCA has made some difficult decisions such as the closure of two facilities and the pending sale of Emory Peachtree Regional Hospital, events which have contributed to the need to make additional structural changes to the joint venture," says Gilbert. "Those considerations have led us to conclude that our primary focus is the north metro area which includes, among others, Dunwoody, Johns Creek, and the Snellville communities."

In this issue
From the director / LettersMed-morphosis
Burden of proof
Big Idea:
Regenerative Medicine
Moving forward
Noteworthy
On Point:
Smallpox, big risks?
MILESTONES
- A 42-year-old pharmacist no longer needs to give herself five insulin injections a day for her type 1 diabetes, thanks to Emory and Georgia's first islet transplant.
- Work began on a new Orthopaedics and Spine Center at Executive Park off of North Druid Hills Road. All orthopaedic outpatient services from The Emory Clinic and the Emory Sports Medicine and Spine Center will move to the 95,000-square-foot, five-story building in early 2004.
- The Agnes Raoul Glenn Building opened in January at Emory Crawford Long Hospital. The two-story building is devoted to radiation and medical oncology and staff training.
- After more than 30 years in trailers, the Emory Children's Center will get a new home next year. The School of Medicine is now designing a new $40 million pediatric building to be located on Ridgewood Drive, behind Children's Healthcare of Atlanta at Egleston and across from the Emory pediatric clinics.
- The state's first Cancer Center of Excellence opened at Grady Hospital early this year. As one of four regional centers planned by the Georgia Cancer Coalition, it will focus on the most common types of cancer in Georgia - breast, cervical, prostate, lung, and colorectal - and will seek to lower disproportionate cancer mortality rates among African Americans, the poor, and the uninsured.
- The Emory Autism Resource Center opened recently on the Emory Clairmont campus in a new 16,000-square-foot, $3.4 million facility. The center provides comprehensive services for children, adults, and their families.
- Yerkes National Primate Research Center broke ground in April for its new 92,000-square-foot, $27 million neuroscience building. The new facility is funded by a partnership of federal, state, and university resources, including two NIH grants for $2 million each and Georgia Research Alliance funds.
Copyright © Emory University, 2003. All Rights Reserved.
Send comments to the Editors.
Web version by Jaime Henriquez.