

| Spring 2008 | |||||||||
| Current Issue | |||||||||
| The eyes of others From Africa to India More than magnolias Secrets of a silent killer Moving forward Clinical care Comprehensive health care reform? From the Executive VP The last word |
|||||||||
| Past Issues Other Publications Contact Us Make a Gift WHSC home |
|||||||||
|
|||||||||
Breasts in 3D
In a clinical trial under way at Emory, researchers have found that stereo mammography, which presents a 3D picture of the breast, reduces false-positive readings by 49% compared with standard digital mammography. The standard mammogram presents only a two-dimensional image.
The new technology is also better at finding easily missed lesions, according to the research. The stereoscopic exam reduced the number of missed lesions by 40%.
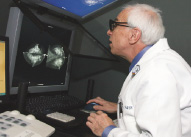
“Standard mammography is widely considered to be one of the most difficult exams to read because lesions may be disguised by normal tissue,” says radiologist Carl D’Orsi (pictured at left), director of breast imaging.
Breasts are made up of two types of tissues—fatty and parenchymal. The dense parenchymal tissue can obscure lesions on a standard mammogram. “Everyone has a different mixture of the two,” says radiologist Mary Newell, a collaborator on the study. “The density of a cancerous lesion is similar to that of parenchymal tissue, and the dense tissue may obscure the cancerous tissue. Essentially, we may be unable to see the forest through the trees.”
Standard mammograms also are more difficult because “we are taking a three-dimensional object—the breast—and making an image of it on a flat piece of film,” says Newell.
By contrast, during a stereo mammogram, two digital x-ray images are taken from two points of view. Each image is displayed on an LCD monitor and then arranged to form a “V” separated by a one-way mirror. The radiologist wears a pair of polarized glasses to view both images at the same time—similar to the experience of a moviegoer at a 3D IMAX film.
So far in this clinical trial, Emory doctors have taken both stereo and standard digital mammograms of 1,093 patients. All the patients are at elevated risk for developing breast cancer. Findings were reported at the annual meeting of the Radiological Society of North America in November.
Because the FDA has not yet approved stereo mammography, it is unavailable to the general public. –Kay Torrance
Kudos: The Emory Breast Imaging Center has earned the Breast Imaging Center of Excellence award from the American College of Radiology. The award recognizes Emory for the highest achievement in breast imaging by earning accreditation in mammography, stereotactic breast biopsy, breast ultrasound, and ultrasound-guided breast biopsy.

| ny | tiny font | ny |
| “Counting pixels is time-consuming and tedious, and many cardiologists don’t bother. However, it’s worth it.” —Dr. Leslee Shaw |
The pixilated heart
Are angioplasties effective long-term? A controversial heart study published in the New England Journal of Medicine (April 2007) left many doctors wondering if the gold standard in cardiac treatment was as effective as believed. But a new look by Emory researchers at a subset of patients from that study confirms that for the sickest heart patients, an angioplasty along with drug treatment is still the best option.
Cardiologist Leslee Shaw (pictured left) reviewed data on a subset of heart patients with moderate to severe ischemia—chest pain caused by the lack of blood flowing to the heart—and found a 33% reduction in ischemia in patients who received angioplasty and drug therapy. By comparison, patients who followed a course of only drug therapy had a 19.8% reduction in ischemia.
The larger, original trial—known as Clinical Outcomes Using Revascularization and Aggressive Drug Evaluation (COURAGE)—enrolled more than 2,000 cardiac patients with a full range of symptom levels. It found no difference in the rates of death, heart attack, or stroke between patients who underwent angioplasty or completed only drug therapy. Patients were followed between 2.5 and seven years. “The take-home message from the main trial was that a percutaneous coronary intervention, or angioplasty, could be deferred,” says Shaw. “Our substudy shows that a perfusion heart scan at one year is a good time to see if there is a need to go to more intensive measures.”
A perfusion scan, using single-photon emission computed tomography, measures blood flow to and from the heart and is more effective than angioplasty at giving a “whole heart health” picture by showing whether the arteries are in good shape, Shaw says. An angiogram shows the extent of blockage in an artery, but since the heart can develop new arteries to work around blockage, a patient can be better off than an angiogram indicates.
But it’s also essential that cardiologists read a perfusion scan properly. “It’s much more advanced and accurate to count the number of pixels lost on a heart scan,” Shaw says, as opposed to estimating the black space, which represents lack of blood flow. “Counting pixels is time-consuming and tedious, and many cardiologists don’t bother. However, it’s worth it,” says Shaw, pointing to a heart scan that seems to indicate 40% to 50% black space. In fact, a closer look at pixels shows a 28% lack of blood flow to the heart.
Numbers are a big deal: When a 5% blockage in blood flow is recorded, medical intervention is usually ordered. –KT
Kids count
The National Children’s Study will follow 100,000 children from birth to age 21 to learn to prevent and treat some of the nation’s most pressing health problems, including autism, birth defects, diabetes, and heart disease. Emory is one of only 22 centers and the only site in Georgia to participate in the landmark study, a collaboration between the U.S. Department of Health, including the National Institute of Child Health and Human Development, the National Institute of Environmental Health Sciences, the CDC, and the EPA.
Branching out
Emory is expanding its reach in West Georgia with an affiliation with Clark-Holder Clinic, a multi-specialty health care group based in LaGrange, West Point, and Newnan. The partnership will bring Emory clinical programs, new doctors, and technology to the region.
A new power tool for the arteries
Imagine a miniature device with a rotating blade, small enough to thread through a catheter. It tunnels to a blocked artery, located with a live x-ray and contrast dye. The blade spins and begins grinding away plaque. As the plaque particles break up, blood flows more freely from the heart to the legs and arms. The body easily absorbs the tiny particles, with no need for further removal of the plaque.
The whole procedure routinely takes only 60 to 90 minutes in an outpatient setting. Patients not only experience significantly improved blood flow but also may avoid the need for more invasive surgeries.
“As we remove the plaque, we often see a patient’s foot change color and feel it warm up,” says endovascular cardiologist Gregory Robertson, who performs the outpatient treatment at Emory Crawford Long and Emory Johns Creek hospitals.
The hospitals are among the first in the country to offer the treatment to people with peripheral artery disease (PAD). Affecting 8 to 12 million in the United States, PAD occurs when plaque builds up on the inside walls of the arteries, causing pain and numbness, impairing the ability to walk, increasing the chances of getting an infection, and, in extreme cases, leading to amputation. However, the condition can close an artery by 60% before any of these symptoms present themselves.
Another Emory cardiologist, Khusrow Niazi, was involved in the multi-center research study that first tested the safety and effectiveness of the new technology, which, unlike stents does not stretch the vessel wall. Twenty-four patients at Emory Crawford Long underwent the procedure, which helped the FDA decide to approve the device.
Patients with diabetes or renal failure or who are heavy smokers are the best candidates for the procedure because their blockages lead to heavy, calcified plaque build-up. “It is ideal for patients who have heavily calcified plaque blockages, which other technology cannot remove because the calcification is too hard,” says Niazi.
A PAD primer
If diagnosed with peripheral artery disease, what should you do? Greg Robertson recommends lifestyle changes that could make a difference.
- Stop smoking.
- Eat a low-fat, low-sodium diet.
- Increase exercise under a doctor’s care.
- Manage health problems such as diabetes, high cholesterol, and high blood pressure.
- Practice good foot and skin care by examining legs and feet every day and applying moisturizing cream to prevent dry skin.
Womb effects
Emory researchers are the first to precisely compute the overall amount of radiation that mammograms deliver to the entire body, a finding with important implications for pregnancy. If a woman had a mammogram while pregnant, the radiation dose to the fetus would be miniscule, equal to no more than a couple of days of background radiation naturally encountered. The study is published online in Radiology (February 2008).

Not your normal arm twisting
Each year, more than 700,000 Americans suffer a stroke, and the consequences can be devastating—85% of survivors experience partial paralysis and must be retrained in simple daily tasks.
But a new physical therapy tested by Emory doctors is giving stroke patients significant improvement in the use of their affected limbs. In the EXCITE (Extremity Constraint-Induced Therapy Evaluation) clinical trial, patients had their “good” hand or arm restrained to encourage their use of the affected extremity. They then were tested in daily repetitive tasks such as opening a lock, turning a doorknob, or pouring a drink.
“The basic principle behind constraint-induced therapy is re-teaching a patient to regain use of his or her impaired limb by limiting their use of the good one,” says Steve Wolf, a rehabilitation specialist at Emory. “Often, stroke rehabilitation has focused primarily on teaching patients how to better rely on their stronger limbs, even if they retain some use in the impaired limbs—creating a learned disuse.”
Researchers found that over the course of a year, the constraint-induced group showed a 52% reduction in the time needed to complete a simple task versus a 24% reduction in a control group. They also found a 24% increase in the proportion of tasks performed more than half of the time with the partially paralyzed arm in the constraint-induced group. The control group only showed a 13% increase.
Two years after the start of the constraint-induced therapy, stroke patients with mild to moderate impairments substantially regained use of their upper limb function. They had an improved quality of life with greater participation in social activities and better overall physical function, according to the study.
This research, led by Emory with the participation of seven centers, was the first national, randomized, single-blinded study to test the therapy on patients who previously had not experienced a stroke and who were enrolled within three to nine months after the stroke. It was presented at the 2007 annual meeting of the Society for Neuroscience in November. Previous research on constraint-induced therapy has been confined primarily to chronic stroke patients, according to Wolf. –KT
Back to Top | WHSC home
© 2008. Emory University, All rights reserved.