

Dean Thomas J. Lawley

A New Curriculum for the 21st Century
Adapted
from the Dean's State of the School Address, September 27, 2005
![]() would like to welcome all of you to our annual faculty meeting. It is
wonderful to see so many of our students as well as our faculty and staff
here. This is really a terrific turnout. It suggests to me that you are
interested in the topic. As the title of my presentation indicates, we
are going to spend most of our time discussing the future of medical education
at Emory. We stand on the brink of a wonderful new era that is ripe with
possibilities to create a model of medical education that will not only
make Emory distinctive but will set a new standard for medical schools
throughout the world. I could not be more optimistic, and I could not
be more enthusiastic about our work to reshape the curriculum.
would like to welcome all of you to our annual faculty meeting. It is
wonderful to see so many of our students as well as our faculty and staff
here. This is really a terrific turnout. It suggests to me that you are
interested in the topic. As the title of my presentation indicates, we
are going to spend most of our time discussing the future of medical education
at Emory. We stand on the brink of a wonderful new era that is ripe with
possibilities to create a model of medical education that will not only
make Emory distinctive but will set a new standard for medical schools
throughout the world. I could not be more optimistic, and I could not
be more enthusiastic about our work to reshape the curriculum.
I will lay out for you the thought process
and then the actual process we have gone through over the past two years
as we considered reformulation of our approach to medical education, culminating
in the redesign of our curriculum. But I want to make it clear that the
curriculum is not finalized. What you will see today are the recommendations
of various committees that have been working on your behalf. We want and
need your suggestions, comments, challenges, and respectful disagreements.
In the end, we need to reach consensus, and I have confidence that we
will. But before we do that, I want to emphasize three important accomplishments
for our school.
First, we have another outstanding M1 class.
They are among the brightest and most diverse classes that we have ever
admitted, and they have the highest average MCAT score (33.3) ever seen
in the school.
Second, our research enterprise continues
to grow and excel. As a school, we rank 19th in the amount of research
funding from the National Institutes of Health (NIH) for 2004 [up from
23rd for 2003 and 12 places higher than in 1996]. We have overtaken Vanderbilt
in the rate of growth of our NIH awards, and so we are ranked first in
the nation among the top 20 schools in growth.
Third, our faculty have been busier than
ever in terms of patient service. Last year, the faculty had more than
3.3 million patient visits at The Emory Clinic and Emory Hospitals, Grady
Memorial Hospital, Emory Children’s Center, and the Atlanta Veterans
Affairs Medical Center (VAMC). It is an astounding number and one that
grows every year, and I congratulate and thank our faculty.
Finally, I want to thank all of the faculty,
nurses, residents, staff, and students who gave and continue to give your
time providing care and resources to the victims of hurricanes Katrina
and Rita. You have done a marvelous job.

Dr. Micahel Johns
CEO of the Woodruff
Health Sciences Center


Dr.
Jack Shulman

Dr. William Eley
Now it seems axiomatic that medical schools should focus the majority of their time and resources on medical education, but we know that the realities of today’s academic medicine prevent that. We also know that superior education must be combined with superior research, clinical service, and citizenship.
When we began thinking about reinventing our curriculum, we had to ask ourselves why consider changing our current curriculum at all? Aren’t we doing very well? The answer is we are doing very well. We have a large and excellent applicant pool. We have outstanding matriculates. They perform superbly on the U.S. Medical Licensing Examination (USLME), where more than half of our class routinely score at or above the 90th percentile on Steps I and II. We have strong MD/MPH and MD/PhD programs. Our graduates match with top residencies and perform very well. In fact, some believe maybe we should leave well enough alone.
But some very strong and important indicators tell us that we could be doing better. Mandates from the Liaison Committee for Medical Education on curriculum content, student competencies, and student assessment indicate that we should teach and test competencies and introduce new concepts of adult pedagogy to replace long hours of sitting in class and listening to lectures. The massive expansion of scientific and clinical knowledge has led us to pack more and more factual material into the same amount of time.
Medicine is moving toward more outpatient care, and we have lagged behind the times. We live in a time of changing demographics with an aging population that has more and more chronic diseases, and the 80-hour work week has placed more stress on faculty as they work longer hours to make up for care previously provided by residents, leaving them with less time to teach.
The predominant lecture format of our curriculum is highly traditional and may not sufficiently emphasize the development of problem-solving skills. We have too little integration of course content, leaving us with inadvertent repetition or gaps. Our junior faculty put their hearts into teaching, but our students often never see the well-known senior faculty who attracted them here and will never know them as role models. We probably do not provide adequate exposure to longitudinal ambulatory care. Because we have lacked adequate facilities, we have had minimal use of standardized patients, simulators, and computer-assisted instruction.
As I thought about medical education in general and at Emory in particular and began an extensive series of readings and conversations with colleagues at other institutions, I became convinced that we should re-examine what we taught and how we taught it.
Two years ago, Dr. Jonas Shulman, our thoughtful and dedicated former Executive Associate Dean for Medical Education, and I began a review of the Emory curriculum. We also reviewed curriculum changes already under way at U.S. and British medical schools, and we made site visits to a number of other schools, including Harvard University, University of California–San Francisco (UCSF), and Stanford University. Dr. Shulman then held one-on-one discussions with more than 50 chairs and course leaders at Emory. We held discussions with medical students as well.
After this extensive but preliminary review, I initiated a leadership retreat. Dr. Shulman and Dr. William Eley, our current Executive Associate Dean for Medical Education, organized this retreat at Brasstown Valley Resort in September 2004 to discuss the type of graduates that Emory should produce, the curriculum that would be needed to produce these graduates, and the willingness to change if necessary. Participants at the Brasstown retreat included leaders of departments and courses, medical education deans, as well as representatives from the Nell Hodgson Woodruff School of Nursing, Rollins School of Public Health, and Emory College.
During the retreat, we discussed the characteristics that we desire in our graduates: integrity, passion, a willingness to “make a difference,” professionalism, enthusiasm for lifelong learning, curiosity, creativity, compassion, critical analytic skills, and leadership drive.
We also considered the knowledge and skills to be taught in our curriculum: a broad knowledge base; skills that integrate basic, clinical, behavioral, and population-based science; an understanding of the scientific method and its application to research and clinical medicine; the ability to work collaboratively with teams of health care providers; superior competence; and leadership skills.
Attendees urged and supported a change and recommended a significant overhaul of the curriculum, a new educational facility—seen as absolutely critical—and formal curriculum strategic planning.

Dr. Stephen Warren
Co-Chair, Curriculum Planning
Steering Commitee

Dr. Carlos del Rio
Co-Chair, Curriculum Planning Steering Commitee
 unique and a model for others. Co-chaired by Dr. Carlos del Rio
and Dr. Steve Warren, the committee included faculty and
department chairs, course leaders, deans, medical students, residents, and
representatives of the School of Nursing,
the School of Public Health, and the College.
unique and a model for others. Co-chaired by Dr. Carlos del Rio
and Dr. Steve Warren, the committee included faculty and
department chairs, course leaders, deans, medical students, residents, and
representatives of the School of Nursing,
the School of Public Health, and the College.The Steering Committee met with a series of internal consultants whom they chose to gather their thoughts and vision. The consultants included Provost Earl Lewis; Dr. Michael Johns, Executive Vice President for Health Affairs; Dr. Marla Salmon, Dean of the School of Nursing; Dr. James Curran, Dean of the School of Public Health; and Mr. Charlie Andrews, Associate Vice President for Health Sciences Space Planning and Construction. They also used four external consultants who had initiated or managed various kinds of curriculum changes, including Dr. Michael Whitcomb of the Association of American Medical Colleges, Dr. David Irby of UCSF, Dr. Emil Petrusa of Duke University, and Dr. Stephen Smith of Brown University.
The Steering Committee then developed a series of general recommendations for the new curriculum that they believed should center on the student, highly integrate course content, define and assess core competencies, be flexible, incorporate a house system that promotes vertical integration among students, provide substantial mentoring (believed by many to be a key to this whole enterprise), require a discovery phase, and emphasize ethics.
They also recommended the curriculum develop strong interactions with other Emory schools and other Atlanta institutions; expect student volunteerism; include leadership, scholarship, and public health as strong threads running throughout the curriculum; and make possible a tuition-free fifth year.
The Steering Committee then created 10 subcommittees to address and make recommendations about specific issues. Four subcommittees were formed to address the four major phases of the curriculum instead of the four traditional years of the curriculum. They also assembled subcommittees focused on information technology and simulation, mentoring, competency assessment, institutional interactions, and becoming a doctor. One subcommittee was composed totally of students, and students were represented on the nine other subcommittees as well.
After reviewing the recommendations of these subcommittees, the Steering Committee first agreed with the Brasstown Retreat recommendations and guidelines and strongly urged combined basic science and clinical curriculum planning. They divided the curriculum into four phases: Foundations of Medicine, Applications of Medical Sciences, Discovery, and Translation of Medical Sciences.
Some parts of the curriculum will vary in length, but everyone would go through the Foundations of Medicine phase and the Applications of Medical Sciences phase (see figure on page 5). The Discovery phase might be five to 10 months, or up to 22 months if the student opted for a tuition-free fifth year. Depending on the length of the Discovery phase, the Translation of Medical Sciences phase could be four to nine months for a student.
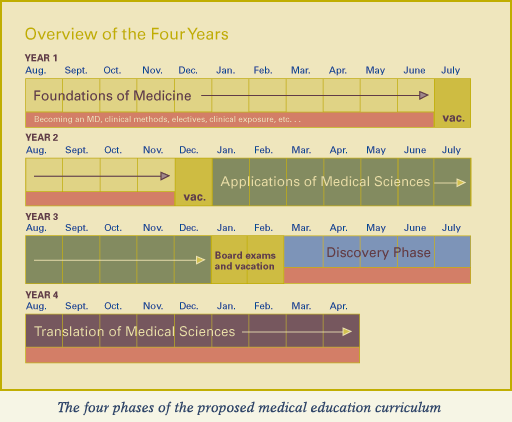
The Foundations of Medicine phase is conceived to be 15 months long. This phase starts with the whole patient and proceeds down to cells and molecules. To my knowledge, no other school in the United States has taken this approach. The reverse is common. This unique concept was originated by some of our basic science faculty, and I congratulate them on this innovation.
The content of Foundations of Medicine would be heavily case based. It would be taught by clinicians and scientists and be highly integrated. There would be strong public health and predictive health components throughout this phase. Small-group problem-solving would be emphasized. Early clinical experiences would be included from the first week or perhaps the first day. Students would work in health care teams, perhaps with nursing students or physician assistant students. Elective time would be available, and volunteer experiences would be expected.
Phase II. Applications of Medical Sciences
The Applications of Medical Sciences is envisioned to be 12 months long and would replace the traditional third year we have now. It would be divided into four or five major blocks. Each block would be preceded by a one-week intersession during which basic knowledge and clinical skills specific to the discipline would be presented. It would tend to maximize student time with clinical teams and not call them away from Grady or the VAMC to come back to campus. We intend to increase exposure to imaging throughout the year.
This phase also will emphasize scholarly activities. There will be student journal clubs, student clinical-pathological conferences, and perhaps even an Emory medical student journal. It will maximize faculty/student interactions and allow us to assess competencies using patients, objective structured clinical examinations, simulators, National Board of Medical Examiners testing, and oral exams.
Phase III. Discovery
Envisioned to be five to 10 months long for most students, the Discovery phase would be dedicated to scholarly pursuits, including basic research, clinical research, and public health. It may build on earlier experiences that students had as undergraduates or during their first two years of medical school. It will provide flexibility in time and place so that students can choose to complete the Discovery phase at Emory, other facilities in Atlanta, or institutions such as the NIH.
We hope this phase will use all of Emory’s resources and promote interactions with the Centers for Disease Control and Prevention and the Carter Center, for example, and that students will be carefully mentored. Students also need to be properly assessed, and they would need to know that we would have high expectations for them during the Discovery phase. A scholarly manuscript would be mandatory. All papers would be presented at student symposia, and papers could be published, for example, in the Emory medical student journal. All students would be encouraged to present at national meetings and to publish in peer-reviewed journals. And as I mentioned earlier, joint degrees would be possible, such as the MD/MPH or the MD/MBA, especially when combined with a fifth year.
Again, for most students, the Discovery phase would be five months. Those who pursue joint degrees could do a fifth year, and I would be glad to waive tuition for the fifth year. However, I cannot waive tuition in the School of Public Health or in the Goizueta Business School, so that would remain to be seen.

Now let’s focus on the Translation of Medical Sciences phase. Envisioned as four to nine months long, we believe it would assure good use of the M4 year and would include one-month subinternships in Medicine, Pediatrics, Surgery, or OB/GYN; a one-month Emergency Medicine rotation, and a Critical Care month. Electives could be as long as three to four months. Another one or two months for interviews or vacation could be factored in. And there would be a mandatory Capstone Course of one month.
The Capstone Course
The Capstone Course would come after Match Day and after the USMLE boards. For part of the course, the class would remain together; for other parts of the course, the class would be segregated into those going into medicine versus pediatrics versus surgery. In any event, there would be instruction in very recent advances in medical science. It would focus on the roles of a resident as a learner, as a teacher, as a caregiver. It would provide instruction on working with other types of health professionals, such as nurses, social services staff, and physical therapists. And it would address medical, legal, and economic issues; include cost-containment principles; re-emphasize ethics and professionalism; provide instruction on quality issues and reducing errors; and teach clinical pearls, perhaps even specialty-specific clinical pearls.
What I have described for you is a curriculum created by faculty and students and painted in very broad strokes. I agree with it. Blanks must be filled in. For example, we do not have details for the Foundations of Medicine phase, which is a major piece of our curriculum, and we do not have a building in which to teach it. But here is an outline of how we propose to get from here to there.
First, we are going to have more town hall meetings to engage faculty and students. There will need to be a final review by the Steering Committee. There will need to be acceptance of the report by myself and other members of our leadership team. We need to develop methodologies to assess the success of the new curriculum: How do we know it is working? How do we know it is better? And we need to begin specific detailed planning and piloting of some of the components that I have mentioned.
M1 students who enter in the fall of 2007 will participate entirely in the new curriculum. Students who begin their M4 year in the fall of 2007 will participate in the last year of the new curriculum. A new phase will be added each year as our 2007 entering class advances, and thus they will be the first graduating class—the Class of 2011—to experience all phases of our new curriculum. So you can see it is going to take a while for all of our students to be exposed to the new curriculum.

As William Butler Yeats said, “Education is not the filling of a pail but the lighting of a fire.” The School of Medicine has the opportunity to create a new standard for medical education—one that lights a fire in the individual medical student and in medical education itself. We are at a place in the history of our school where we have everything it takes to create this new standard, not just here at Emory but throughout the world. We can change the trend in medical education from pouring as many facts as we can into our medical students and then
 expecting
them to pour them back out in examinations, to allowing the patient to ignite
a sense of excitement and discovery in them and us as we all bring together
the art and science of medicine, all the way from the molecule to populations
biology.
expecting
them to pour them back out in examinations, to allowing the patient to ignite
a sense of excitement and discovery in them and us as we all bring together
the art and science of medicine, all the way from the molecule to populations
biology. To paraphrase Jean Piaget, the noted child psychiatrist, educator, and scholar, our principal goal should be educating young men and women to be capable of doing new things, not simply repeating what other generations have done; to be creative, inventive and discoverers; and to be critical and verify and not accept everything that they are offered. And, I would add, to be sterling examples of physicians and scientists and to conduct their daily activities with compassion, character, integrity, and professionalism.
As baseball legend Yogi Berra said, “We have deep depth.” As an aside, his message for our medical students is that you can observe a lot by just watching.
Now we will begin to fill in the gaps, writing in the blanks during the final stages of the shaping of our new curriculum. As we do so, I want each of us to turn from the intellectual exercise in which we have been engaged and begin thinking about how we can put ourselves into our parts of this new curriculum, whether our parts are large or small, and how each of us can light that fire using our own unique knowledge, interests, and skills.
Some of us are outstanding problem-solvers, small- and large-scale. Some of us have immense stores of highly specialized or technical knowledge that we apply in both usual and novel ways. Others of us generate that highly specialized and technical knowledge. Some of us are marvelous bedside teachers. Some of us focus on health policy and health care, global and local. Regardless of the area in which our star shines, each of us has something important to contribute to the education of our students.
We are all busy, some of us are stretched, but we came into academic medical centers because we love to teach and do science as well as care for patients. We now have a chance to pull it all together in a new and exciting and stimulating way that will be fun for us. I invite you to help us light this fire. In particular, I urge our senior faculty and department chairs to be involved in the teaching of our medical students and to be their role models along with our enthusiastic and vibrant junior faculty.
How many times have you remembered or recounted the words and deeds of a faculty member during your own medical education that helped you make the decisions and choices that shaped your life? I want all of us to give our students the chance to remember and be grateful to us at Emory. This is a once-in-a lifetime opportunity, and we must not fail.
Thank you very much.
Thomas J. Lawley, MD
Following the State of the School address, five members of the Curriculum Planning Steering Committee held a question-and-answer session with audience members. The panelists included Drs. Jonas Shulman, William Eley, Carlos del Rio, Neil Lamb, and Richard Nichols. Excerpts from the session follow.
Q. Dr. Ned Waller (Hematology/Oncology): The idea for a Discovery phase is great. But it seems to be modeled at least in part on what occurs at Duke, with the third year being a 12-month period, and Stanford, which has a fifth year for research activities. Are we creating conditions where our students are going to achieve less than they could with a Discovery phase of only five months for individuals who may have never engaged in research activities?
A. Dr. Shulman: Obviously, five months is too short for many kinds of scholarly activities. We do not envision everybody using that time as a way to begin an in-depth career in research. But it at least will give students a taste. When students start the Discovery phase, whether it is going to be a five-month or 10-month period, they will already have done a lot of legwork and are not starting from scratch on day 1. We thought about five years, but we did not think that was something we wanted to have every single student do. There will be students who do five years for sure, and we have many doing that now. But the Discovery phase at least assures that every single student will have an in-depth opportunity. We will have to see how that goes.
Q. Dr. Erica Frank (Family and Preventive Medicine): Could you talk about what parts of the curriculum will be uniquely Emory?
A. Dr. Nichols: One aspect that is uniquely Emory is that we were trying to face the problem of cramming basic sciences into an even shorter period than students are given at the present time. So we decided to be creative about it and propose a new idea of giving medical students a conceptual coat rack on which to hang all of the information they receive. The first phase—the Foundations of Medicine—would give them a conceptual framework for understanding the human body. We took a different approach by starting at the level of societal and environmental concerns, and the level of public health, and bringing some of the greater global issues into the educational process. Following some case presentations, we would begin teaching the conceptual framework of the human body, starting from the behavioral level by talking about tension, emotion, sleep, sexual behavior, everything that we do, and even get some of our humanities colleagues involved. We would then start to march down through the body through the major regulatory systems, the body, the organ systems and how they interact, and then finally end up at the cellular and molecular level and how the body interacts with its environment at the cellular and molecular level. That brings us back to public health and the environment, which closes the whole loop.
Following that period, we propose to have another major section that is the more traditional-based approach to diseases and organ systems, which will be organized more like traditional medical textbooks. This would give medical students a chance to reintegrate the cellular information with the global aspects of disease.
Q. Dr. Juha Kokko (Medicine): Who is going to do the teaching? It is incredibly labor intensive. And how are we going to pay for it?
A. Dr. Lawley: This curriculum is going to cost more money than we currently apply to our teaching enterprise. We estimate that it will cost an additional $4 million to $5 million per year. We already have budgetary shifts going on that will allow us to do this over the course of about three fiscal years That’s the easy part. The hard part is applying that appropriately. Everybody is expected to teach. However, there are some individuals who do an extraordinary amount of teaching. We need to be sure that individuals who are course leaders or mentors or who head up the house system we have proposed are compensated for what they do. And we will try to do it wisely.
Q. Dr. Bhagirath Majmudar (Pathology): The typical Emory medical student 20 years ago would come here primarily to be a good clinician, would reach out to the community and be a good doctor and reasonably good clinician. Those kinds of medical students are not applying to Emory today. For example, when I interviewed two medical students last year, I asked them, "What do you see yourself doing 15 years from now?" One of them said surgeon general. He was very serious. We will have to provide some kind of an outlet, which is individual-specific rather than group-specific, for students with different dreams and different ideas about being a doctor. The second concern I have is about teaching. If we are going to involve so many vigorous junior faculty, do we have to change our criteria of promotion?
A. Dr. Shulman: One of the most unique aspects of this curriculum is that it offers a highly individualized curriculum for every single student. In our report to the dean, we show four different types of students going through this curriculum as examples. One is interested in intra-urban care and begins working in a clinic and takes courses within the School of Public Health. We also describe a student who is interested in vascular biology and is spending time in the lab. By the time he hits the Discovery phase, he is able to do a minimum of 10 months or maybe even go for a PhD. There are a variety of possibilities within this curriculum, and the mentoring process is the glue that is absolutely necessary to hold them together.
A. Dr. del Rio: In the curriculum report, we are proposing to the dean and the chairs that we need to develop a clinical educator track, similar to the clinical track and the research track, that allows people to be promoted on excellence on teaching locally. Not the national recognition that will get you tenure, but the kind of teaching we need to carry out this curriculum. It is going to need a lot of student contact hours. And we need to be able to recruit and retain outstanding teachers and outstanding educators to carry out this curriculum.
Q. Dr. Randy Hanzlick (Pathology): How would anatomical dissection and traditional pathology be incorporated into this curriculum?
A. Dr. Lamb: I can give you a little more detail about the Foundations of Medicine phase, which incorporates the basic sciences. Anatomical dissection would begin in the fall. We feel that is something that needs to stand on its own. It is difficult to try to integrate that across the 15 months, partly because of the way dissection has to proceed by moving through certain parts of the body, and the challenges of dealing with cadavers over that long a period of time.
At the same time, students will start the human biology section. Before that, they will have spent a month in the case theater, which is modeled roughly on the way UCSF starts their students. There are four week-long cases that students follow from the moment a patient first experiences clinical symptoms, to hospital admission, surgery if necessary, follow-up care in the hospital, release from the hospital or clinic, and then continuing care. They will use these cases as a scaffold in physiology or biochemistry or the introduction to a certain organ system. Then they will begin human biology and anatomical dissection. They will have a three-week period in December when they are in a clinical setting, where they spend part of their time in clinical instruction and patient interaction, learning to be part of a hospital team, and part of their time actually on the wards functioning as that team. When they come back from winter break, they will continue human biology and then shift into the organ-based discussion of human disease. There is a one-month period in May where they have an elective. It can be public health. It can be business. It can be individual research. There are a number of options in that elective month that potentially set the stage for the student’s Discovery phase later on. That month can also be used for remediation if a student is struggling with issues in the first year.
Then there is a three-week period—and this also addresses the question about what is unique about our curriculum—where our students will be involved in serving an underserved population. Whether that's participating in a medical clinic in rural Georgia or working in a medical clinic in rural Uganda. We would partner with the CDC and the Carter Center to identify these needs worldwide and then move our students into these experiences. They are not just observing; they are part of the process. They come back and have their summer break. They continue the human disease section. Then they move into a mini Capstone that addresses everything they have covered in the first 15 months.
Q. Dr. Frank Anania (Medicine): The USMLE Steps II and III for our students can only get better in terms of their scores, given what you have presented to us. But how will our students do in the time capsule that is required to get through USMLE Step I? There are going to be a lot of things going on in the first 18 months. Since our students are now doing so well on USMLE Step I, how well do you envision they will do during the roll-out phase of this curriculum?
A. Dr. Shulman: When Dr. Lawley and I were at UCSF, that was one of the first questions we asked them. They had gone to compressing their curriculum in a similar way for the first part. As it turned out, their students had done exactly the same as they had done before. Their board scores and our board scores are very comparable. We do not want to see those scores drop too much because they do help our students get excellent residencies. But we cannot keep that idea as our main focus. What I would like to see, when I look at the Annals of Internal Medicine or the New England Journal of Medicine, is that three or four Emory students have published articles there. Or when I look at who is leading the Georgia state health department, it is one of our graduates. You have got to balance all that along with how students perform on the boards.
Q. Shveta Raju, (MD/MBA student): I learned during my third year of medical school that what really matters is how you treat patients. However, I was often disappointed in my residents. While the faculty were amazing and I learned many valuable things from them, my daily interactions were often shaped by residents who did not act the way I wanted to act. How can we empower medical students to treat our patients well and not get bogged down in the pressures of residency training?
A. Dr. Eley: That is one of our concerns. Dr. Lawley mentioned the 80-hour work week, which compresses the hours of the residents so much that they are struggling to get their work done. I know that their teaching has decreased. The faculty are now doing more work than the residents, and their teaching has decreased. One of the major threads of this curriculum is putting the students back together with our faculty and allowing the faculty to have time to teach. We cannot graduate ethical professional medical students unless we have ethical professional residents and faculty. We already have that. We have to find a way to teach them to teach, to find out how many people we need to teach, so that we can allow people to do their jobs in a humane way. It is going to take more money injected into the system for teaching. But a main theme of the curriculum is putting students back together with faculty who are practicing exactly that kind of medicine. If we do not do that, we have failed.
Q. Matt Wallace (M2 student): When you talk to people, the biggest criticism that patients, malpractice claimants, and even older doctors have is that doctors these days really do not have great interpersonal skills. They are just abysmal. They are very scientific and focused, and that gets a lot of people into trouble. As far as developing a competent bedside manner and interpersonal style, I do not see that in any of the objectives for the new curriculum. Where are students supposed to get this?
A. Dr. del Rio: Drs. William Branch and Joanne Williams chaired a subcommittee on Being a Doctor. What we are talking about is longitudinal instruction across the four-year curriculum that emphasizes the patient-doctor relationship. We envision interpersonal communication skills as part of this curriculum from the beginning. For example, from the first week, you would be assigned to an afternoon clinic. You would work with a doctor and learn interpersonal communication skills from the very beginning. There will be another series of scenarios for teaching interpersonal communication skills on how to relate to the patient, how to relate to the family, how to relate to the other colleagues. One of the most important interpersonal communication skills is how to deal with the health care team. Clearly, that is one of our most important goals.
Q. Sophia Topeman (M2 student): Have you considered making the fifth year an international year? A lot of students in my class are interested in international health and would really appreciate a year to go overseas and work in a country where health care is not as advanced as our own.
A. Dr. Eley: We already have students who are getting their MPH in international health and are traveling to Africa and other places as part of that experience. It is a very popular choice for MPH students. Will that fifth year be that? If we get this curriculum out there and people see how excited we are, there are a lot of opportunities in Atlanta for those kind of experiences.
A. Dr. del Rio: Atlanta has been called the public health capital of the world. We have the CDC, the Carter Center, CARE, and the Task Force for Child Survival and Development. A lot of students come here because of public health. While we do not want to turn every student into a public health expert, we want to give students an appreciation of global health and making predictive health a central theme of what students are concerned about. Whether they are going to be working on a molecule in the lab or they are going to be working in a clinic in rural Uganda, they need to understand the broader issues of public health, of population health, of predictive medicine. That will be a very unique feature of the curriculum.