














|
 |
 |
A
new palliative care program
Mutant plants to the rescue
Gleevec for smallpox?
Nanotechnology funds for cancer
Treating (and preventing) injuries in Mozambique
Bernstein wins Novartis Prize
New blood vessels in the heart, thanks to gene
transfer
A
big breakthrough in curing diabetes, with the help of pigs and
monkeys
Clues about ketogenic diet and seizures
|
Cystic
fibrosis has an older face
On the rebound: more clues to bone loss
More than happiness: the science behind satisfaction
Why response to therapy varies in rheumatoid
arthritis
Mental health for the homeless
Trials against cancer
Time for a commercial break: incentive to invest
in new technologies
Faculty Leadership |
 |
 |
 E-mail to a friend
E-mail to a friend  Printer friendly
Printer friendly |
 |
|
|
|
 |
A
new palliative care program
has
been established at both Emory and Emory Crawford Long hospitals,
focusing on alleviating suffering and improving quality of life
for patients who have a serious illness. Palliative care not only
relieves both the physical and non-physical suffering that accompanies serious illnesses
but
also addresses mental health and spiritual needs.
and non-physical suffering that accompanies serious illnesses
but
also addresses mental health and spiritual needs.
Staffed
by internal medicine physicians and co-directed by hospitalists
Stephanie Grossman and Melissa Mahoney, who are board certified
in palliative care, the program is part of a rapidly growing trend
in health care. Not to be confused with hospice care, palliative
care is appropriate for patients in any stage of illness, not
just for those approaching the end of life. The team includes
physicians, nurses, social workers, chaplains, and pharmacists.
Grady Hospital also has a palliative
care clinic for cancer patients, funded by a $200,000 grant from
the Lance Armstrong Foundation. |
 |
|
|
|
 |
| |
|
|
| |
Mutant
plants to the rescue
|
|
| |
Global
warming may have met its match. Emory researchers have discovered
a mutant enzyme that could enable plants to use and convert
carbon dioxide to sugar (3-phospho-glycolate) more quickly,
effectively removing more greenhouse gases from the atmosphere.
During photosynthesis, plants
and some bacteria convert sunlight and carbon dioxide into
usable chemical energy—a process that relies on an
enzyme called RuBisCO. While  RuBisCO
is the most abundant enzyme in the world, it is one of the
least efficient. RuBisCO
is the most abundant enzyme in the world, it is one of the
least efficient.
“All life pretty much
depends on the function of this enzyme,” says biochemist
Ichiro Matsumura. “It actually has had billions of
years to improve but remains about a thousand times slower
than most other enzymes. Plants have to make tons of it
just to stay alive.”
For decades, scientists have
struggled to engineer a variant of the enzyme that would
more quickly convert carbon dioxide. For the Emory study,
Matsumura and colleagues used a process called directed
evolution, which involved mutating genes, inserting them
into bacteria (in this case E. coli), and screening for
the fastest and most efficient enzymes produced by the mutant
genes.
Matsumura’s team then
added genes encoding RuBisCO to E. coli to enable the bacteria
to change carbon dioxide into consumable energy. They then
added mutated RuBisCO gene to the modified E. coli. The
mutations of the fastest-growing strains caused a 500% increase
in RuBisCO expression.
“We are excited because
such large changes could potentially lead to faster plant
growth,” says Matsumura. More plants using and converting
carbon dioxide more quickly means less pollution and greenhouse
gases. |
|
| |
|
|
|
 |
|
|
|
 |
| |
|
|
| |
Gleevec
for smallpox?
|
|
| |
 The
hallmark anti-cancer drug Gleevec may be effective in controlling
smallpox infections or treating the complications caused
by smallpox vaccines. Emory scientists administered Gleevec
to mice and infected them with lethal doses of the poxvirus
used to vaccinate against smallpox. They found that the
drug reduced dissemination of the virus and the mice survived.
The Emory investigators, led by pathology researcher Daniel
Kalman, tested Gleevec against poxviruses after their discoveries
about how the viruses interact with host cells on a molecular
level. The virus particles become encased in an envelope
that helps them evade the immune system, then travel to
the cell’s surface, where the enveloped viruses hijack
host-cell proteins, which allow them to detach and spread
to other cells. The
hallmark anti-cancer drug Gleevec may be effective in controlling
smallpox infections or treating the complications caused
by smallpox vaccines. Emory scientists administered Gleevec
to mice and infected them with lethal doses of the poxvirus
used to vaccinate against smallpox. They found that the
drug reduced dissemination of the virus and the mice survived.
The Emory investigators, led by pathology researcher Daniel
Kalman, tested Gleevec against poxviruses after their discoveries
about how the viruses interact with host cells on a molecular
level. The virus particles become encased in an envelope
that helps them evade the immune system, then travel to
the cell’s surface, where the enveloped viruses hijack
host-cell proteins, which allow them to detach and spread
to other cells.
Kalman and colleagues speculated
that Gleevec might be effective against poxvirus without
eliciting drug resistance because it inhibits the host cell
molecule, rather than the viral molecule. “It would
be hard for the virus to overcome blockade of a host cell
factor because it would have to completely change its virulence
program,” says Kalman. He believes the concept of
using anti-cancer drugs to treat microbial infections may
prove to be more generally applicable. “Many pathogens
use host molecules as part of their pathogenic program,”
he says. |
|
| |
|
|
|
 |
|
|
|
 |
Nanotechnology
funds for cancer
 The
National Cancer Institute (NCI) has selected Emory and Georgia
Tech as one of seven National Centers of Cancer Nanotechnology
Excellence. The Emory-Georgia Tech Nanotechnology Center for Personalized
and Predictive Oncology will function as a discovery accelerator
to integrate nanotechnology into personalized cancer treatments
and early detection. The
National Cancer Institute (NCI) has selected Emory and Georgia
Tech as one of seven National Centers of Cancer Nanotechnology
Excellence. The Emory-Georgia Tech Nanotechnology Center for Personalized
and Predictive Oncology will function as a discovery accelerator
to integrate nanotechnology into personalized cancer treatments
and early detection.
With the new designation, Emory
and Georgia Tech now have one of the largest federally funded
programs in the United States in this arena. The NCI grant is
expected to reach $19 to $20 million over a five-year period.
Nanotechnology is research and technology
at the atomic, molecular, or macromolecular levels, where particles
are measured with a nanometer equivalent to one-billionth of a
meter (or 100,000 times smaller than the width of a single strand
of human hair). It offers promise for earlier cancer detection,
personalized diagnostics for targeted treatment, and creation
of new drugs for metastatic cancers.
“Nanotechnology will eventually
apply to all cancers,” says Bill Todd, CEO of the Georgia
Cancer Coaltion (GCC). “However, this grant is focusing
on breast and prostate cancers, which represent compelling challenges
in cancer research.”
The center’s director, Shuming
Nie, an Emory faculty member and GCC Scholar, is leading collaborative
research to develop several kinds of nanoparticle probes, including
quantum dots, which are luminescent nanoparticles that can be
chemically bound to biologic particles such as antibodies or proteins.
Such dots therefore can act as markers to study protein interactions
in live cells or to detect diseased cells.
Jonathan Simons, outgoing director
of the Winship Cancer Institute, is co-principal investigator
of the grant.
This NIH support came on the heels
of other major NIH awards, including one for $11.5 million, again
to Emory and Georgia Tech, to Gang Bao and colleagues, who are
using nanostructured probes to detect cardiovascular plaques. |
 |
|
|
|
 |
Treating
(and preventing) injuries in Mozambique
If
a motorist is hurt in a car crash in Mozambique, it is likely
that the first person to tend to his or her injuries will be a
bystander or a taxi cab driver.
EMS systems like those that exist in the
United States to aid accident victims are “far beyond the
reach of most low-income countries,” says Scott Sasser,
assistant professor of emergency medicine. “What they need are simple and sustainable strategies
for improving prehospital care.”
medicine. “What they need are simple and sustainable strategies
for improving prehospital care.”
While much of the attention in global
health assistance is geared toward disease prevention and treatment,
WHO estimates that 5 million people worldwide die of injuries
each year—largely in developing nations.
Sasser, emergency medicine physician David
Wright, and surgeon Jana MacLeod have received a five-year, $675,000
grant from the Fogarty International Center of the NIH to establish
an injury control program in Mozambique.
“When I did ward rounds at
the Central Hospital Maputo, I discovered that 60% of the patients
we saw that morning were admitted with an injury-related diagnosis,”
says MacLeod. “For the general surgeon in such an environment,
up-to-date knowledge about appropriate evidence-based trauma care
is essential. Also, injury prevention will have a significant
impact because of the relative volumes of injury, compared with
other types of admissions to the Maputo hospital.”
Mozambique was selected as the site
of the program—which Sasser hopes will become a model for
other African nations—because, according to WHO, its government
was prepared to support efforts to reduce its “injury epidemic.”
Through a partnership between Emory and Mozambique’s University
Eduardo Mondlane, academic and clinical core medical faculty in
Mozambique will be trained in the principles of public health,
research methods, ethical principles, and safety promotion.
Sasser also is working with WHO
and the City Council of Maputo to improve prehospital care within
the city. His efforts are based on the recently published WHO
monograph, “Prehospital Trauma Care Systems,” of which
he was lead editor.
“Instead of buying 50 new
ambulances that can’t be maintained or providing advanced
training that existing technology can’t support, we look
at what can be done,” says Sasser, “such as teaching
basic first aid to interested community members.”
The Fogarty grant will support the
training of 10 fellows from Mozambique in trauma and injury control.
The fellows, mostly clinicians, will spend their first year in
Africa completing coursework, followed by stints at Emory’s
Rollins School of Public Health and the University of South Africa,
returning to Mozambique to put methods into practice. —Mary
Loftus |
 |
|
|
|
 |
| |
|
|
| |
Bernstein
wins Novartis Prize
|
|
| |
 Emory
pathologist Kenneth Bernstein was the 2005 co-recipient
of the Novartis Prize from the American Heart Association,
marking the second consecutive year that an Emory faculty
member has won the award. In 2004, the award, which honors
contributors to advancing knowledge of hypertension, vascular
disease, and cardiovascular disease, went to Emory cardiologist
David Harrison. Emory
pathologist Kenneth Bernstein was the 2005 co-recipient
of the Novartis Prize from the American Heart Association,
marking the second consecutive year that an Emory faculty
member has won the award. In 2004, the award, which honors
contributors to advancing knowledge of hypertension, vascular
disease, and cardiovascular disease, went to Emory cardiologist
David Harrison.
Bernstein and his colleagues
have been responsible for a number of important discoveries
about the link between the kidneys, blood pressure, and
cardiovascular function, including cloning and characterizing
the gene for the receptor for angiotensin II, the central
component of the process of blood pressure control. |
|
| |
|
|
|
 |
|
|
|
 |
| |
|
|
| |
New
blood vessels in the heart, thanks to gene transfer
|
|
| |
 Emory
Crawford Long Hospital is one of 32 sites participating
in a national study of experimental gene transfer designed
to stimulate new blood vessel growth in the heart. Researchers
hope this new treatment will restore blood flow to ischemic
areas of the heart in patients with severe angina due to
coronary artery disease and who have few or no remaining
treatment options. Emory
Crawford Long Hospital is one of 32 sites participating
in a national study of experimental gene transfer designed
to stimulate new blood vessel growth in the heart. Researchers
hope this new treatment will restore blood flow to ischemic
areas of the heart in patients with severe angina due to
coronary artery disease and who have few or no remaining
treatment options.
The procedure involves injecting
a special gene directly into the heart muscle in six places
through a specialized catheter. The goal is for the gene
to provide the heart with instructions to grow new blood
vessels.
The results of earlier phase
1 and 2 trials have been encouraging, according to cardiologist
Henry Liberman, who leads the study. |
|
| |
|
|
|
 |
|
|
|
 |
A
big breakthrough in curing diabetes, with help of pigs and monkeys
Islet
cell xenotransplantation presents a promising near-term solution
to the problem of critically low islet cell supply for people
with type 1 diabetes. Researchers from the Emory Transplant Center
have transplanted insulin-producing neonatal porcine islet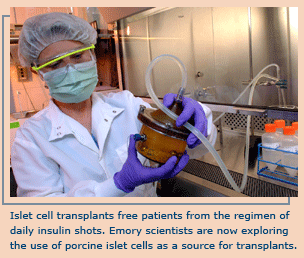 cells harvested by University of Alberta (Canada) researchers
into diabetic rhesus macaque monkeys, restoring the monkeys’
glucose control and resulting in sustained insulin independence.
cells harvested by University of Alberta (Canada) researchers
into diabetic rhesus macaque monkeys, restoring the monkeys’
glucose control and resulting in sustained insulin independence.
Islet cell transplantation has successfully
reversed type 1 diabetes in humans, but the availability of islet
cells limits use of this procedure in reaching more than 1 million
Americans with the disease. Each year, only 3,000 to 4,000 donor
pancreases are available, and each can produce enough islet cells
for, at most, only one transplant. “We must find new donor
sources to allow large-scale application of islet cell transplantation
in humans,” says Emory transplant researcher Chris Larsen.
Published in February in Nature
Medicine, this research also examines the effectiveness of
a costimulation blockade-based regimen developed by Larsen and
his colleague Thomas Pearson, which has fewer toxic side effects
than currently used immunosuppressive regimens.
Belatacept is a key ingredient in
the costimulation blockade that selectively blocks the second
of two cell signals the body needs to trigger an immune response.
This regimen is less complex than the immunosuppressant compounds
used in previous research, and its simplicity will make it more
applicable in clinical use.
In addition, Emory researchers addressed
concerns of the possibility of cross-species disease transmission
as a result of xenotransplantation. After extensive testing, they
found no evidence of transmission of porcine endogenous retroviruses
between the porcine cells and the transplant animals. The use
of nonhuman primates was critical for testing cross-species viral
transmission due to their close genetic link to humans, according
to Larsen.
The next step is to prove porcine islet
cells can be a source for human transplantation and to verify
the safety of the transplant procedures, a process researchers
hope to begin in the next three to five years. |
 |
|
|
|
 |
| |
|
|
| |
Clues
about ketogenic diet and seizures
|
|
| |
Physicians
have long prescribed a high-fat, calorie-restricted ketogenic
diet to prevent childhood epileptic seizures that are unresponsive
to drugs, but until now no one has understood why the diet
works. New studies at Emory show that the diet alters the
expression of genes involved in energy metabolism in the
brain, which in turn helps stabilize the function of neurons
exposed to the challenges of epileptic seizures.
To identify which genes might
be involved in this process, the Emory research team, led
by pharmacology chair Raymond Dingledine, used microarray
gene chips to examine changes in gene expression for more
than 7,000 rat genes. They focused on the hippocampus, finding
more than 500 genes that correlated with treatment with the ketogenic
diet, including genes involved in energy metabolism.
genes that correlated with treatment with the ketogenic
diet, including genes involved in energy metabolism.
To test whether energy reserves
in hippocampal neurons were enhanced with the diet, they
counted the number of mitochondria within cells, using electron
microscopy. They found that ketogenic diet treatment significantly
increased the number of mitochondria per unit area in the
hippocampus and concluded that the diet enhances energy
production in the hippocampus and may lead to improved neuronal
stability.
The researchers also tested
whether brain tissue affected by the diet would be better
able to withstand metabolic changes associated with seizures,
such as lowered glucose levels, because of enhanced energy
reserves. They found that synaptic communication in rats
on the ketogenic diet was more resistant to low glucose
levels.
This new knowledge could lead
to the development of more effective drug treatments for
epilepsy and brain damage. The researchers also believe
that the ketogenic diet should be studied as a possible
treatment for neurodegenerative disorders such as Alzheimer’s
or Parkinson’s diseases. |
|
| |
|
|
|
 |
|
|
|
 |
| |
|
|
| |
Cystic
fibrosis has an older face
|
|
| |
The
median age of cystic fibrosis patients has risen from 14
in 1969 to 35 in 2004, with almost 40% of today’s
patients already 18 or older. The Cystic Fibrosis Adult
Program at Emory is the only one in Atlanta geared to the
needs of adults living with the disease, which affects 30,000
people in the United States. The program is comprehensive,
assembling pulmonologists, gastroenterologists, nutritionists,
respiratory therapists, and others to serve more than 140
adults—the oldest of which is now in his mid-60s.
A multi-pronged translational research program including
studies on antioxidant production and lung inflammation
and the role of pollution and ultraviolet light exposure
helps researchers test multiple hypotheses simultaneously
to further increase the life span of those with cystic fibrosis,
says Arlene Stecenko, who directs the center and its research.
Center faculty also are examining the potential for gene
therapy and determining the molecular makeup of some 900
mutations of the cystic fibrosis gene and its functions. |
|
| |
|
|
|
 |
|
|
|
 |
| |
|
|
| |
On
the rebound: more clues to bone loss
|
|
| |
 Osteoporosis
may be caused by a “thymic rebound” resulting
from estrogen deficiency and increased production of the
protein IL-7, according to research led by Garland Herndon
Professor of Medicine Robert Pacifici and published in the
Nov. 2 online edition of Proceedings of the National
Academy of Sciences. Osteoporosis
may be caused by a “thymic rebound” resulting
from estrogen deficiency and increased production of the
protein IL-7, according to research led by Garland Herndon
Professor of Medicine Robert Pacifici and published in the
Nov. 2 online edition of Proceedings of the National
Academy of Sciences.
The research is based on earlier
findings suggesting a link between estrogen deficiency and
an increase in the number and activity of T cells. Increased
T cell activity also leads to increased levels of TNF, which
helps ward off infections but causes bone loss.
The Emory team discovered
a cause for the increase in T cells and TNF production:
reactivation of the thymus, which is where T cells finish
developing after differentiating from stem cells in the
bone marrow. The findings suggest a direct link between
the functioning of the thymus and bone loss.
Scientists have long believed
that the thymus is inactive after childhood, but Pacifici
and his colleagues found otherwise. Their data in mouse
models (and there is similar evidence in humans, says Pacifici)
showed that with estrogen deficiency the thymus surprisingly
comes back to life and starts pumping out new T cells.
Estrogen deficiency sets off
a chain reaction, he explains, triggering increased production
of IL-7, which causes production of new bone marrow stem
cells and reactivates the thymus. “This thymic rebound
results in a profusion of T cells, which in turn leads to
increased generation of TNF.”
While a thymic rebound may
be helpful to people dealing with immunodeficiency diseases
such as AIDS, the purpose in estrogen deficiency remains
unclear. “There are times for the thymus to come back
to life and make new T cells,” Pacifici says. “In
estrogen deficiency, there is no clear helpful reason for
that. It’s an unexpected phenomenon.” |
|
| |
|
|
|
 |
|
|
|
 |
More
than happiness: the science behind satisfaction
 Psychiatrist
Gregory Berns is curious about how the human brain works. In
his laboratory at Emory, he uses imaging techniques such as
MRI to study how the brain functions during tasks that have
a level of uncertainty, novelty, and even decision-making. His
curiosity and research have led him to develop a theory about
how people are motivated, which he explores in a new book, Satisfaction:
The Science of Finding True Fulfillment. Psychiatrist
Gregory Berns is curious about how the human brain works. In
his laboratory at Emory, he uses imaging techniques such as
MRI to study how the brain functions during tasks that have
a level of uncertainty, novelty, and even decision-making. His
curiosity and research have led him to develop a theory about
how people are motivated, which he explores in a new book, Satisfaction:
The Science of Finding True Fulfillment.
The book examines the drive that
motivates people, from running a marathon to maintaining novelty
in a relationship. “There were many activities that seemed
mysterious to me, the culinary magic of great cooking, Aha!
moments of intellectual stimulation, the fascination of self-inflicted
pain, the challenge of a crossword puzzle,” Berns says.
“The satisfaction of those pursuits appeared to derive
from doing something novel and tapped directly into the motivation
centers of the brain.
“Everything I have encountered
inside the research lab and out in the world suggests that satisfaction
is not the same as either pleasure or happiness, and searching
for happiness will not necessarily lead to satisfaction.” |
 |
|
|
|
 |
Why
response to therapy varies in rheumatoid arthritis
New findings by Emory researchers—that growth factors in
the immune system have both pro- and anti-inflammatory roles in
rheumatoid arthritis—help explain why some patients respond
to current therapy for this disease and others don’t.
Rheumatologists Cornelia Weyand
and Jorg Goronzy have helped delineate three different subtypes
of RA over the past 10 years (diffuse RA, germinal center synovitis,
and aggregate synovitis) and say that rheumatologists need to
develop diagnostic tools to 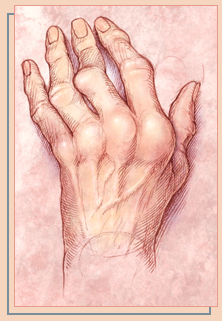 discern
differences among patients to help determine appropriate therapy.
Current therapies targeting inflammatory growth factors are applied
universally to all RA patients, without accounting for differences
in disease, even though not all RA patients respond well to these
therapies. discern
differences among patients to help determine appropriate therapy.
Current therapies targeting inflammatory growth factors are applied
universally to all RA patients, without accounting for differences
in disease, even though not all RA patients respond well to these
therapies.
In recent work, Weyand and Goronzy
used a humanized mouse model to study growth factors known for
helping B cells survive and differentiate. Two of these proteins,
known as APRIL and BlyS, are targets of new experimental drugs
currently in early-phase clinical trials.
The researchers implanted human
tissue from RA patients with the three types of disease into mice
engineered to lack a natural immune response. They then treated
the mice with a soluble receptor targeted to remove APRIL and
BlyS from the affected tissue.
They found that in the mice carrying
tissue from patients with germinal center synovitis, the inflammatory
process was halted. In mice carrying tissue from patients with
the other two types of RA, however, the opposite happened, and
the growth factors and inflammation increased.
“This is a very surprising
result,” says Weyand. “We found that these two factors
do more than just support the growth and differentiation of B
cells. They also can bind to T cells. In the tissues that had
worsening of the disease, we found T cells binding APRIL and BLyS,
telling us that these T cells had actually been suppressing the
disease.” |
 |
|
|
|
 |
| |
|
|
| |
Mental
health for the homeless
|
|
| |
Can
intensive case management, education, and coordination of
services for homeless people improve their mental health
and keep them off the streets? That’s the question
Emory psychiatrist Raymond Kotwicki is exploring with a
$250,000 grant from United Way of Atlanta. His Education and Community
Services Engagement Linkage (ECSEL) study will compare two
similar groups of patients who are randomized to either
a usual care group or an experimental group. Half of the
participants will receive the same care they currently get
at Grady Memorial Hospital, while the other half will receive
enhanced levels of case management and services.
grant from United Way of Atlanta. His Education and Community
Services Engagement Linkage (ECSEL) study will compare two
similar groups of patients who are randomized to either
a usual care group or an experimental group. Half of the
participants will receive the same care they currently get
at Grady Memorial Hospital, while the other half will receive
enhanced levels of case management and services.
“Those receiving care through ECSEL are some of the
leading users of expensive tertiary care such as psychiatric
emergency services and hospitals,” says Kotwicki.
“We hypothesize that the life support and case management
services provided to homeless people will cost taxpayers
less than safety net health services and jail.” |
|
| |
|
|
|
 |
|
|
|
 |
Trials
against cancer
Emory’s
Winship Cancer Institute is conducting some 115 clinicals trials,
including a number initiated at Winship.
Winship was the first cancer facility
in the country, for example, to open a trial of a new combination
of chemopreventive drugs for the oral cavity and larynx in former
smokers. Researchers are using a combination of erlotinib and
celecoxib to block epidermal growth factor receptor (EGFR) mediated signaling and to inhibit cyclooxygenase-2
mediated pathways.
factor receptor (EGFR) mediated signaling and to inhibit cyclooxygenase-2
mediated pathways.
Erlotinib blocks EGFR tyrosine kinase
protein messaging, which tells cancer cells to grow and divide,
and celecoxib is an anti-inflammatory that reduces cell formation,
blood vessel formation, and metastases. Individually, the drugs
have been found to be effective chemopreventive agents. This study
will evaluate the safety and effectiveness of the two drugs in
combination.
Winship is the only cancer facility
in Georgia offering a phase 2 trial for transitional cell carcinoma,
a common form of bladder cancer, testing the efficacy of the investigational
drug Vinflunine. Previous studies have shown that the drug exhibits
anti-tumor activity by inhibiting cell division. The purpose of
the trial is to assess whether it will shrink tumors or slow their
growth in patients with advanced bladder cancer that is worsening
despite chemotherapy.
Winship is one of only two cancer
research facilities in the country to conduct a procedure to determine
how much chemotherapy actually reaches certain kinds of brain
tumors. In the procedure, a microdialysis catheter is inserted
directly into the patient’s brain tumor. The patient then
receives an intravenous infusion of methotrexate. Researchers
use the catheter to remove fluid directly from the tumor. They
hope to determine exactly how much of the drug reaches the tumor by removing fluid for 24 hours
after the chemotherapy is delivered. Patients in the study have
recurrent, malignant, high-grade gliomas, one of the most difficult
types of brain tumors to treat.
much of the drug reaches the tumor by removing fluid for 24 hours
after the chemotherapy is delivered. Patients in the study have
recurrent, malignant, high-grade gliomas, one of the most difficult
types of brain tumors to treat.
Finally, Winship researchers participating
in a phase 3 multicenter, international study found that bortezomib,
one of a new class of drugs known as proteosome inhibitors, showed
promise against multiple myeloma, as reported in the New England
Journal of Medicine last June. Proteosome inhibitors are
designed to specifically inhibit the proteasome, an enzyme complex
in the cell responsible for breaking down a variety of proteins,
including many that regulate cell division. Unlike traditional
chemotherapy drugs, this drug works at the molecular level to
interrupt the mechanism that myeloma cells use to reproduce themselves.
It also has less impact on normal cells, says Winship hematologist
Sagar Lonial, one of the authors of the report. |
 |
|
|
|
 |
| |
|
|
| |
Time
for a commerical break: incentive to invest in new
technologies
|
|
| |
Emory
has established a new Investor Challenge Fund that will
provide a match for qualified investors who invest in promising
technologies discovered by Emory scientists. The eligible
technologies, including drug candidates, medical devices,
and diagnostic tests, will have the potential for commercialization
through licensing to start-up companies.
Emory already provides proof-of-concept
funding, in-house services for licensing new technologies
to companies, assistance for new start-ups in the creation
process, and some physical space for new start-ups. The
University also participates as a limited partner in venture
capital funds, such as the newly created $3.5 million Georgia
Venture Partners Fund, established by Emory, Georgia Tech,
and the University of Georgia.
“Supporting private
investment in our own research helps assure that the work
of our scientists reaches patients, where it can do good,”
says medical school dean Thomas Lawley.
The University has made big
strides in moving key discoveries from the laboratory to
the marketplace over the past decade. For example, Emory
has launched 35 start-up companies and currently has 24
licensed therapeutic products in various stages of drug
discovery, clinical development, or regulatory approval. |
|
| |
|
|
|
 |
| |
|
|
 |
Faculty
Leadership
 Richard
Cummings, an internationally known expert in glycomics,
is the new chair of the Department of Biochemistry. He comes to
Emory from the University of Oklahoma, where he was chair of molecular
biology. Richard
Cummings, an internationally known expert in glycomics,
is the new chair of the Department of Biochemistry. He comes to
Emory from the University of Oklahoma, where he was chair of molecular
biology.
Glycomics is the study of the carbohydrate
molecules produced by an organism, a major new research focus
identified by the NIH. Cummings has played a key role in the Consortium
for Functional Glycomics funded by the NIH. His research focuses
on glycoconjugates, the carbohydrate molecules and their associated
proteins that permit cells to communicate with and adhere to each
other—transmitting and receiving chemical, electrical, and
mechanical messages that underlie all cellular and bodily functions.
His research focuses on the role of glycoconjugates in cardiovascular
biology, autoimmune diseases, and parasitology.
 David
Stephens, Schwartzmann Professor, director of infectious
diseases, and executive vice chair of medicine, has a new title
and added responsibility as executive associate dean for research.
An expert on meningitis, Stephens heads a lab that has led international
efforts to define the molecular basis for virulence of bacteria
causing this disease. He helped found what is now the Georgia
Emerging Infections Program, a population-based laboratory surveillance
and clinical research program focused on bacterial pathogens.
He also led CDC’s clinical emergency response team in defining
clinical issues in prophylaxis, diagnosis, and treatment of anthrax.
He currently is principal investigator of the NIH-sponsored Southeastern
Regional Center of Excellence for Emerging Infections and Biodefense. David
Stephens, Schwartzmann Professor, director of infectious
diseases, and executive vice chair of medicine, has a new title
and added responsibility as executive associate dean for research.
An expert on meningitis, Stephens heads a lab that has led international
efforts to define the molecular basis for virulence of bacteria
causing this disease. He helped found what is now the Georgia
Emerging Infections Program, a population-based laboratory surveillance
and clinical research program focused on bacterial pathogens.
He also led CDC’s clinical emergency response team in defining
clinical issues in prophylaxis, diagnosis, and treatment of anthrax.
He currently is principal investigator of the NIH-sponsored Southeastern
Regional Center of Excellence for Emerging Infections and Biodefense.
 Stephen
Warren, chair and William Patterson Timmie Professor
of Human Genetics at Emory, is the new president of the American
Society of Human Genetics. He is renowned for groundbreaking genetic
discoveries, including the identification of the cause of fragile
X syndrome, the most frequently inherited form of mental retardation. Stephen
Warren, chair and William Patterson Timmie Professor
of Human Genetics at Emory, is the new president of the American
Society of Human Genetics. He is renowned for groundbreaking genetic
discoveries, including the identification of the cause of fragile
X syndrome, the most frequently inherited form of mental retardation. |
 |
| |
|
|
| |
|
|
|
|
|





